A neurosurgical voyage through an unprivileged world—the everyday battle and how to bring about change
Career planning in neurosurgery—an ever changing, highly competitive, and thrillingly vibrant specialty—is not something one does once and for all. Research and technological innovations drive new trends in the field, making a career with a focus on rural neurosurgery hardly a mainstream or a popular choice. It requires an out of the box approach and extra effort to overcome barriers.
Succeeding in any continuously evolving workplace environment requires rigor and battle with challenges, and I have experienced this from early life. Working in remote areas in an unprivileged world, where I saw either no health care structure at all or an insufficient one, I witnessed human misery, myths based on ignorance, and a ruling class completely cut off from the needs of people.
There is a dearth of innovation in science, technology, and health services and an abundance of trauma caused by bad planning, infections such as tuberculosis and poliomyelitis, and unnecessary suffering in pregnancy due to poor health and lack of nutrition, leading to congenital problems such as neural tube defects.
This is the everyday reality for people in any third world country. But new strategies could accelerate change and provide for "health for all". Let me explain.
Roadblocks add to patients' misery
Around five billion people worldwide lack access to basic surgical care and most people in low and middle-income countries (LMICs) struggle to access neurosurgical services at all. This means limited access to trained medical, nursing, and allied health staff, lack of equipment, and availability of services at a reasonable distance.
The lack of resources, planning, investment, population surge, and being disconnected from research leave the underprivileged part of our world even more exposed.
To give an idea, the WHO has set a standard of one neurosurgeon for 100 000 people, which is still a far-off dream. In East African countries, 10–15 million people have theoretically access to one neurosurgeon and most of the rural population must travel hundreds of miles to see one.
General and family physicians are the foundation for appropriate referrals. In the absence of working health care systems, patients end up wasting valuable time in multiple rounds and often lose the window for treatment.
Insurance and government support systems are non-existent or insufficient in many developing areas, and the exponential population growth can break down any existing strategies facilitated to the public. Health care facilities in the private sector focus on diagnostic equipment for quick returns of investment. The lack of attention and support for clinicians on human resources, operating setups, and modern equipment provision further add to the miseries of patients. Professionals working and utilizing governmental facilities, perks, privileges—titles, and academic support do not restrict to one place—don’t usually allow private practitioners to contribute services under the government-based rules.
Ironically, most professionals eventually leave the country for better opportunities.
The retention of trained professionals is a major issue. Migration to urban areas or overseas is the usual end point in the absence of due support and opportunities.
What needs to change to achieve health for all
Locally, academia and industry have no interaction and are disconnected, but turning this around could provide a major leap forward. The lack of research for local and inexpensive solutions leads to inaccessible care for those in need: There are plenty of resources but what is needed is proper prioritization leading to long term plans and finally realistic solutions for a “health for all” vision.
The burden of neurological disease leading to morbidities and mortalities is a leading concern; these disorders affect the whole family and eventually the country take the brunt. The rising financial burden can be statistically calculated, but the psychological impact and its long-term negative consequences are being ignored and not yet measured.
No system can sustain a population explosion without long term planning or support from insurance and the governments.
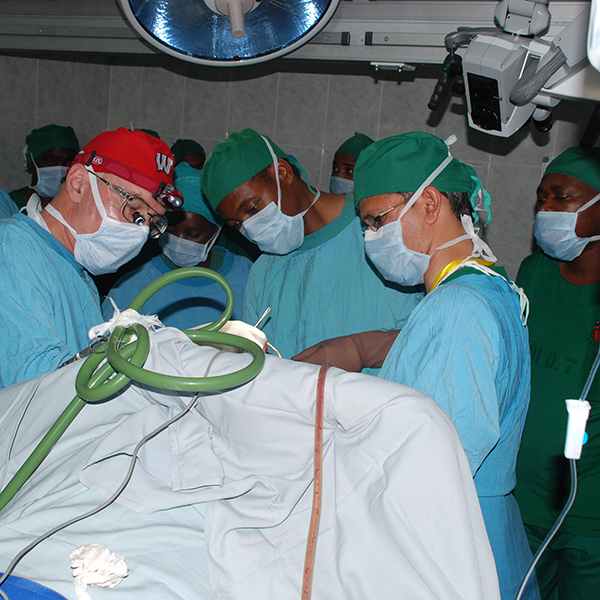
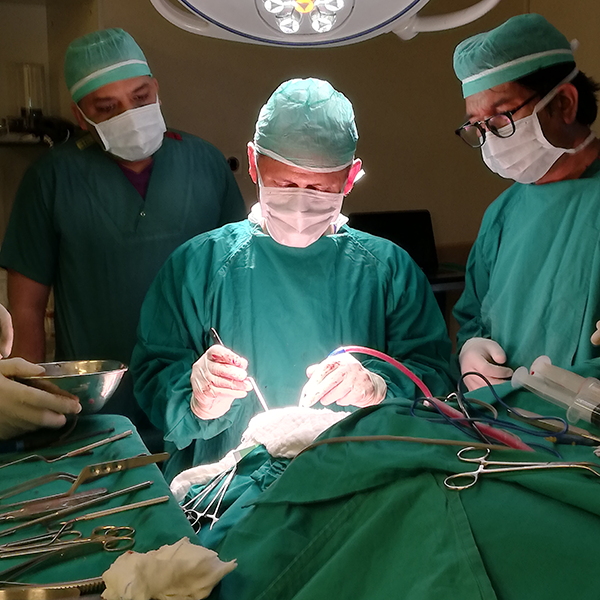
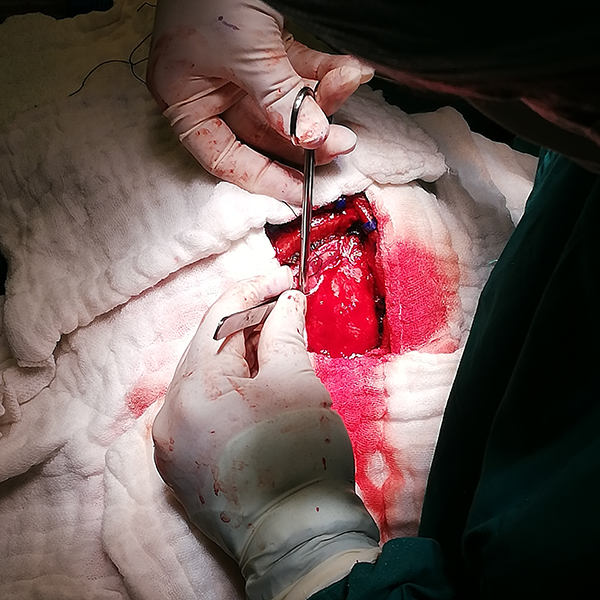
Performing brain tumor surgery in South City Hospital, Karachi, Pakistan
Importantly, planning and human resource provisions for the future need neurosurgeons' and spine surgeons' input. Moreover, lack of reliable data leads to authorities building these services inappropriately. Clinicians face severe challenges regarding provision of adequate neurosurgical services and workforce and access to care, equipment, and training needs are seen worldwide as the areas to be prioritized.
Most of the modern equipment come at a high cost, with taxes and maintenance rapidly making them too expensive and unrealistic for the available budgets. Processes of procurement are frustratingly slow for the end users. In the current corporate culture, employers aim to attract, hire, and retain employees who provide the best monetary value, considering professionals a business and a product to sell, and creating a marketing strategy to sell in the mainstream.
Companies work with local representatives with sole distribution rights. Unfortunately, most of the time, there is nothing in stock and there are no alternatives available.
This kind of market monopoly is another major concern. As an example, for the 220 million strong population of Pakistan and our many spinal and neuro-centers, leading companies don’t have a presence, while the procurement process is ill-defined, expensive, and patchy. The role of middlemen leads to difficulties when the sole distributor focuses on their own interest and there is no well-defined mechanism for feedback.
Parallel to the above, increasing public awareness is important. Teaching our school-going children about road safety, positive lifestyle strategies, back care, first-aid training, identifying stroke prevention, signs of stroke, and so on are vital and preventive strategies should be the basic step. Prehospital care and budget planning are necessary to boost general physician, family physician, emergency specialty, ICU, and neurorehabilitation specialties.
There is a lot to be done on many fronts, but the vision is clear, and the road forward is mapped: my aim is to establish a collaboration structure and work for LMIC in collaboration with first world-based organizations, institutes, and authorities.
About Dr Atta Ul Aleem Bhatti, my story
“Witnessing these harsh realities were the hallmark of my early education in Tharparkar Sind, a remote desert area of Pakistan. My parents had migrated from the mountains of Srinagar, Kashmir—a landscape full of natural beauty with cool temperatures—to a desert where summers were harsh at over 40 degrees Celsius. Throughout their lives they served the community by teaching to primary school children in extremely difficult situations faced by poor population in interior Sindh.
Later, I managed to get medical education and early surgical training from Ayub Medical College, Abbottabad. It was located at the scenic doorstep to the Karakoram Mountains—the home to K2. This area has five of the world's fourteen 8'000-meter-high mountains, and 100 peaks towering above 7'000 meters. The historic road Shahrah-e-Resham (Silk Road) from Pakistan to China through Khunjrab Pass still marks its face in front of the Ayub Medical College Abbottabad.
Moving on to fulfilling my dream to become a neurosurgeon, I joined Aga Khan University Hospital (AKUH) in Karachi—an institute realizing Prince Karim Aga Khan’s vision for raising education and health in Pakistan. The institute of post graduate medical education (PGME) awarded me graduate residency training in 2007. After a few months, the college of physician and surgeons of Pakistan (CPSP) awarded me an FCPS degree in neurosurgery. For next two years I kept working as an instructor neurosurgeon at AKUH focusing mainly on operative neuro spine surgery, clinical management, training of nurses, interns, and resident doctors.
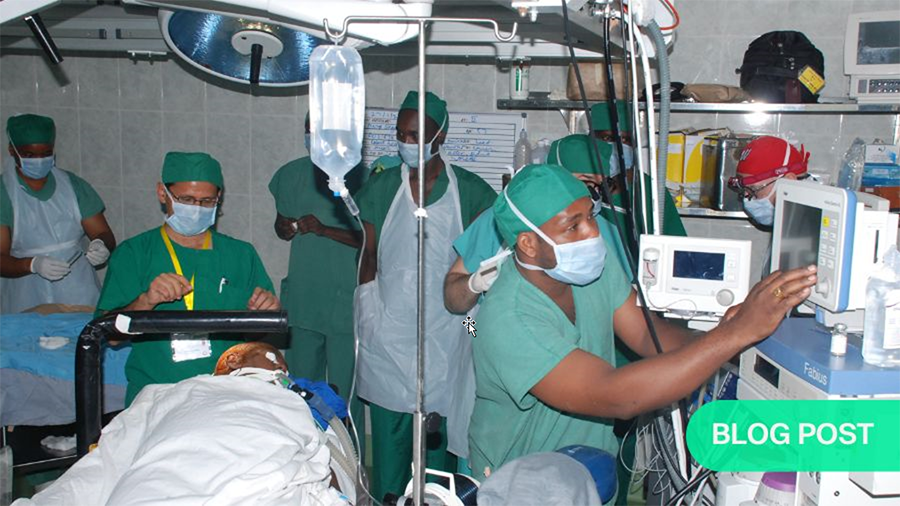
At that point I decided to take a leap forward towards becoming an independent professional. Previously I had been moving between north and south of Pakistan. While this time I was lucky to have an adventure of going to a different part of the world. In 2010, I moved to East Africa through Aga Khan Health Services. I was fortunate to establish the first private sector neurosurgery unit at Agha Khan Hospital in Dar es Salaam, Tanzania.
Moving on to exploring another continent, I got an opportunity to complete a 2-year fellowship (2011–2013) in endovascular neurosurgery / interventional neuroradiology from the University Hospital Zurich in Switzerland.
I feel fortunate to have been able to avail the opportunities of completing short term fellowships in micro-neurosurgery, spine, vascular, neuroradiology, neuroanatomy, neuro-oncology from INI, Hanover; Montpellier, France; and HUS, Helsinki.”
Disclaimer
The articles included in the AO Spine Blog represent the opinion of individual authors exclusively and not necessarily the opinion of AO Spine or AO Foundation.