VSP, 3D modeling and AR welcome the new era of personalized CMF surgery
BY DR DAVID SHAYE

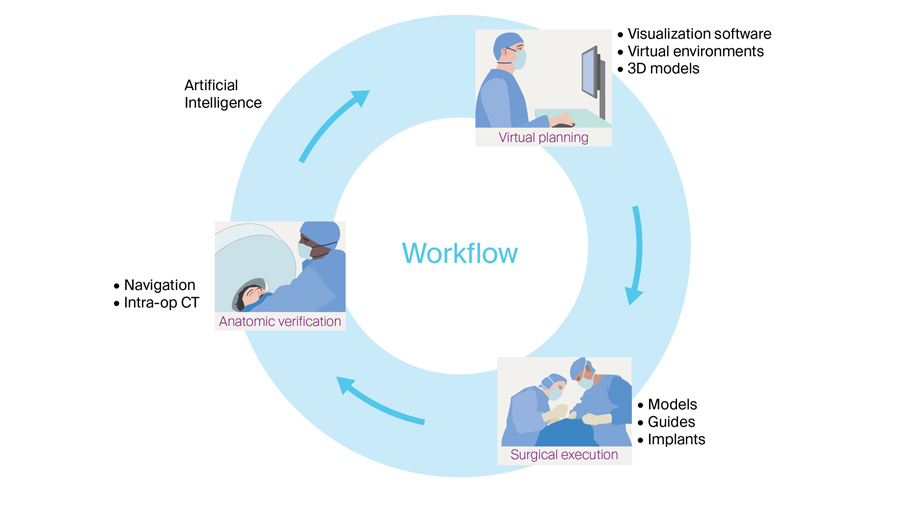
Over the last decade, digital technologies have transformed the landscape of cranio-maxillofacial (CMF) surgery. From virtual surgical planning (VSP) and intraoperative navigation to 3D modeling and augmented reality (AR), these innovations are reshaping the way surgeons' approach complex cases. What do these advances mean for patient care—and for us as surgeons?
As digital tools become more accessible and affordable, it’s crucial for CMF surgeons to receive structured training early in their careers. Exposure to these technologies demystifies their use and sparks curiosity about their many uses. Aspects of these new technologies will now be introduced in the AO’s updated Management of Facial Trauma courses. Participants will learn how technologies can improve fracture visualization, reduction, and implant placement.
-
Read the quick summary:
- Dr David Shaye discusses how digital technologies such asVSP, 3D modeling, and AR are transforming CMF surgery.
- Key outcomes include more precise planning, reduced operative times, and improved patient trust and satisfaction.
- Surgeons benefit through enhanced preoperative visualization, personalized implants, and efficient intraoperative workflows.
- Ongoing challenges include cost, accessibility, and the need for specialized training; future integration and research remain active topics.
Disclaimer: The article represents the opinion of individual authors exclusively and not necessarily the opinion of AO or its clinical specialties.
Streamlining decision-making with digital tools before and during CMF surgery
Full digital workflow is transforming surgical decision-making, both before and during the treatment procedure. The integration of digital tools into CMF workflows holds promise for reduced operative times, fewer complications, and better functional and aesthetic results.
Technologies that allow for a less invasive, more efficient procedure equate to quicker recoveries. 3D Models provide a personalized, visual understanding of each patient’s unique anatomy, allowing surgeons to re-imagine surgical planning.
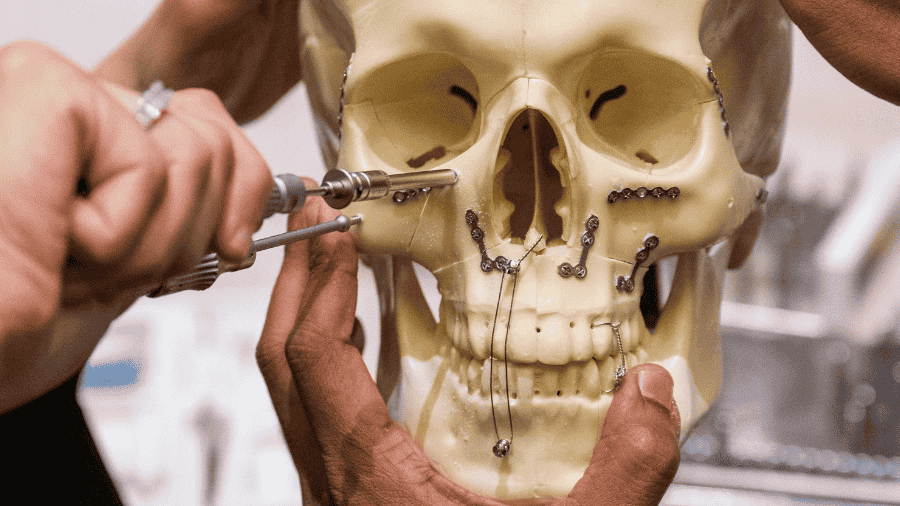
During surgery, tasks that once consumed valuable time, such as bending plates to fit complex contours, have already been offloaded to technology. With patient-specific implants (PSIs), operative workflow and surgery becomes personalized. But the benefits extend beyond the operating room.
Building patient trust through visualization with 3D CMF reconstructions
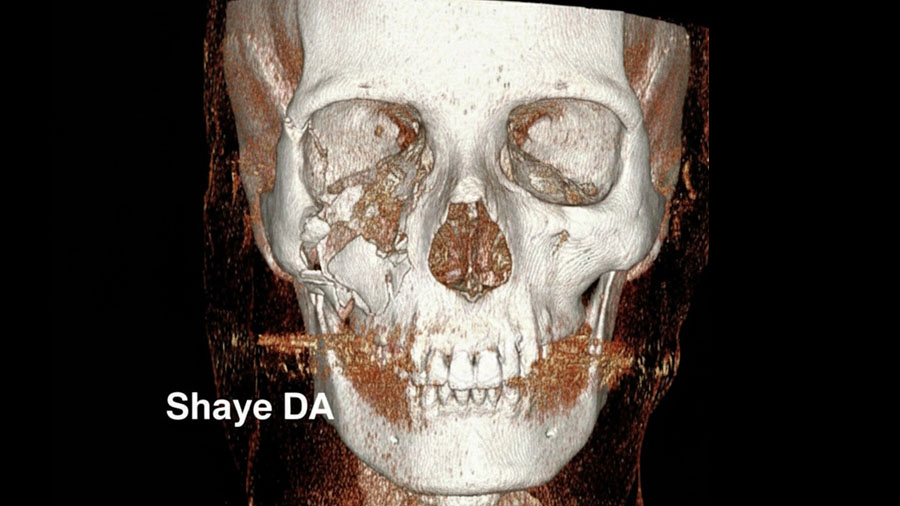
Patient trust is a cornerstone of successful surgical care, and ultimately, the goal of any surgical innovation is to improve patient outcomes. Digital tools, especially 3D reconstructions, have proven to be powerful aids in building that trust. A picture is worth a 1000 words, and a 3D reconstruction illustrates that concept.
When we bring patients into our offices and show them a 3D reconstruction of their own injury—rotating the model to view every angle—we’re not just educating them; we’re building trust. While patients trust their surgeon, they also trust their eyes, and technological tools help us educate patients in their own care.
For instance, the Singerman et al. (2025) paper describes a 34-year-old male with a self-inflicted gunshot wound involving a pan-facial fracture (mandible, maxilla, orbital walls). The VSP workflow produced a 3D printed model of ideal post-reduction anatomy and an occlusal splint, allowing the surgical team to plan meticulously—and then show the patient what “after repair” could look like.
Complex explanations suddenly become clear. Patients can see, in literal terms, why surgery is necessary and what it aims to achieve. This transparency often alleviates anxiety and empowers patients to participate actively in their own care.
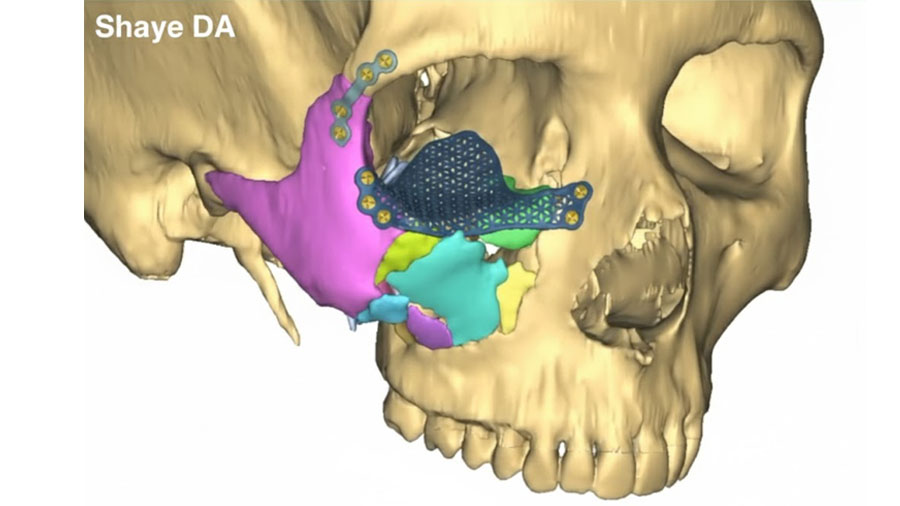
Conceiving repairs before the first incision with VSP
According to Aristotle, “Art indeed consists in the conception of the result before its realization in the material.” VSP enables surgeons to digitally “conceive the repair” prior to incision. By virtually rehearsing the surgery, we may anticipate challenges, optimize our approach, and visualize the result.
Enhancing surgical practices and CMF education in the OR with AR
Augmented Reality (AR) is emerging as a promising tool in both surgical practices and education. By superimposing digital information onto the surgeon’s field of view, AR offers a live feed of critical data during the procedure. This can highlight anatomical landmarks, alert the learner to vital steps, and offer real-time feedback.&
Strong et al. (2025) demonstrated the use of AR for midface osteotomies, midface fracture repair, orthognathic surgery, and mandibular reconstruction. They reported major advantages to be improved visualization of critical anatomy, real time tracking, and 3D visualization of the surgical plan.
Beyond clinical care, the potential for AR in training surgeons is particularly exciting, as it offers a new dimension of experiential learning that is both interactive and immersive.
Technology as an extension—not a replacement—of surgical skill
Technology, however, remains a tool. New tools refine our approaches to care, but do not replace clinical expertise and judgment. Rana et al. (2025) emphasize that, “modern technology complements rather than replaces the clinical expertise and principles established in cranio-maxillofacial surgery”. The best results occur when technology, knowledge, and traditional surgical skills work hand in hand.
A new tailored standard for precision and personalization
Perhaps the most profound change brought by these digital tools is the ability to deliver highly personalized, precise care. Just as a tailor fits clothing to a body, digital workflows enable us to “fit” surgery to the unique anatomy and injury pattern of each patient.
For example, Smolka et al. (2025) utilized a titanium 3D-printed cutting guide for condylar hyperplasia in 8 patients. Virtual mirroring of the healthy side allowed precise definition of how much bone to resect; intraoperative positioning of the guide and resection accordingly led to predictable, personalized outcomes.
Virtual surgical planning allows us to digitally reduce fractures, simulate repairs, and pre-bend plates or design patient-specific implants before stepping into the operating room. This level of preparation means that we are not improvising solutions on the fly; instead, we are executing a well-conceived plan tailored to the individual.
Precise surgery lends itself to less tissue trauma, quick recovery, fewer complications, and better long-term functional and aesthetic results. The ability to plan and execute with such accuracy minimizes guesswork and reduces the margin for error.
The promises digital workflows hold for CMF surgery
Despite the promise of digital workflows, challenges remain. The high cost of new technologies can limit widespread adoption, and the majority of our global population still lacks access to even basic surgical hardware for fracture fixation, let alone advanced digital tools (Shaye et al.,2023). While we push the technological envelope for CMF fracture care, we must simultaneously envision ways that technology could improve access to those in need. The incredibly advances of medicine must progress with the humanity of the profession.
While patient-specific workflows bring benefits, limitations such as costs, required specialized expertise, and necessary imaging remain. Furthermore, turnaround time for PSI production, while decreasing, remains a limiting factor in acute trauma, with a recent study reporting an average of 8.6 days to primary repair with PSIs (Singerman et al. 2025).
Nonetheless, the digital transformation of CMF surgery is well underway. Just as the introduction of plates and screws once revolutionized trauma care, today’s digital technologies are poised to become a new standard. As costs decrease and accessibility improve, these tools will increasingly become more integrated into standards of care. The journey is ongoing, but the direction is clear: a future where technology and surgical expertise work hand in hand for the benefit of every patient.
About the author:
References and further reading:
- Rana, M., Buchbinder, D., Aniceto, G. S., & Mast, G. (2025). Patient-Specific Solutions for Cranial, Midface, and Mandible Reconstruction Following Ablative Surgery: Expert Opinion and a Consensus on the Guidelines and Workflow. Craniomaxillofacial Trauma & Reconstruction, 18(1), 15. https://doi.org/10.3390/cmtr18010015
- Shaye, D. A., Nwosu, O., Ncogoza, I., Nyabyenda, V., Tuyishimire, G., Manana, W., & Taiwo, A. O. (2023). Cost Burden of Rigid Internal Fixation in Craniomaxillofacial Trauma Care in Low- and Middle-Income Countries. OTO open, 7(4), e92. https://doi.org/10.1002/oto2.92
- Singerman, K. W., Morisada, M. V., Kriet, J. D., Flynn, J. P., & Humphrey, C. D. (2025). Virtual Surgical Planning for Management of Acute Maxillofacial Trauma. Craniomaxillofacial Trauma & Reconstruction, 18(1), 18. https://doi.org/10.3390/cmtr18010018
- Smolka, W., Cornelius, C.-P., Obermeier, K. T., Otto, S., & Liokatis, P. (2025). Proportional Condylectomy Using a Titanium 3D-Printed Cutting Guide in Patients with Condylar Hyperplasia. Craniomaxillofacial Trauma & Reconstruction, 18(1), 7. https://doi.org/10.3390/cmtr18010007
- Strong, E Brandon et al. “Augmented Reality Navigation in Craniomaxillofacial/Head and Neck Surgery.” OTO open vol. 9,2 e70108. 11 Apr. 2025, doi:10.1002/oto2.70108
You might also be interested in...
AO CMF Course—Management of Facial Trauma
This course provides learners with the fundamental knowledge and principles for the treatment of craniomaxillofacial fractures and their complications. It covers diagnostic and treatment principles for midface and mandibular fractures, as well as the prevention and treatment of complications.
AO CMF Course—Advanced Management of Facial Trauma
This 2.5-day hands-on course with human anatomical specimens covers complex facial fractures and posttraumatic deformities involving the entire facial skeleton. It focuses on the nasoorbitoethmoidal (NOE) region, including soft-tissue management.
AO CMF Education
AO CMF's courses and events, online learning tools, educational videos, fellowship opportunities and more—designed for craniomaxillofacial surgeons, residents and orthodontists, to enhance their surgical knowledge and skills.