Unstable but neurologically intact: are we over-operating in spinal trauma?
BY DRS LUIZ GUSTAVO DAL OGLIO DA ROCHA, MANUEL JOSE VALENCIA CARRASCO, AND RATKO YURAC

Management of neurologically intact spinal trauma in patients remains one of the most debated areas in spine surgery. These patients often present after high-energy trauma with significant vertebral body damage and concerning imaging findings, yet they maintain full neurological function. For us, the practicing spine surgeons, the decision between operative and nonoperative management is rarely straightforward.
-
Read the quick summary:
- Spine surgeons from Latin America discuss whether neurologically intact spinal trauma patients are being overtreated surgically.
- Many fractures heal well nonoperatively; instability is multifactorial and imaging alone can overestimate need for surgery.
- Surgeons should apply structured assessment with neurology, PLC, alignment, and patient factors and balance evidence with judgment before operating.
- There is ongoing debate on defining instability and a need for stronger evidence to guide when surgery improves outcomes.
Disclaimer: The article represents the opinion of individual authors exclusively and not necessarily the opinion of AO or its clinical specialties.
Over the past two decades, surgical capabilities have advanced dramatically. Modern pedicle screw systems, minimally invasive approaches, and improved imaging allow surgeons to stabilize fractures quickly and reliably. As a result, operative treatment has become increasingly common in many centers.
But clinical reality is more complex. Many neurologically intact patients recover well with nonoperative treatment. This raises a critical and highly debated question for surgeons: Are we increasingly operating on injuries that might be treated successfully with nonoperative strategies?
The AO Latin America Regional course AO Spine Masters Course—Fixing the unfixable: Expert challenges in spinal trauma provides an opportunity to critically examine modern treatment strategies including minimally invasive techniques, deformity assessment, and complication management, helping surgeons refine decision-making and select the most appropriate approach for complex spine trauma cases.
Understanding what “unstable” really means
One of the first challenges in these cases is defining instability. Radiographic findings alone can be misleading. A burst fracture with significant vertebral body comminution may appear alarming on CT, yet the patient may have intact posterior ligamentous structures and preserved neurological function.
In practice, instability is not caused by a single variable but results from multiple elements, including fracture morphology, the integrity of the posterior ligamentous complex, the extent of vertebral body collapse, and sagittal alignment. Neurological status also plays a key role in urgency and guiding treatment decisions.
The clinician assessing a new trauma patient needs to consider these elements. Classification systems like the AO Spine Thoracolumbar Injury Classification or TLICS can help organize and guide this evaluation, but they should not replace clinical judgment
Why surgeons often choose to operate
In daily practice, several practical considerations can push treatment decisions toward surgery.
First, instability remains a leading cause of failure after thoracolumbar fracture treatment. Surgeons who have experienced difficult reoperations for late instability may develop a lower threshold for early fixation.
Second, surgical stabilization provides immediate mechanical control of the injured segment. For polytrauma patients, early mobilization can simplify overall care and decrease complications associated with prolonged immobilization (damage control surgery).
Third, surgical correction can restore alignment and reduce kyphotic deformity. From a technical perspective, this can feel like achieving a definitive solution.
Finally, expectations from patients or institutions can influence decision-making. Patients might see surgery as a more definitive treatment, and surgeons may feel pressured to act when imaging looks severe.
These considerations are understandable, but they should be balanced against the evidence that many neurologically intact fractures remain stable during healing and may not require surgical fixation.
What conservative management looks like today
Nonoperative treatment for thoracolumbar fractures has evolved considerably, and depending on surgeon preferences or regional traditions, it may be the preferred treatment option. In the past, conservative care often involved prolonged bed rest and rigid bracing. Modern protocols, however, emphasize early mobilization, pain management, and structured rehabilitation.
For the neurologically intact patient with preserved ligamentous structures, this approach can produce excellent outcomes. Many patients regain function and return to normal activities without surgical intervention.
Bracing remains a debated aspect of conservative care. Some surgeons continue to prescribe thoracolumbosacral orthoses to promote early mobilization, while others depend on guided activity and physiotherapy alone. In either case, the main principle is active recovery rather than immobilization.
Close follow-up of recovery is essential. Serial imaging helps monitor alignment and detect progressive deformity. Most patients who are appropriately selected for conservative management remain stable during healing.
Soft instability versus radiographic instability
Another clinical dilemma arises when imaging suggests significant structural injury, but the patient remains clinically stable. CT scans may show burst fractures with canal compromise or moderate kyphosis, yet neurological function is intact, and pain is manageable.
In these situations, the temptation to operate can be strong. Radiographic deformity might seem unacceptable, and the surgeon may worry about long-term outcomes.
However, clinical outcomes do not always correlate with radiographic correction. Many patients tolerate moderate kyphosis without functional impairment. Conversely, surgical correction of alignment does not guarantee improved long-term outcomes.
For practicing surgeons, the key is to distinguish between fractures that are mechanically unstable and those that appear dramatic on imaging but are not.
When surgery clearly makes sense
Despite ongoing debate, some clinical situations strongly favor surgical intervention.
Progressive neurological deficits remain the clearest indication for surgery. Similarly, confirmed disruption of the posterior ligamentous complex often indicates true mechanical instability that may not heal reliably without fixation.
Severe vertebral body collapse with loss of structural support may also require stabilization, particularly when associated with progressive deformity.
Polytrauma is another key factor to consider. In patients with multiple injuries, early spinal stabilization can help with mobilization and overall recovery.
Our challenges are in the gray area between clearly stable and clearly unstable injuries.
The cost of unnecessary surgery
Every surgical procedure has inherent risks. Infection, hardware failure, adjacent segment degeneration, and anesthesia-related complications are real concerns even in otherwise healthy trauma patients.
There is also the long-term biomechanical impact of instrumented fusion to consider. Stabilizing one segment inevitably alters load distribution across adjacent levels, potentially accelerating degenerative changes.
Beyond individual patient risks, operative treatment elevates resource use within healthcare systems. Operating room time, implants, and hospitalization all add to the economic burden of care.
When conservative treatment can achieve similar outcomes, these factors deserve careful consideration.
Considerations of decision-making in complex cases
The question of whether we are over-treating neurologically intact spinal trauma is not straightforward. Advances in surgical techniques have broadened our capacity to stabilize complex fractures safely. Simultaneously, evidence and clinical experience indicate that many injuries can heal well without surgery.
A structured decision-making approach could help reduce unnecessary variability in treatment. Here is an example of steps to consider before making the final decision:
- Assess neurological status carefully and repeatedly. Deficits can evolve during the early phase after injury.
- Evaluate the posterior ligamentous complex using imaging and clinical examination. Ligamentous disruption often represents the tipping point between conservative and operative care.
- Consider sagittal alignment and vertebral body integrity. Progressive deformity during follow-up may indicate the need for stabilization.
- Evaluate the patient holistically. Age, bone quality, associated injuries, and functional demands all impact treatment decisions.
- Involve the patient in the decision-making process. Discuss both surgical and nonoperative options openly, including the potential benefits and uncertainties of each approach.
The goal is not to avoid surgery but to apply it selectively and thoughtfully to each case. Careful assessment of fracture stability, ligament integrity, and patient-specific factors remains the cornerstone of appropriate management.
The most effective treatment strategies will likely combine evidence-based tools with experienced clinical judgment. As registries and multicenter collaborations continue to expand and produce new evidence, the field will gain clearer insights into which patients benefit most from surgical stabilization.
Until then, the neurologically intact patient with an “unstable” fracture will continue to be one of the most significant and intellectually demanding cases in spine trauma practice.
About the authors:
Dr Luiz Gustavo Dal Oglio da Rocha is a spine surgeon based in Curitiba, Brazil, where he is part of the Cajuru Hospital Spine Group, an AO Spine Fellowship Host Center. He holds a master’s degree in health sciences and has completed advanced training through AO Spine, including a long-term fellowship in 2005 at Cajuru Hospital and a fellowship at Harborview Hospital in Seattle, USA, in 2006.
He serves as a long-term AO Spine faculty member and is currently the AO Spine Latin America Chairperson Elect. He is also a member of the board of the Brazilian Spine Society.
Dr Manuel Jose Valencia Carrasco is a spine surgeon at Clínica Alemana in Santiago, Chile, and at the Mutual de Seguridad Hospital. He has over 30 years of experience in a Level 1 Trauma Center.
Dr Carrasco completed an AO/ASIF Fellowship at the Division of Trauma Surgery at the University Hospital in Zurich, Switzerland, in 1989, and an MHH-International Trauma Fellowship Program at the Trauma Department in Hanover Medical School, Germany, in 2004.
Dr Yurac is an Associate Member of the AO Spine Knowledge Forum Trauma & Infection and a member of the AO Spine Trauma Latin America Study Group. He has an h-index of 7 with co-authored 24 publications.
Past President of the Chilean Spine Committee, Orthopaedics and Traumatology Society (SCHOT), Past Chair of the AO Spine Chile council, Past Officer of Spinecenter, fellowships and Community development of the AO Spine Latam council. Actual Secretary of the Chilean Spine Society and a member of different global Spine Societies.
References and further reading:
- GSJ Special Issue Vol 14 (1S): What Motivates Treatment Decisions in Neurologically Intact Thoracolumbar Burst Fractures?
- Wood KB, Buttermann GR, Mehbod AA, Garvey TA, Jhanjee R, Sechriest VF. Operative compared with nonoperative treatment of a thoracolumbar burst fracture without neurological deficit.
- Wood KB, Buttermann GR, Phukan R, Harrod CC, Mehbod AA, Shannon B. Operative versus nonoperative treatment of thoracolumbar burst fractures without neurological deficit: long-term follow-up.
- Vaccaro AR, Lehman RA Jr, Hurlbert RJ, et al. A new classification of thoracolumbar injuries: the thoracolumbar injury classification and severity score (TLICS).
- Reinhold M, Audigé L, Schnake KJ, et al. AO spine injury classification system: a revision proposal for the thoracic and lumbar spine.
- Giele BM, Wiertsema SH, Beelen A, et al. No evidence for the effectiveness of bracing in patients with thoracolumbar fractures.
- Siebenga J, Leferink VJM, Segers MJM, et al. Treatment of traumatic thoracolumbar spine fractures: a multicenter prospective randomized study of operative versus nonsurgical treatment.
You might also be interested in...
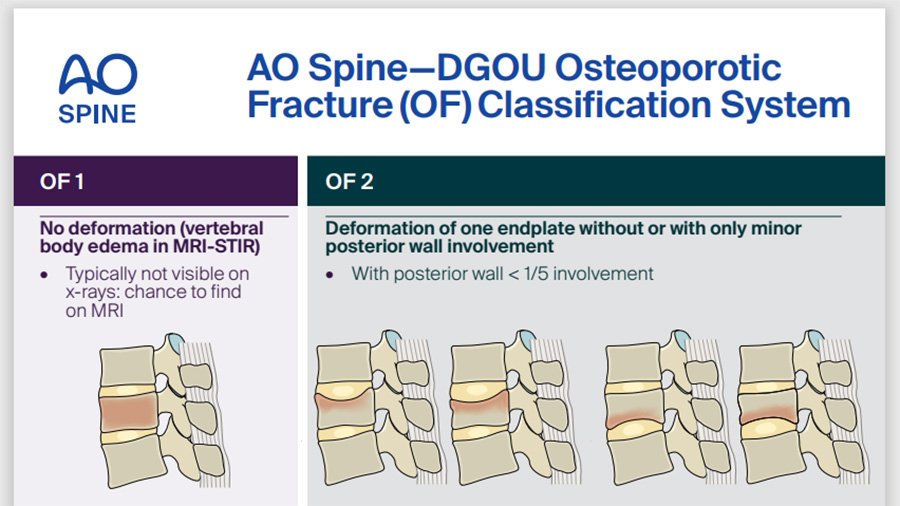
AO Spine Classification Systems
Guides and toolkits to spinal fractures, infections, deformity, osteoporosis, and tumor-related instability.
Benefit from unparalleled education
AO Regional Courses Latin America will be held in Santiago, Chile in August 2026.
AO Spine Latin America
An introduction to the activities and leading spine surgeons in the region.