Mandibular fracture complications: a time-based guide for CMF surgeons
BY DR RODRIGO PEREIRA

When it comes to mandibular fracture management, every surgeon knows that complications can, and do, happen. What makes the difference in outcomes is not only technical skill, but also an understanding of when different complications tend to arise. Recognizing these patterns allows clinicians to anticipate, intervene, and guide patients through each stage of recovery. This post breaks down complication timing: immediate, intermediate, and late—with clinical examples, management protocols, and decision-making tips to help every maxillofacial surgeon optimize care.
-
Read the quick summary:
- Dr Rodrigo Pereira explains complication timing in mandibular fractures: immediate, intermediate, and late.
- Proactive recognition and stage-specific management are essential for optimizing outcomes and minimizing long-term morbidity.
- Surgeons benefit by anticipating complications, following evidence-based protocols, and tailoring interventions to the timing and nature of each complication.
- Ongoing discussion centers on clinical vigilance, multidisciplinary care, and continuous learning from real-world cases to improve patient recovery.
Disclaimer: The article represents the opinion of individual authors exclusively and not necessarily the opinion of AO or its clinical specialties.
Immediate complications in mandibular fractures
Immediate complications in mandibular fractures present during the acute phase of trauma. At this stage, the goal is to rapidly identify conditions that may place the patient at risk and influence the sequence of care.
Two main complications tend to dominate the early management of these injuries: airway compromise and hemorrhage/bleeding. Airway compromise may result from blood and secretions accumulating in the oral cavity or oropharynx, soft-tissue edema, hematoma formation in the floor of the mouth, loss of functional tongue support due to detachment of the genioglossus muscle, or the presence of intraoral foreign bodies. Alongside this, hemorrhage can vary in severity from mild to life-threatening, especially if there is an expanding hematoma in the floor of the mouth.
To facilitate early recognition, clinicians should remain alert for key red flags that indicate urgent risk. If any of these warning signs are identified, it is essential to adopt a systematic and thorough approach to assessment and intervention.
Red flags
- Signs of airway obstruction/compromise
- Large amount of blood in the oral cavity with aspiration risk
- Expanding hematoma (especially floor of mouth/submandibular region
What to check first
- Airway patency
- Bleeding: identify the source and control active bleeding/expanding hematoma
- Oral cavity: look for avulsed teeth, bony fragments, and clots that may obstruct; clinically relevant lacerations
- Skeletal instability: comminuted fractures or bony avulsion in the symphyseal region
Intermediate complications in mandibular fractures
Intermediate complications arise days to weeks after trauma or the initial intervention and generally reflect planning issues, technical execution, or fracture-pattern complexity. In this phase, four scenarios account for most clinically relevant problems: inappropriate use of osteosynthesis hardware, comminuted fractures, inadequate alignment and reduction of bony fragments, as well as Injury to anatomic structures.
Inappropriate use of osteosynthesis hardware occurs when the fixation system selected is not compatible with the fracture pattern, increasing the risk of instability and an unfavorable course. Comminuted fractures represent a more complex pattern, with greater difficulty achieving predictable stability. Inadequate alignment and reduction of bony fragments often manifests as occlusal changes such as premature contacts, deviation, and/or open bite, along with signs of instability. Injury to anatomic structures refers to iatrogenic injury to dental and/or neural structures, which may cause complaints such as pain, sensory changes, and persistent dental symptoms.
Given the complexity of the intermediate phase, a high index of suspicion is essential for timely recognition of complications that might otherwise be overlooked. Staying alert to these developments, and knowing what to assess, enables clinicians to intervene before minor issues escalate into major setbacks. The following red flags and focused assessments can help guide early detection and effective management.
Red flags
- Change in occlusion compared with the immediate postoperative period
- Clinical sign of instability (a sense of “shifting/displacement”)
- Pain that does not improve along the expected curve, especially if function-related
- Complaint consistent with an anatomic injury (e.g., persistent neurosensory/dental symptoms)
What to check first
- Occlusion (a sensitive marker of reduction/alignment)
- Anatomic asymmetry
- Fixation strategy: whether the chosen hardware matches the pattern (especially with comminution)
- Anatomic structures: assess and document possible procedure-related injury
Late complications in mandibular fractures
Late complications arise weeks to months after the initial trauma or treatment and can significantly affect long-term function and quality of life.
Among the most relevant scenarios is malunion, where bony healing occurs with inadequate alignment or reduction, leading to malocclusion and deformity. Delayed union is another concern, defined by a lack of consolidation within the expected six to twelve weeks, often caused by instability or unfavorable occlusal loading. Nonunion, or failure of bone healing after eight weeks, may present with persistent mobility and functional impairment.
Infection is also a notable late complication, frequently associated with ongoing fracture instability, retained teeth in the fracture line, insufficient soft-tissue coverage, or loss of fixation. It can result in pain, swelling, fistula formation, and involvement of adjacent tissues.
Finally, TMJ ankylosis, though rare, represents a high-impact outcome characterized by a progressive reduction in mouth opening and functional limitation. It may develop weeks to months after condylar trauma and/or a local inflammatory process, with gradual worsening of function.
Because late complications often develop gradually, their recognition depends on careful follow-up and a focus on subtle but clinically significant changes. Monitoring specific warning signs and conducting targeted assessments can help clinicians identify issues before they become entrenched or difficult to treat. The following red flags and key points of evaluation are especially important when late complications are suspected:
Red flags
- Persistent malocclusion beyond the period when union should be occurring (especially >6–8 weeks)
- Bony mobility or a sensation of “bone movement”
- Active purulence
- Progressive reduction in mouth opening
- Plate exposure (osteosynthesis hardware exposure)
What to check first
- Occlusion and function: document occlusal pattern, masticatory complaint, and perceived asymmetry
- Stability: assess mobility at the fracture site and pain with function
- Signs of chronic infection: fistula, drainage, recurrent swelling, soft-tissue status
- Imaging: determine presence/absence of bony union and the position of osteosynthesis materials
- TMJ: measure maximal mouth opening, deviation, and temporal evolution (progression = warning)
- Soft tissues: dehiscence, hardware exposure
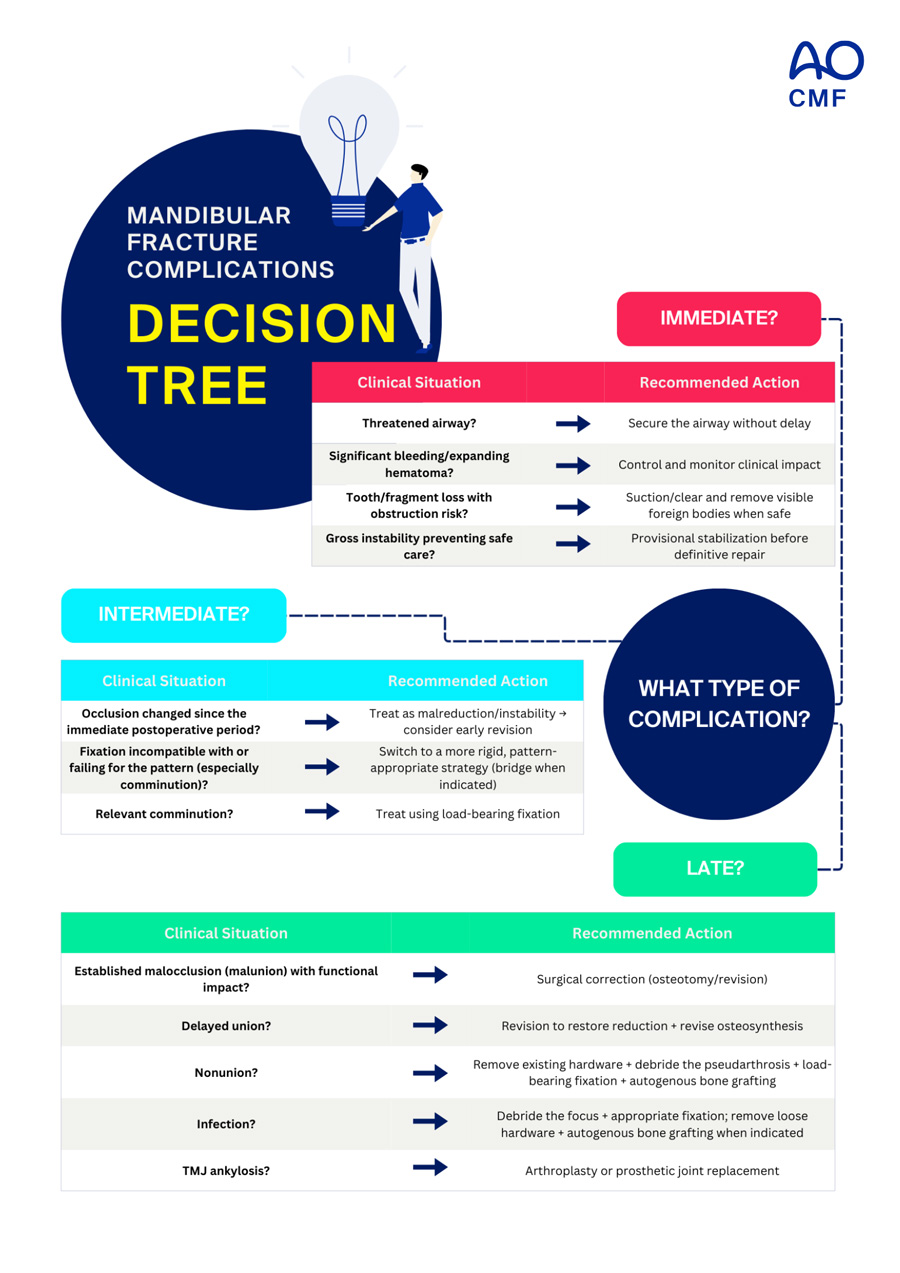
Decision trees and evidence-based protocols
In practice, managing complications in mandibular fractures is about making reproducible decisions based on a few key clinical axes. Once the phase of the complication and the failure pattern are defined, treatment becomes a set of objective choices: when to observe and protect, when to revise early to restore stability and reduction, and when to proceed to reconstructive revision.
Below is a direct “problem → decision” guide to support decision-making:
AO Surgery Reference provides stepwise algorithms for hardware selection, fixation strategy, and complication management. Decision-making should always consider patient comorbidities, bone quality, and functional demands.
Case examples and lessons learned
Real-world cases reveal the diverse and often complex challenges in managing mandibular fractures complications. Each highlights the technical precision and clinical judgment required for successful outcomes and reminds us that even expertly executed care can face complications, especially in severe trauma or difficult anatomy.
Clinical examples and the spectrum of complications:
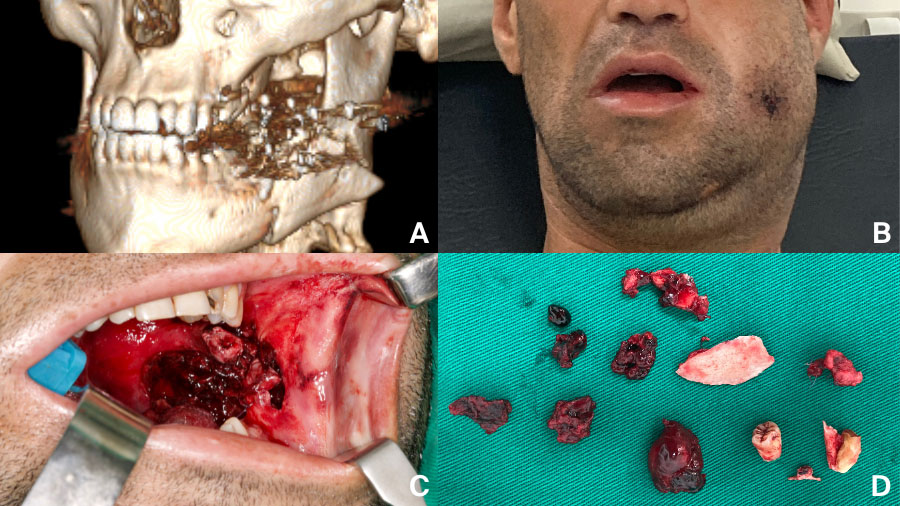
- Gunshot injuries often demand immediate airway control and staged reconstruction.
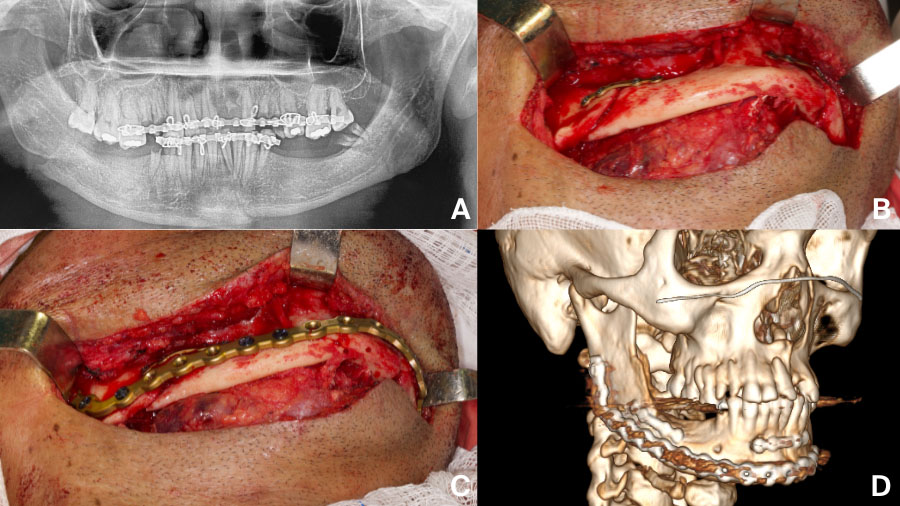
- Comminuted or atrophic fractures require load-bearing plates and generous exposure.
- Malunion after inadequate fixation may be salvaged with revision surgery
- Nonunion
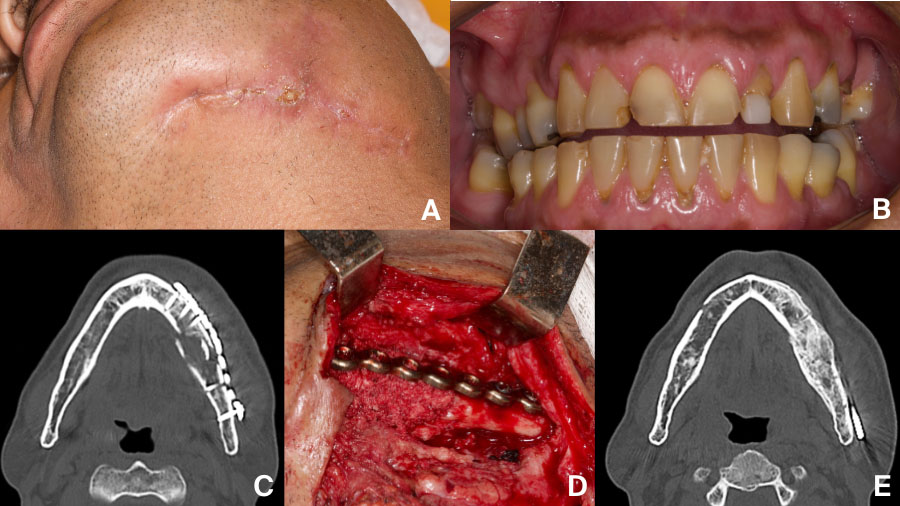
- Persistent infection is often a sign of instability or hardware failure
Reflecting on these cases, it becomes clear that complications are not always a reflection of suboptimal care, but frequently stem from the complexity of the injury and the limitations of current techniques. The most important lessons are the value of early recognition, proactive intervention, and continuous learning, each of which plays a critical role in achieving the best possible outcomes for patients.
Proactive complication management for better outcomes
Time-based awareness of complications in mandibular fracture care empowers surgeons to anticipate and address challenges at every stage. Understanding when, and why, complications arise supports better decision-making, timely intervention, and improved patient outcomes. Surgeons who recognize the full spectrum of each phase of mandible fracture complications, are best positioned to guide their patients safely through recovery and back to function.
About the author:
References and further reading:
- Punjabi AP, Thaller SR. Late complications of mandibular fractures. Opertive Tech Plastic Reconst Surg 5:226-274, 1998. DOI: 10.1016/S1071-0949(98)80019-X
- Alpert B. Management of the complications of mandibular fracture treatment. Opertive Tech Plastic Reconst Surg 5:325-333, 1998. DOI:10.1016/S1071-0949(98)80038-3
- Ostrander BT, Wang HD, Cusano A, Manson PN, Nam AJ, Dorafshar AH. Contemporary Management of Mandibular Fracture Nonunion-A Retrospective Review and Treatment Algorithm. J Oral Maxillofac Surg 76: 1479-1493, 2018. DOI: 10.1016/j.joms.2018.01.027
- Mehra P, Van Heukelom E, Cottrell DA. Rigid internal fixation of infected mandibular fractures. J Oral Maxillofac Surg 67:1046-1051, 2009. DOI: 10.1016/j.joms.2008.12.036
- Alpert B, Tiwana PS, Kushner GM. Management of comminuted fractures of the mandible. Oral Maxillofac Surg Clin North Am 21:185-192, 2009. DOI: 10.1016/j.coms.2008.12.002
- Pereira RDS, Albieri F, Maikon de Sousa Santos A, Martins RDS, Pessanha IL, Mourão CF. Is Active Purulence Associated With the Success of Particulate Autogenous Bone Grafting in the Reconstruction of Post-traumatic Mandibular Defects? A Retrospective Cohort Study. J Oral Maxillofac Surg. 2025 Nov;83(11):1381-1392. DOI: 10.1016/j.joms.2025.07.002
You might also be interested in...
Management of Facial Trauma
This course provides learners with the fundamental knowledge and principles for the treatment of craniomaxillofacial fractures and their complications.
Advanced Management of Facial Trauma
This 2.5-day hands-on course with human anatomical specimens covers complex facial fractures and posttraumatic deformities involving the entire facial skeleton.
Management of facial trauma resources
Explore AO's resources on CMF trauma surgery, from structured curricula and educational events to clinical tools, videos, blog posts, and research.