Beyond union: predicting post-traumatic osteoarthritis after intra-articular injury
BY PROF M. A. IMAM

Most trauma surgeons have met the patient who reminds us that “union” is not the finish line. The fracture heals, the X-ray looks tidy, but the joint never truly forgives. They are the patient who returns months later with persistent swelling, morning stiffness, aching with stairs, or a gradual loss of motion, and asks, “Did something go wrong?”
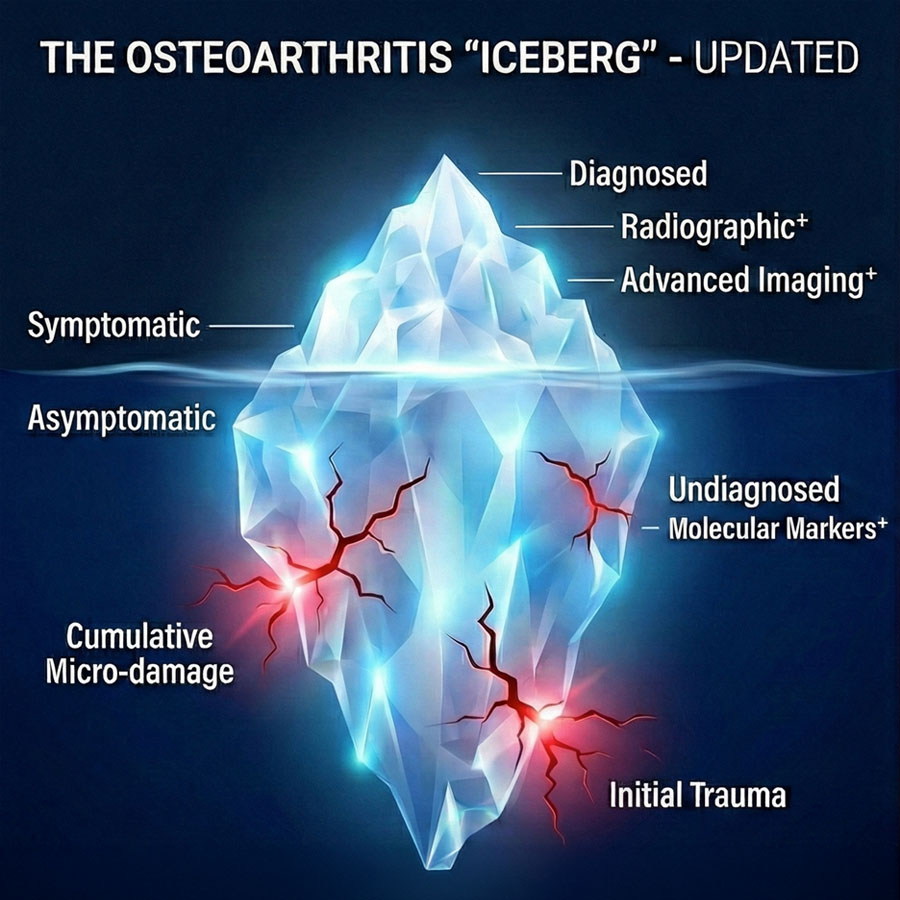
Often, nothing went wrong in the operating theatre, yet joint biology and joint mechanics were injured enough for degeneration to have already begun. That is a core challenge of post-traumatic osteoarthritis (PTOA). It is not simply “wear and tear”, but a whole-joint response to injury that develops over years, sometimes even when our reduction was excellent.
-
Read the quick summary:
- An orthopedic trauma perspective on predicting post-traumatic osteoarthritis (PTOA) after intra-articular injury, emphasizes biology, mechanics, and early risk stratification.
- PTOA risk persists despite perfect fixation. Early signals include injury phenotype, mechanical factors at union, and the patient’s early recovery trajectory.
- Surgeons can stratify high-risk patients early and implement targeted rehab, structured follow-up, imaging triggers, and registry-based monitoring to protect long-term joint health.
- Registries are a long game. Feed PROMs + imaging + reoperations back into the audit cycles to improve prediction, generalizability, and AO-alignment.
- Biomarkers/genomics should be treated as future layers for research-embedded pathways. Current best predictors remain injury severity, mechanics, and recovery trajectory.
Disclaimer: The article represents the opinion of individual authors exclusively and not necessarily the opinion of AO or its clinical specialties.
Recent trauma-related knee data continues to emphasize how common this can be following intra-articular injury. For tibial plateau fractures, medium- and long-term cohorts report high radiographic OA prevalence and variable functional outcomes, with identifiable risk factors. Additionally, long-term studies indicate that a significant minority progress to joint replacement within a decade, with specific radiographic features at union predicting risk [1].
If AO principles aim for durable function, then the next step is obvious: treat intra-articular trauma as a long-term joint-health problem—not only a short-term fixation problem [2].
Biology and mechanics: the two drivers of PTOA
The biological “first hit”: cartilage + synovium + subchondral bone
At the moment of injury, cartilage can be damaged in ways that no implant can reverse. Chondrocyte death, matrix disruption, and a synovial inflammatory response can persist and amplify degeneration. Contemporary reviews of knee PTOA emphasize that this is not a single-tissue problem; it is a coupled process involving cartilage, synovium, and bone, influenced by inflammatory pathways [3].
A classic clinical example is the ankle: in a large prospective cohort of operatively treated ankle fractures, arthroscopically identified initial cartilage lesions were an independent predictor of later PTOA and worse clinical outcome [4]. The study makes a simple point trauma teams recognize immediately: the joint can be “injured for life” on day one, even when fixation is technically sound.
The mechanical “second hit”: incongruity, malalignment, and micro-instability
Even small residual abnormalities, step-offs, depression, widening, malalignment, and subtle instability can alter contact stresses and joint loading. Long-term tibial plateau data underline this: joint depression and increased tibial width at union have been associated with later progression to total knee arthroplasty (TKA). Similarly, contemporary reviews focusing on tibial plateau fixation describe multiple mechanical and injury-severity factors associated with PTOA risk [5]. The pragmatic take-home message is that biology can “load the gun”, mechanics can “pull the trigger”, and most poor outcomes reflect some combination of both.
A practical approach to establish who is high-risk in clinic
The goal here is not to predict PTOA with a false precision like “you have a 37% risk”, but to identify the patient who deserves a different pathway with tighter follow-ups, earlier rehab escalation, earlier imaging when indicated, and earlier counselling about joint-health risk [6].
1) Injury phenotype and joint-surface insult
Start with what you already know: energy, complexity, and soft-tissue insult are powerful signals.
In tibial plateau fixation, reviews, and cohort work consistently highlight risk factors such as fracture complexity and severity, extensive soft-tissue damage, open injury/compartment syndrome, and reduction-related factors.
Long-term outcome studies show that measurable features at union (depression/widening) correlate with later need for arthroplasty [7].
When the injury is high-energy, comminuted, or has large articular involvement, or when you need a complex reconstruction, treat that patient as “high-risk until proven otherwise.”
2) Early function trajectory: the “recovery slope”
Trauma follow-up often samples recovery as snapshots. PTOA risk often reveals itself as a trajectory. In practice, the recovery slope can be captured with a handful of consistent data points over 6–12 weeks:
- pain + effusion pattern
- ROM slope. Is it climbing week by week?
- tolerance of weight bearing as appropriate
- return of basic function milestones
- a short joint-specific PROM. When used consistently, even a brief one beats a perfect one used inconsistently
Large cohorts in tibial plateau outcomes demonstrate that medium- and long-term function varies substantially, supporting the value of earlier identification of patients who are drifting off course [8].
If ROM is plateauing early, swelling is persistent, and function is not advancing on schedule, don’t normalize it as “expected trauma recovery.” That is often your earliest warning.
3) Imaging strategy and red flags: targeted imaging for decision-making
Imaging helps when it answers one of two questions:
- Is there a remediable mechanical driver, such as loss of reduction, malalignment, instability, hardware issue, depression/widening?
- Is there evidence of significant joint injury burden where imaging will alter counselling, rehab intensity, or consideration of adjunct strategies?
From long-term tibial plateau work, union-time features like depression and widening have prognostic relevance. From ankle fracture data, initial cartilage injury is a prognostic factor for later PTOA [4].
Practical red flags that justify earlier review or escalation, tailored to joint:
- persistent effusion and pain disproportionate to the expected phase
- ROM plateau, especially extension loss in the knee or dorsiflexion loss in the ankle
- recurrent mechanical symptoms, catching/locking/instability
- progressive malalignment or loss of reduction on serial films
- inability to progress milestones without a clear reason (pain control, fear-avoidance, access barriers)
A practical follow-up model to protect function
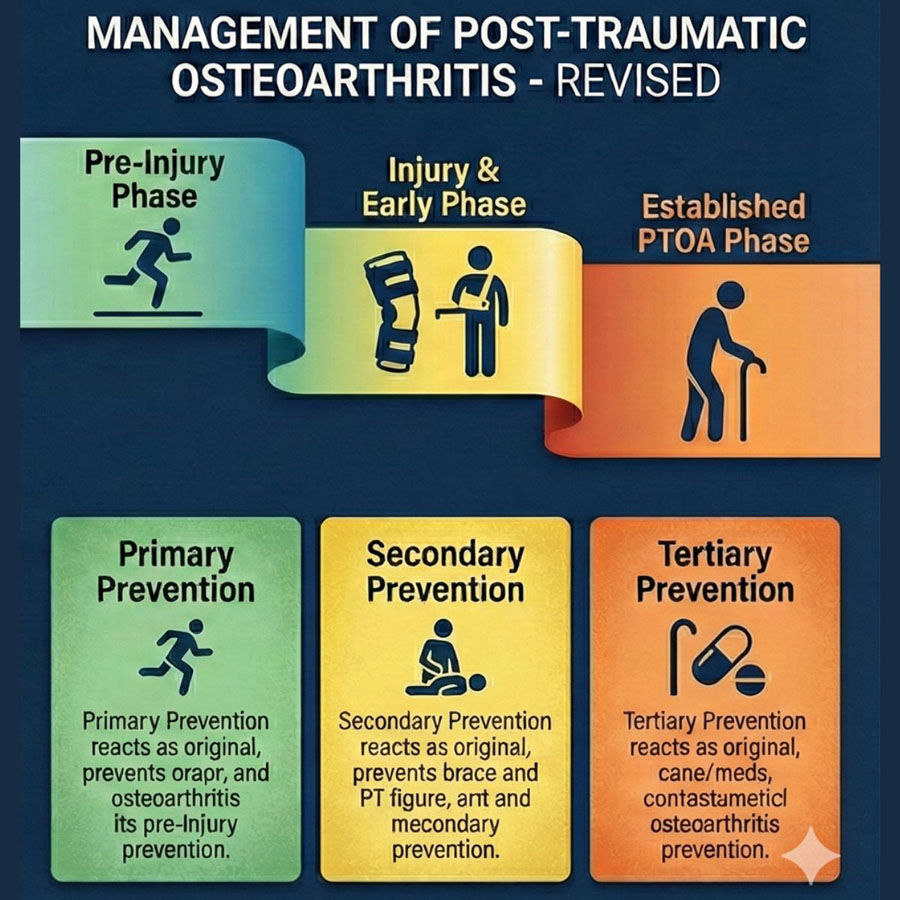
1) Targeted rehab and early stiffness pathways
There are things we can do differently. High-risk patients should not receive generic advice; they should receive a defined pathway with:
- early therapy review with explicit ROM targets
- a time-based escalation plan (“reassess if ROM hasn’t improved by X by week Y”)
- pain control optimization to permit movement
- early identification of barriers (fear-avoidance, transport, social constraints, rehab access)
In many joints, stiffness and persistent synovitis-type symptoms become self-reinforcing, so early action is often lower risk than late salvage [9].
2) Counselling that is honest but not fatalistic
When patients hear the word “arthritis” they often think it means inevitable decline. Our job is to explain PTOA risk in a way that is truthful and actionable:
- explain that intra-articular trauma is both a biological and mechanical event
- set realistic expectations. The joint may be vulnerable even after excellent surgery
- emphasize controllable levers: ROM work, gradual strength, weight management where relevant, adherence, and follow-up
- define what “off track” looks like and what you will do if it happens
This is one of the most powerful interventions we have because adherence and early symptom reporting often change outcomes [10].
3) Monitoring that is simple enough to sustain
The best monitoring bundle is the one your team will do every time. A minimalist approach for intra-articular injuries includes:
- a short PROM at baseline and follow-up (consistent tool, consistent time points)
- standardized ROM measurement
- a brief pain/effusion check
- imaging only when it will change management
Recent tibial plateau cohorts show how much outcomes vary and how important long-term follow-up is. A consistent monitoring bundle helps to intervene earlier and to learn from your own outcomes [11].
Registry feedback loop: how prediction improves over time (AO-aligned)
The most scalable way to improve PTOA prediction is not to build the perfect model once. It is to build a system that teaches safely over time.
A practical registry loop:
- capture baseline phenotype (injury pattern, soft tissue, treatment details)
- capture early trajectory (2–6–12 weeks)
- capture mid-term outcomes (6–12 months)
- capture late outcomes where feasible (2–5 years), including OA signals and reoperations
- feed back into pathway design who gets intensified follow-up, which red flags trigger escalation, what surgical/rehab factors predict problems
Recent cohort studies on tibial plateau fractures explicitly link radiographic OA prevalence, functional outcomes, and risk factors, reinforcing the value of structured long-term follow-up.
The registry mindset also keeps us more honest: if a unit’s outcomes improve year on year, it’s rarely because of a single technology, but because measurement and feedback together reduce variation and improve decisions [12].
Future layers with biomarkers and genomics
Biomarkers and genomics are attractive because they speak to the biological “first hit”, but the current clinically responsible position to take is “promising, not yet routine”.
A 2025 review focused on synovial biomarkers and PTOA risk highlights active research interest but also the reality that most candidates require better validation and clearer clinical utility before they can guide everyday post-injury care. Broader 2025 work on the clinical and molecular landscape of PTOA similarly emphasizes biomarkers as tools for early diagnosis and monitoring, while acknowledging translation challenges [13].
Biomarkers may become useful for identifying high biological responders after injury. But today, they best belong in research-embedded pathways, trials, and specialized settings. Our most useful predictors remain injury phenotype, mechanics at union, and recovery slope.
My Monday-morning checklist: a 5-step plan for the trauma unit
- Define your high-risk intra-articular list (tibial plateau, pilon, acetabulum, complex ankle, etc.)
- Standardize early trajectory capture (ROM + brief PROM + pain/effusion pattern at 2–6–12 weeks)
- Agree on imaging red flags that trigger escalation (not routine scans)
- Implement a stiffness pathway with explicit targets and time-based escalation
- Start or join an existing registry loop so your pathway improves year on year
About the author:
Professor M. A. Imam: Consultant Upper Limb & Complex Trauma Surgeon. Clinical Lead at Rowley Bristow. Professor & Medical Director at University of East London. Fellowship-trained in Oxford, Stanford, Zurich, Mayo Clinic & Steadman. Founder of OrthoGlobe. Author of UNLOCK.
Prof Imam is also an AO Faculty member with the AO Foundation and teaches in multiple courses globally.
Further reading:
- TRIPOD+AI Statement (EQUATOR Network). Reporting guidance for prediction models using regression/ML
- WHO. Ethics and governance of artificial intelligence for health. 2021.
- NICE. Evidence standards framework for digital health technologies (ESF).
References:
- Klasér J, Kotake L, Lindberg M, Wigge S, Lundqvist R, Szczęsny G, et al. Prevalence of osteoarthritis and clinical outcomes in patients with fractures of the tibial plateau - medium- and long-term analysis. BMC Musculoskelet Disord. 2025;26:522. https://doi.org/10.1186/s12891-025-08786-7
- Howell M, Khalid A, Nelson C, Doonan J, Jones B, Blyth M. Long term outcomes following tibial plateau fracture fixation and risk factors for progression to total knee arthroplasty. The Knee. 2024;51:303–11. https://doi.org/10.1016/j.knee.2024.10.003/li>
- O’Sullivan O, Valdes AM, Watson F, Kluzek S, Bull AMJ, Bennett AN. Insights into knee post-traumatic osteoarthritis pathophysiology from the relationship of serum biomarkers to radiographic features in the ADVANCE cohort. Arthritis Res Ther. 2025;27:207. https://doi.org/10.1186/s13075-025-03648-y
- Stufkens SA, Knupp M, Horisberger M, Lampert C, Hintermann B. Cartilage lesions and the development of osteoarthritis after internal fixation of ankle fractures: a prospective study. J Bone Joint Surg Am. 2010;92:279–86. https://doi.org/10.2106/JBJS.H.01635
- Franulic N, Muñoz JT, Pineda T, Laso J, Olivieri R, Schröter S. Fixation of tibial plateau fracture – risk factors for developing infection: a narrative review. 2024 [cited 2026 Jan 17]; https://doi.org/10.1530/EOR-24-0058
- Whittaker JL, Culvenor AG, Juhl CB, Berg B, Bricca A, Filbay SR, et al. OPTIKNEE 2022: consensus recommendations to optimise knee health after traumatic knee injury to prevent osteoarthritis. Br J Sports Med. 2022;56:1393–405. https://doi.org/10.1136/bjsports-2022-106299
- Assink N, El Moumni M, Kraeima J, Bosma E, Nijveldt RJ, van Helden SH, et al. Radiographic Predictors of Conversion to Total Knee Arthroplasty After Tibial Plateau Fracture Surgery: Results in a Large Multicenter Cohort. J Bone Joint Surg Am. 2023;105:1237–45. https://doi.org/10.2106/JBJS.22.00500
- OLERUD F, GARLAND A, HAILER NP, WOLF O. Risk of conversion to total knee arthroplasty after surgically treated tibial plateau fractures: an observational cohort study of 439 patients. Acta Orthop. 2024;95:206–11. https://doi.org/10.2340/17453674.2024.40605
- Lee DR, Therrien E, Song BM, Camp CL, Krych AJ, Stuart MJ, et al. Arthrofibrosis Nightmares – Prevention & Management Strategies. Sports Med Arthrosc Rev. 2022;30:29–41. https://doi.org/10.1097/JSA.0000000000000324
- Kolasinski SL, Neogi T, Hochberg MC, Oatis C, Guyatt G, Block J, et al. 2019 American College of Rheumatology/Arthritis Foundation Guideline for the Management of Osteoarthritis of the Hand, Hip, and Knee. Arthritis Care Res (Hoboken). 2020;72:149–62. https://doi.org/10.1002/acr.24131
- Lang C, Hörmandinger C, Klaut M, Neidlein C, Watrinet J, Arnholdt J, et al. Clinical outcome in tibial plateau fractures improves over time: Insights from a collaborative data network. Injury. 2025;56:112607. https://doi.org/10.1016/j.injury.2025.112607
- Wilson I, Bohm E, Lübbeke A, Lyman S, Overgaard S, Rolfson O, et al. Orthopaedic registries with patient-reported outcome measures. EFORT Open Rev. 2019;4:357–67. https://doi.org/10.1302/2058-5241.4.180080
- Takase K, McCulloch PC, Yik JHN, Haudenschild DR. Clinical and molecular landscape of post-traumatic osteoarthritis. Connective Tissue Research. Taylor & Francis; 2025;66:373–9. https://doi.org/10.1080/03008207.2025.2490797
Disclosures: No conflicts of interest or funding. Claude Opus 4.5 thinking process was utilized to support drafting and editing. All content was reviewed, fact-checked, and finalized by the author.
You might also be interested in...
AO Trauma curriculum courses
Learn more and find your next AO Trauma’s competency-based curriculum course.
AO Surgery Reference (AO SR)
AO’s popular resource for the management of fractures, based on principles, practices, and evidence.
myAO 2.0
The global AO-managed community built on belonging, shared purpose, trust, and self-organization is just one click away.
Faculty programs and resources
The passion and dedication of AO Trauma faculty drive the outstanding reputation of AO Trauma’s educational offerings.