The particulate iliac crest bone graft: An overlooked alternative for mandibular reconstruction
BY DR CARLO FERRETTI

-
Read the quick summary:
- Dr Carlo Ferretti advocates for particulate iliac crest bone graft as a superior, underused option for mandibular reconstruction, especially in benign conditions and trauma.
- Particulate grafts better restore arch form and height, reduce morbidity, and avoid many limitations of free flaps and block grafts.
- Surgeons can benefit from two-stage protocols, posterior iliac crest harvest, and combining autograft with growth factors for large defects or pediatric cases.
- Ongoing debate emphasizes individualizing reconstruction plans, reducing unnecessary morbidity, and rethinking the dominance of free flap techniques.
Disclaimer: The article represents the opinion of individual authors exclusively and not necessarily the opinion of AO or its clinical specialties.
The surgical status quo: Free flaps for mandibular reconstruction
It has become surgical dogma that the reconstruction of mandibular segmental defects must be done with a free vascularised flap, (most commonly the fibula) particularly if the linear length of the defect exceeds 6cm. The latter restriction is based on flawed assumptions, has no basis in biology, has been repeatedly shown to be false and should be permanently abandoned.
Whilst a free flap is undoubtedly an unavoidable treatment for a patient who has needed the removal of bone and soft tissue, for a patient with bone only defect (such as resections for benign pathology and trauma) use of free flaps confers only disadvantages in exchange for little benefit. The impact of harvesting a free flap creates greater patient morbidity and impact on quality of life than the harvest of a particulate graft from the posterior iliac crest.
Moreover, the bulk of soft tissue co-transferred (even with the most conservative fibula harvest) creates on-going problems when implants are to be placed in the reconstructed mandible. To this must be added the challenge of adapting a tubular, straight bone to the mandibular arch form. A rough approximation of arch form can be achieved with multiple osteotomies of the fibula, but a persistent and more difficult problem to solve is the height deficiency of the fibula in comparison to the mandible it replaces.
The challenge of mandibular arch form
As with most surgical reconstruction the technologies of 3D imaging, virtual planning and CAD/CAM manufacture of implantable devices ensures that the form of the metal mandibular reconstruction plate closely follows the facial form.
When a fibula reconstruction is used, the reconstruction philosophy is reversed: the tubular fibula bone is adapted not to the desired facial form, but the closest facsimile achievable within the limitations imposed by osteotomy numbers of the fibula. In instances where a free flap is obligatory, these compromises must be made and accepted, but if these exigencies do not exist then accepting compromises in mandibular morphology are unnecessary and unacceptable.
Non-vascularised grafts: Block vs particulate
Many surgeons have reported excellent results with non-vascularised grafts in the form of a free block (although this type of graft IS often plagued by significant post implantation resorption), but reports of block graft treatment often conclude with the caveat that non-vascularised block grafts should be limited to mandibular defects that are truly lateral (the biological rationale for this proviso is unclear). It is quite probable that this restriction is because non-vascularized block grafts have the same drawback as the fibula: adaptation to the mandibular arch form is difficult.
Advantages of the particulate iliac crest graft
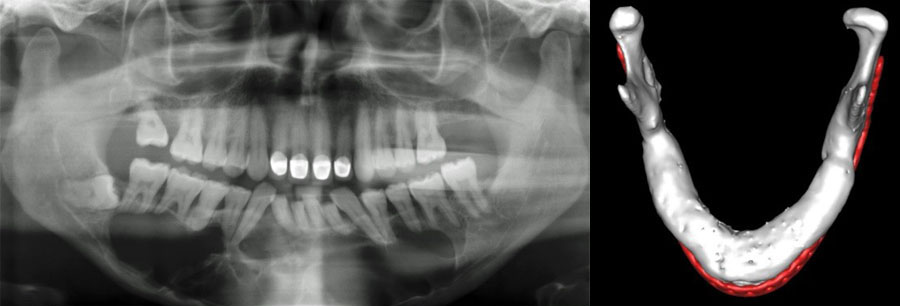
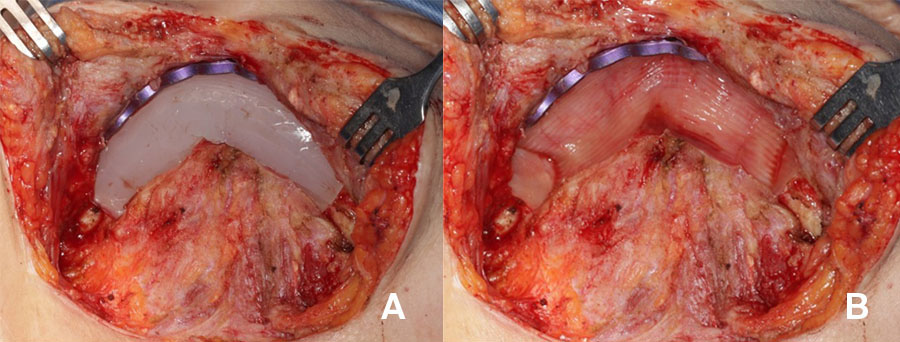
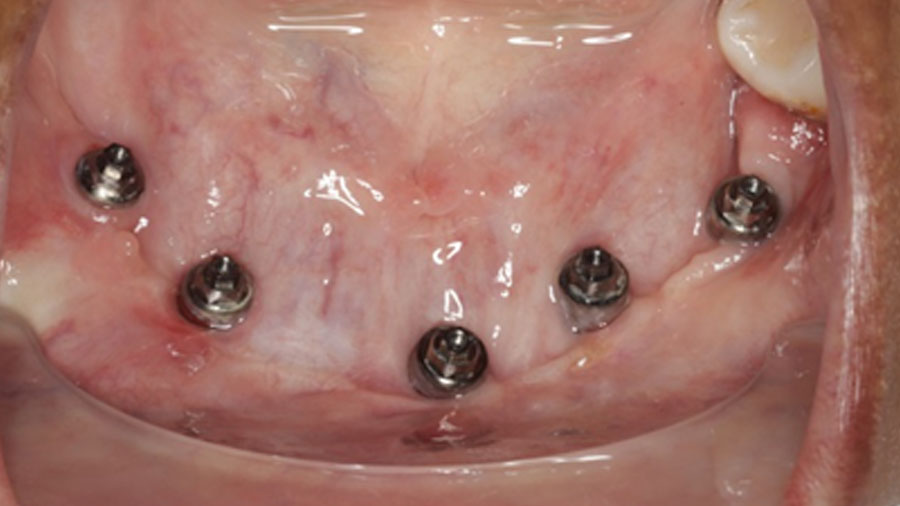
In contrast the particulate, compressed, autologous bone graft overcomes many of these challenges. Due to its mouldable properties it adapts to an arch and allows for the superior restitution of mandibular arch form and alveolar height (Figure 1), whilst significantly reducing patient morbidity and treatment costs.
Staged approach: Reducing risk and improving outcomes
Although a particulate graft can be completed concurrent to ablation surgery, I hold the view that this approach confers excessive risk for salivary contamination and graft loss due to sepsis. Two stage treatment avoids this risk, but does mean that definitive reconstruction must occur at a second surgery. To avoid salivary contamination the graft must be placed via an extraoral approach once the oral mucosa has healed and so the graft implantation bed needs to be developed in the previously operated site. This creates a technical challenge and to facilitate graft bed development at second surgery a silicone spacer is implanted at the time of primary surgery which serves to maintain a space into which the particulate graft is introduced. It will also sculpt the shape of the recipient bed and guide the shape of the ossicle.
Biological basis of the particulate graft
The biology of the particulate graft differs from the block graft which explains the different clinical performance but the details thereof are beyond the scope of this overview.
To summarize, the particulate graft should be considered a cellular transplant (within a mineral matrix replete with growth factors), and it is the high cellular concentration and cellular survival (by diffusion gradients from the soft tissue bed) that confers on the compressed, autologous, particulate graft its superior regenerative properties. Survival of the cellular populations responsible for bone deposition, resorption and maintenance ensures that coupled bone formation can continue uninterrupted post transplantation. Defect length is thus immaterial, but successful regeneration relies on an adequate volume of autologous bone.
It has been my experience that attempting to avoid the inconvenience of posterior iliac crest harvest and harvesting from the anterior crest yields an inadequate bone volume harvest and failure of ossicle formation. As a minimum, a mandibular defect will require 5g of wet bone mass per linear centimetre of mandibular defect. In cases where autologous bone is insufficient graft expansion may be successfully done by combining with an osteogenic growth factor (such as BMP-2 or TGF-β) delivered on a suitable matrix.
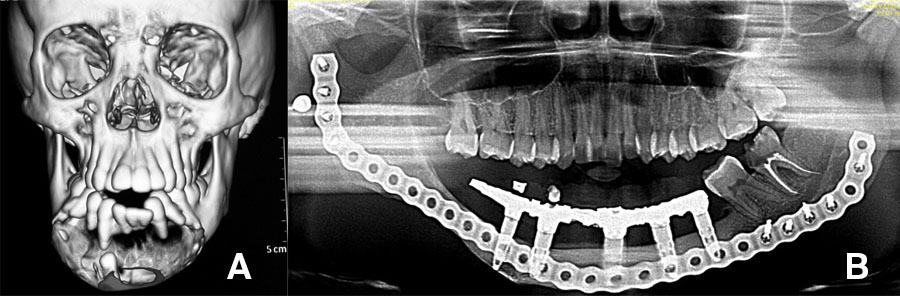
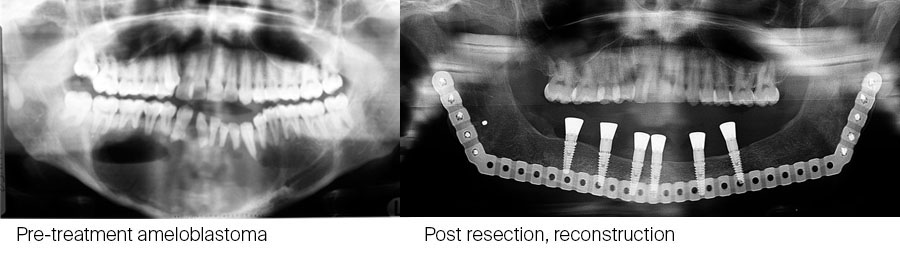
This is particularly useful in children with large defects. An example of such a case illustrated below: CT scan of 10-year-old with large ameloblastoma (A). Panoramic radiograph (B) 13 years post reconstruction and 7 years post implant placement and dental rehabilitation. Patient grafted at age 10 with a composite graft of autologous bone and TGF-β3 loaded onto DBM (demineralized bone matrix).
Sample case and treatment protocol
To illustrate a typical protocol a brief overview of the treatment algorithm will be useful:
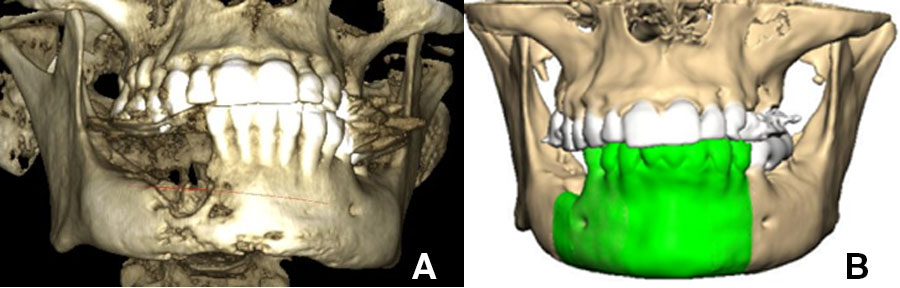
Images of 3D CBCT scan of patient with advanced osteomyelitis of the mandible (A). Virtual planning (B) is required to produce either a pre-bent or milled patient matched plate.
First surgery: resection of affected mandible segment, placement of plate and silicone spacer.
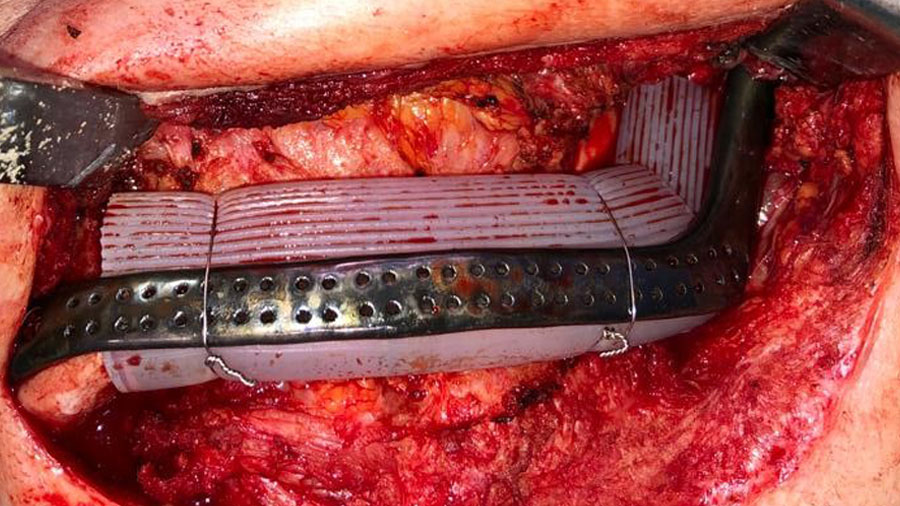
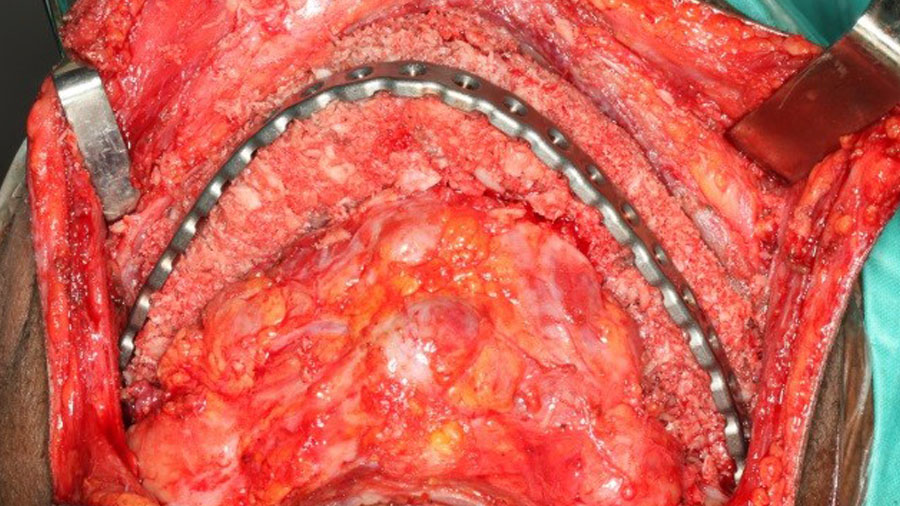
Second surgery: Following a minimum of 8 weeks (but can be later if needed) definitive reconstruction surgery ensues. The defect is exposed of via extra-oral approach (A), and the silicone spacer is removed to reveal a richly vascularised soft tissue bed hermetically isolated from the oral environment (B).
Harvest of posterior iliac crest – 5 grams of wet weight per linear centimetre of mandible defect.
The graft is morselized in a power bone mill, compressed in a syringe and implanted into the defect. The typical length of hospitalization after a posterior iliac crest harvest and mandibular reconstruction is no more than 3 days.
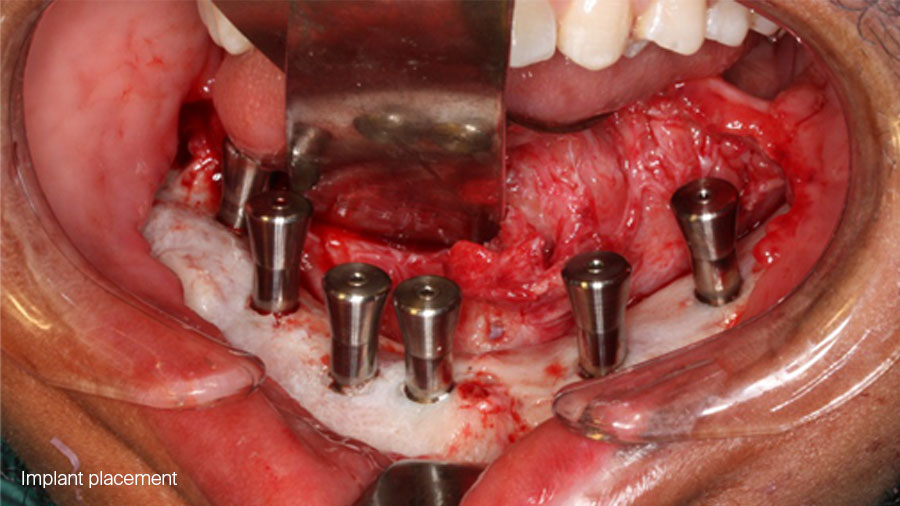
6 months later ossicle maturation is complete and planning and execution of implant placement can be done in the traditional manner.
Rethinking mandibular reconstruction philosophy
The inappropriate enthusiasm for single surgery in mandibular reconstruction (such a jaw-in-day) forces patients to have treatment that carries far worse morbidity, compromised results and often ongoing problems particularly with peri-implant soft tissues around free flaps.
For patients who may require radiotherapy and whose long-term prognosis is poor, expeditious completion of surgical treatment may be necessary and force one to accept the compromises and morbidity associated with this approach.
However, if we consider that reconstructions for benign pathology and trauma may need to survive for many decades the philosophy of a staged approach which allows for superior long-term rehabilitation should be considered when feasible. It remains an under-utilized option despite its superior reconstructive results and reduced morbidity.
It is my contention that it should be the empirical first choice reconstruction for all defects following trauma and benign pathology that should be more widely deployed for the benefit of all our patients.
About the author:
You might also be interested in...
Reconstructive Surgery in Head and Neck
Learn state-of-the-art reconstructive techniques using a variety of free and pedicled flaps
AO CMF reconstructive surgery resources
From structured curricula and educational events to clinical tools, videos, blog posts, and research
AO Surgery Reference: Mandible
A resource for the management of patient issues (AO CMF member privilege)
Craniomaxillofacial Trauma & Reconstruction
An international, peer-reviewed, open access journal covering head, face, and jaw research