Necrotizing fasciitis—why you should unlearn what you think you know
BY IAIN MCFADYEN
When it comes to severe soft tissue infections like necrotizing fasciitis, orthopedic surgeons are not usually the go-to experts. In many hospitals however, they are more likely than others to be called in to consult on patients with these potentially life-threatening conditions. That’s why Dr Iain McFadyen, an orthopedic trauma specialist at the University Hospitals of North Midlands in Stoke-on-Trent, United Kingdom, is calling on orthopedic surgeons to change their approach to these kinds of infections. Here, he shares the story of his most difficult case, an extraordinarily difficult surgery that ultimately became a career-affirming moment.
Bacterial skin and soft tissue infections are nothing much out of the ordinary. Conditions such as cellulitis, which is most commonly caused by group A streptococcus bacteria, often involve symptoms such as redness, swelling, or pain and are easily treatable with oral antibiotics.
However, in rare instances, cases that seem comparably manageable at first will rapidly deteriorate and develop into severe soft tissue infections. One example of these is necrotizing fasciitis, which you may have seen described in the media as flesh-eating bacteria. While the term may seem a little over the top, it is indeed quite a scary and horrific condition. It can spiral out of control very quickly and without specialized care, many patients with necrotizing fasciitis are likely going to die.
Interestingly, all over the world, it is orthopedic specialists who regularly find themselves being called in to consult on these kinds of conditions. The reason behind this is simple: in many hospitals, the surgeon who not only knows their way around limbs but is also most likely to be present at any given moment will often be an orthopedic consultant. So, when the acute medical team refers patients with aggressive and persistent soft tissue infections, they often land with us.
Soft tissue infections are obscure and dangerous
The problem is that as orthopedic surgeons, severe soft tissue infections are not really our bread-and-butter work. For most colleagues, I would assume that at best, life-threatening infections of this kind are at the periphery of their expertise. Come to think of it, I am not even sure that any surgeon could be called an out-and-out expert in this kind of infection, which after all is rather rare: even in big hospitals like the one I work for, only a handful of soft tissue infections each year will end up requiring surgical care.
But—and this is something I tell my residents over and over—we absolutely have to take those referrals seriously. We must try and get to the bottom of what the referring medics are worried about. Because if they call us in, they will have a very good reason to do so. They are not simply trying to offload cases. In fact, for every patient they refer, they will have seen 90 others that they do not. So, we must ask ourselves: what makes this one case so drastically different from the other 90 and how can we best help?
One of the main issues here is insecurity. I know that dealing with these relatively obscure infections can make some colleagues feel slightly apprehensive. But even the slightest resistance will open the door to them not getting it right. The fact that we get referrals from other teams and are not necessarily primarily responsible only aggravates the problem. I would like to describe how I have worked at overcoming that and why I think it is so important.
Expectations can be misleading
The case study I am about to describe is at the extreme end of the spectrum. But it is completely within the realm of what is possible. A few years ago, I was called in to consult on the case of a 41-year-old woman who was decidedly fit and healthy. She was not diabetic, her immune system was sound, she was not on radiation or chemotherapy, and she took neither steroids nor intravenous drugs. There were no major medical issues running in her family. In short, this was not the kind of patient you would expect this in. But expectations can be misleading, which is why it is patients like these that scare me the most.
According to the woman, her entire family including herself had at some stage in the preceding weeks had a strep sore throat. Just when she thought she was getting better, she began developing a pain in her calf. By the time she saw her family physician, the pain had become intense. But except for a little bit of pink discoloration, the calf looked normal. The doctor reasonably diagnosed her with cellulitis and prescribed oral antibiotics.
A few days later however, the patient felt worse. In her own words she felt simply terrible, like she had the worst flu imaginable. She went to the emergency room, where she was diagnosed with cellulitis once again. She was admitted to the hospital and put on intravenous penicillin. She was also given the usual range of lab tests that you would expect in a case like this.
Rapid deterioration and systemic toxicity
When the results came back, they did not look good at all: the patient had rising blood lactate levels as well as some organ dysfunction. Also, her kidneys were no longer working as they should. In short, she was showing systemic toxicity. The medical team made the right call at this point and requested an orthopedic consultant. And although this consultant did indeed take it seriously, they unfortunately decided that to them, it did not look like necrotizing fasciitis.
As a result, the patient remained under the supervision of the medics. However, overnight, things took a turn for the worse: the patient systemically crashed. She was admitted to the intensive treatment unit (ITU), intubated, and ventilated. She was also put on maximum inotropes in order to support her heart.
The following morning, I was called in to see her. I quickly recognized that something was going on in her calf: it was swollen, and there was a little patch of redness. It did not look too dramatic, but I knew we were in trouble—all her organs were failing, and plainly, the patient was dying.
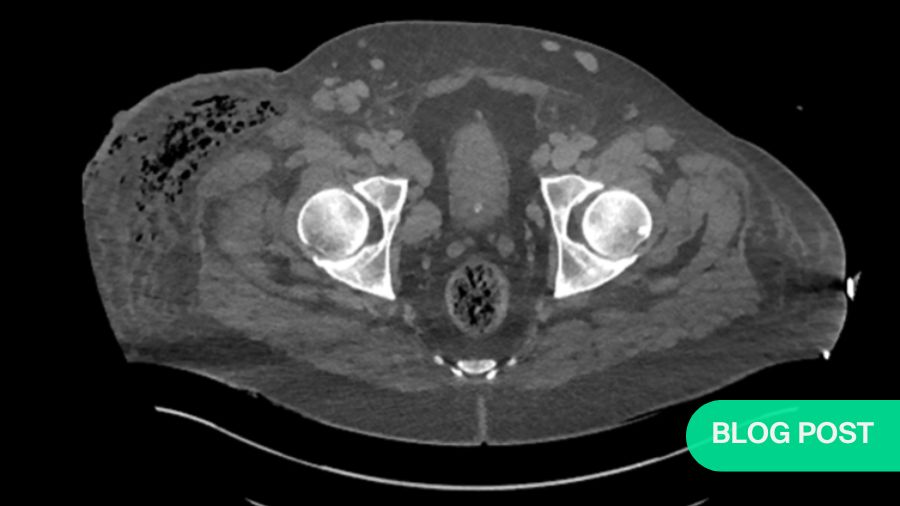
It was way too late at this point to obtain imaging. We knew that if we were going to save this woman’s life, we would have to act quickly, and that we would have to start with the place where her problems had started. I was fairly confident that I could alleviate things surgically. Of course, I did not know exactly what was going on. But I knew that the cause of her systemic failure was in her leg. So, we decided to open up the calf and check for necrotic tissue as well as puss needing to be released.
We were able to get the patient into an emergency operating theater around three or four hours later. By that time—and this is a very stark illustration of how rapidly necrotizing fasciitis can develop—her leg had deteriorated considerably. Only a few hours before, there had been a small patch of redness on the calf, entirely below the knee. The difference between then and what I was looking at now gave me a profound scare.
Further escalation
So, I went ahead and did a systematic debridement, cutting away skin, fascia, and muscle tissue layer by layer. I started in the worst-looking area and began radiating outwards. The muscles I cut out did not look too traumatic, but they were dead. The brown discoloring is a clear sign of that. Unfortunately, we eventually realized that there was too much muscle for me to be able to excise it all compartment by compartment and save her limb. We therefore decided to perform a transfemoral amputation—we amputated the leg above the knee.
We chose to do a guillotine amputation without closing the skin, because the skin and fascial debridement was bigger than the muscle. Our thinking was that we wanted to retain whatever tissue was still healthy and alive in order to keep as many reconstructive options as possible for later by saving as much of the residual limb as we could for prosthesis fitting.
With the amputation complete, the patient was sent back to the ITU. Her me dication was adjusted to include clindamycin, an antibiotic used to treat serious infections, as well as immunoglobulin. At this point, I was sure that I had gotten rid of all the infected tissue. I went home thinking this was a job well done and that I had saved this woman’s life. However, at six a.m. the following morning, the intensivist called me. The patient had deteriorated further and he asked me to come in immediately.
Turns out, I had not gotten ahead of the infection after all. Not even 24 hours after the amputation which I thought had cured her, every muscle in her thigh was necrotic. The infection was rampant, and moving proximally. The fascia was probably the worst affected tissue. Eventually, we had no choice but to progress onto a hip disarticulation amputation. Mind you, there was never any bone involved at all. The infection strictly affected the soft tissue.
A happy ending despite all odds
As unlikely as it may seem, the story ends happily. We got on top of the infection with the last set of debridements. Reconstructive surgery was a challenge because the patient literally had a naked pelvis, complicated further by issues such as a diverting colostomy. But we eventually managed a reconstruction with free tissue transfers. Today, the patient is back in her life as a mum and a teacher. In fact, she does not even use a wheelchair or any kind of prosthetic. Instead, she relies on crutches.
The reason I look back on this as my most challenging case to date is how rampant this infection was in a previously healthy patient, and how we constantly were slightly behind. I now realize that with cases like this one, there is a critical point early on that we cannot afford to miss. Conversely, if we recognize early on what we are looking at, then extreme outcomes like this one can be averted, and in many cases probably with just antibiotic therapy.
As I said before, soft tissue infections are not uncommon. In fact, there are numerous cases that are not ever referred to a surgeon because the medics get on top of it in time. But that is exactly why it is so important for orthopedic surgeons like myself to work on how we can better recognize the ones they do not.
This example of course is a very extreme one. I am not advocating for colleagues to immediately consider surgery in every soft tissue infection consult they get. But we do need to be aware that some of these cases can progress much too fast for imaging. We pick it up too late, and once we get behind, we have no choice but to be bold in order to stop this terrible process.
Telltale signs of group A streptococcus bacteria to look out for
So, my hope is that we can collectively change our approach. It may sound bizarre, but we should stop thinking of necrotizing fasciitis as necrotizing fasciitis. Because it does not necessarily present in the one typical way that we are taught. The reality is that these life-threatening soft tissue infections have a huge spectrum of how they present, including the physical appearance of the skin, the kind of patient it happens to and even the rate of progression.
There are a few red flags for group A streptococcus bacteria, which is what I specifically talking about here, and which is slightly different from multi-bacterial infections. But being able to recognize it will help you with the full spectrum of soft tissue infections.
The first telltale sign is intense pain. Sometimes we tend to focus a little too much on visual appearances, but remember: this is generally a very painful condition. These are invasive infections that produce toxins which kill tissue, and they cause ischemic type pain that is intense, deep, and burning. If a patient reports having been in contact recently with some kind of group A strep type infection, then you should become even more alert.
Some patients will also tell you that they are feeling very sick or they will show the corresponding behavior—sometimes they already have delirium by the time they get to the emergency room. So, while cellulitis is a little uncomfortable and causes a kind of prickly pain that’s not unlike a sunburn, it is not overtly painful. Likewise, you may pick up some abnormalities in blood tests, but patients do not present with organ dysfunction.
Lastly, the illness does not behave as it should and patients do not respond to antibiotics. Most people who present with cellulitis will have improved within 24 hours of receiving antibiotics.
Three takeaways that could save lives
This case has profoundly changed my approach to how I teach residents and how I talk about this issue. Firstly, we as orthopedic surgeons must accept our role and be involved. Granted, it can make us feel uncomfortable, because it is outside of our expertise. But a vascular surgeon or a general surgeon will not be able to do it much better than us. Almost always, we will have a great acute team ready to look after serious limb problems. We just have to apply it a little bit.
If you feel you are out of your depth, call a friend. It can be a huge help when there are two of you spurring each other on. If there is a plastic surgeon who can get involved, great. But many of us work in hospitals that do not have a plastic surgeon or at least not one that is available all the time. We should not shy away from this—this is a chance for us to save lives.
Secondly, do not try and recognize necrotizing fasciitis. It sounds weird, but it can present very differently. If a case looks different from a previous case of necrotizing fasciitis, still do not rule it out. If you do, you will miss opportunities to help people. Instead, I would like you to ask the question, is this a life-threatening soft tissue infection? And how do you recognize if something is indeed life-threatening? All the things I outlined: it is going more rapidly, it is not responding to treatment, is the patient developing organ dysfunction?
Thirdly, once you have recognized that something could be a life-threatening soft tissue infection, the only other thing you have to ask yourself is, can I help surgically? Is there a target? Do I know where to start cutting? And could my cutting potentially help? And the answer is almost always yes. There will times when it is difficult to work out, and maybe imaging can help you plan or target where you are going. But sometimes you have to be ready to operate on clinical grounds only, even if it may feel unusual to simply start a systematic exploration with the nastiest-looking point and move on from there.
I am convinced that if you do those three things well—accept responsibility, however reluctant you may be, try to recognize whether something is a serious infection, and decide whether you can help surgically—then you will probably prevent some terrible illnesses, and maybe even save the lives of a few patients. Because without you changing your attitude like this, they will likely not have access to that kind of care.
Video: Iain McFadyen talks to Samir Mehta about a career affirming moment, an extraordinarily challenging necrotizing fasciitis case and difficult surgery
About the author:
Dr Iain McFadyen is an experienced consultant in Trauma and Orthopaedics with a full-time trauma practice. He has a special interest in complex upper and lower limb fractures, non-union, bone infection and deformity correction. McFadyen was previously Chief of Trauma in Brighton where he helped lead the establishment of major trauma systems. He is the National Director of Clinical Audit for the UK's Trauma Audit and Research Network (TARN) and co-chairman of the Fracture Guidelines Development Group for the National Institute for Health and Care Excellence (NICE).
You might also be interested in:
AO Surgery Reference
AO Surgery Reference is your go-to resource for the management of fractures, based on current clinical principles, practices, and available evidence.
myAO
Join AO's digital network! On myAO, you can securely save and share cases, connect and exchange knowledge with peers, and access leading clinical and scientific expertise.
AO video hub
Discover a wealth of educational videos, practical exercises, recorded webinars, expert presentations, and interviews from AO's world-renowned faculty.