For calcaneal fractures, approach and fixation decisions rely on soft tissue healing potential
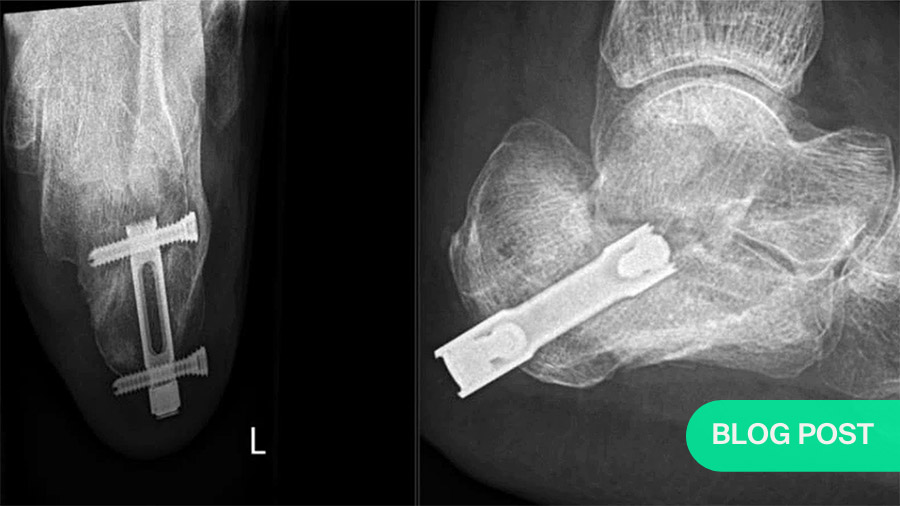
Calcaneal fractures can be very problematic to heal, with serious consequences to patients’ quality of life. However, when choosing an approach and fixation, success is not simply a matter of achieving a well-aligned reduction. Joris Hermus (Maastricht University Medical Center, the Netherlands) and Aleksas Makulavicius (Vilnius University Hospital, Lithuania) recently met to discuss the problem of how to choose approaches and fixation techniques that match patient characteristics. Here, they also speak of visualization options.
Makulavicius opened by emphasizing that, for calcaneal fractures, the surrounding tissue is a matter of major concern: “These fractures occur in a very sensitive area surrounded by soft tissue, which is very unforgiving. Normally, the fracture site is a soft tissue injury with a broken bone inside.”
As calcaneal fractures often tend to have high-energy causes—traffic accidents or falls from ladders, for example—they not only present serious challenges on their own, but also tend to accompany other traumatic injuries. Therefore, the trauma surgeon’s initial job may be simply to correct the most serious displacement and close open wounds, then wait to perform the definitive surgery. In addition to minimizing infection risk, this relieves the pressure on the surrounding soft tissue, where necrosis can quickly set in.
Complications and treatment
Complications such as infection, soft tissue necrosis, or even simply overtaxing the patient’s ability to heal can greatly increase recovery time. Therefore, both surgical approaches and fixation techniques must be weighed against the complication risks they entail.
“Treatment choice depends on soft tissue healing potential. For an otherwise healthy patient with reasonably robust soft tissue, we can be more aggressive. Conversely, if there are soft tissue problems, or the patient’s general status or cooperativity level is poor, our approach will have to be more conservative. For example, we need to think about smaller incisions, percutaneous techniques, and less invasive fixation. Non-operative treatment is normally reserved for non-displaced fractures or non-compliant, elderly, or high-risk patients with multiple contraindications regarding surgery. After calcaneus surgical treatment, infection can be disastrous.”
Makulavicius also summarized the main radiographic tools used for diagnosis and planning. For an intraarticular fracture, an initial x-ray will usually be enough to choose an Essex-Lopresti classification—that is, whether it is a joint-depression or tongue-type.
To plan treatment, though, more information is necessary. For that, either 2-D or 3-D CT scans will allow better understanding and the use of a Sanders classification. The number of fracture lines on the posterior articular surface plus one will determine the Sanders number: Calcaneus fracture without displacement is type 1; one or two lines indicate, respectively, types two or three; and three or more lines are classed as type 4.
“The key for treatment success is to select the right patient, the right timing and the correct approach, achieve anatomical reduction, ensure adequate fixation—absolute for the articular part, relative of the rest—and, most importantly, to avoid severe complications by using less invasive, less traumatic approaches with high-risk patients.”
Open vs percutaneous approaches, implants, and first steps
Where a surgical approach is indicated, the surgeon must decide between an open or percutaneous option. “For open approaches, lateral extensile surgery was routine a few decades ago. While that remains relevant, the sinus tarsi approach is now becoming more popular. For pure sustentaculum fractures, a direct medial approach is now routine. For simple and highly displaced tongue-type fractures, a posterior approach is recommended.”
Even with a percutaneous approach’s smaller incisions, a good range of implants is available. “For fixation, implants include lag screws, anatomical plates, and special nails; sometimes screws and K-wires are combined.” After each step of the reduction, fragments are positioned and fixed temporarily until image intensification allows the surgeon to confirm the positioning. “We confirm the reduction under image intensification. If we are satisfied, we fix the joint fragment, usually with lag screws, and neutralize the rest with a calcaneal locking plate or intramedullary screws or an intramedullary nail.”
Whichever surgical approach is used, external fixation techniques such as Schantz pins provide effective manipulation with minimal soft tissue damage.
Sinus tarsi vs extensile lateral approach
While Makulavicius noted that the classic extensile L-type approach was appropriate in patients with robust soft tissue or many bone fragments, he emphasized the additional soft tissue damage it entails. “This makes the outcome rather unpredictable, particularly in high-risk patients.”
“For safer management, less traumatic techniques such as the sinus tarsi approach are preferable. While the lower visibility can lead to less accurate reduction, C-arm image intensification or intraoperative CT can be used to confirm both the reduction and the placement of any implants.”
“Compared to an L-type approach, short-term outcomes following the sinus tarsi approach are excellent: less pain, faster soft tissue healing and shorter hospital stays. A post-operative stay of one or two days is typically sufficient before the patient can be discharged.”
To wrap up the discussion, Hermus emphasized the importance in every case of considering the injury, the patient, and one’s own skill as a surgeon to decide whether surgery was advisable.
“First, we need to decide whether we need to perform surgery, which fractures can best be treated conservatively, and which patients have the highest risk of complications. And always ask yourself, am I capable of this kind of surgery? For example, tongue-type or open fractures demand immediate reduction. Otherwise, try to wait until you see the wrinkle sign, then scan and plan your surgery.”
“So, choose the right approach for your patient and fracture type. For less complex intraarticular fractures, the sinus tarsi approach is the best. More complex cases will probably require an extended lateral approach. However, if there are comorbidities such as diabetes or smoking, the sinus tarsi approach would be more acceptable, even with less visibility.”
“To optimize your visibility, apart from choosing a larger approach, we can use additional instruments such as arthroscopy or the 3D intensifier.” While Hermus considered the 3D intensifier a valuable tool, he did not advocate using it exclusively. Instead, he employed it as a security measure to help spot potential complicators. “Once you are satisfied with the results, confirm that with a run of the 3D intensifier. If that shows malreduction or malpositioning of the screws, you can correct these and finish with a final 3D run.”
About the video
This discussion and presentation are part of the AO Trauma Webinar Series. The same webinar includes a description of how to conduct a subtalar fusion. The full video, including all presentation slides, is available to AO Trauma members at no cost.
AO Trauma thanks Hermus and Makulavicius for sharing their time, knowledge, and experience with their colleagues around the world.
About the authors
Joris Hermus
Maastricht University, Netherlands
Aleksas Makulavicius
Education:
1994 graduated from Medical Faculty of Vilnius University
2021 completed PhD. Topic “ Results of open v. percutaneous repair of AATR”
Work experience:
Vilnius University Center of Orthopedics and Traumatology. Team leader in F@A Northway Medical Center
Research and publications:
- Makulavičius A, Mazarevičius G, Klinga M, Urmanavičius M, et al. "Outcomes of open "crown" type v. percutaneous Bunnell type repair of acute Achilles tendon ruptures. Randomized control study. Foot Ankle" Surg. 2020 Jul;26(5):580-584. doi: 10.1016/j.fas.2019.07.011. Epub 2019 Aug 3. PMID: 31548150.
- Makulavicius A, Martin Oliva X, Mazarevicius G, et al. "Comparative anatomical study of standard percutaneous and modified medialised percutaneous Bunnell type repair for artificial Achilles tendon rupture: positive effect of medialisation of the stitches with lower risk of sural nerve injury". Folia Morphol (Warsz). 2016;75(1):53-59. doi: 10.5603/FM.a2015.0067. Epub 2015 Sep 14. PMID: 26365861.
Disclaimer
The articles included in the AO Trauma Blog represent the opinion of individual authors exclusively and not necessarily the opinion of AO Trauma or AO Foundation.


