Atlantoaxial instability—decision options in the modern era
BY DR MITCHELL NG AND DR GREGORY SCHROEDER

Atlantoaxial instability (category II Type C of the AO Spine Upper Cervical Classification Injury) remains one of the most challenging pathologies in cervical spine surgery. The C1–2 articulation is responsible for ~50% of cervical rotation, which explains both the high degree of mobility normally and the substantial clinical effects of instability at this level.1
Clinical indications for surgical treatment of C1–2 instability
There are a wide range of indications for operative intervention, which include: acute trauma (e.g. odontoid fractures, transverse ligament disruption), rheumatoid arthritis, congenital anomalies (e.g. os odontoideum), and infection/neoplasm.2 Since spontaneous stabilization is not commonly possible, surgical fixation is frequently required.
-
Read the quick summary:
- AO Spine surgeons review atlantoaxial instability, focusing on indications, biomechanics, and modern C1–2 fixation strategies.
- Goel–Harms fixation offers reliable fusion, safety, and versatility; transarticular screws remain useful in select anatomy.
- Surgeons gain a practical decision framework for selecting fixation techniques based on stability, anatomy, and risk.
- Standardized classification and terminology remain essential to improve diagnosis, research comparability, and outcomes.
Disclaimer: The article represents the opinion of individual authors exclusively and not necessarily the opinion of AO or its clinical specialties.
Nonoperative vs operative management of atlantoaxial instability
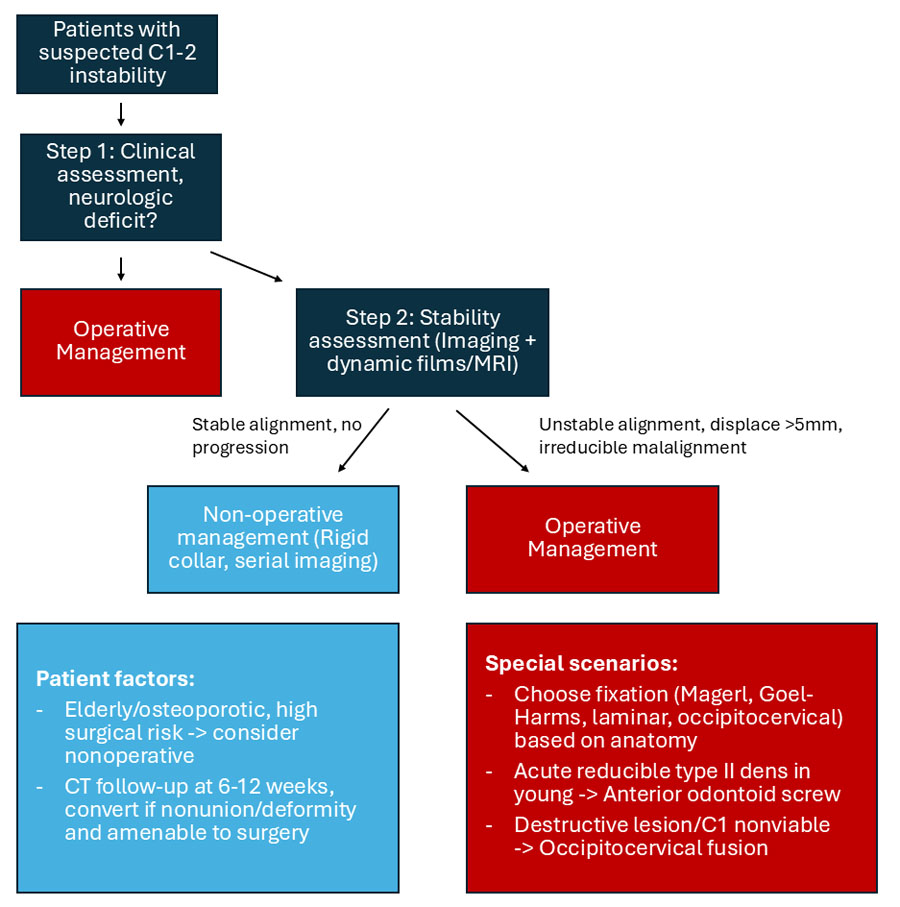
The first step in managing atlantoaxial instability is deciding whether nonoperative care is a reasonable option.3 In select cases, typically stable fractures without neurological deficit, patients may be managed with a rigid collar or halo, though nonunion is a frequent concern, especially in elderly or osteoporotic individuals.4–6 When there is clear instability, progressive deformity, or neurological compromise, surgery is the more reliable path (Figure 1).
Historical evolution of C1–2 fixation techniques
The evolution of C1–2 fixation has been marked by steady progression toward constructs able to both reliable and overall greater stability7. Early wiring techniques such as those described by Gallie and Brooks were straightforward to perform but had significant biomechanical limitations (e.g. poor rotational control) leading to high rates of nonunion.8 A recent global survey of AO Spine members revealed that 0/24 (0%) routinely utilize wiring techniques.
Transarticular screw fixation (Magerl Technique): benefits and risks
The introduction of Magerl’s posterior transarticular screw fixation in the 1980s was a significant advancement to wiring techniques. Fusion rates of 95–100 percent were reported, and the technique provided a construct strong enough to obviate the need for external immobilization9,10. However, notably Magerl’s method requires anatomical reduction of C1–2 before placement of screw, and anatomical variations limit its use.11 Specifically, ~18–22% of patients are not candidates due to a high-riding or anomalous vertebral artery.12,13 Overall, the ~5% risk of vascular injury has certainly tempered enthusiasm for its routine application.14
Goel–Harms Construct: the modern workhorse for C1–2 fusion
The Goel–Harms construct, involving C1 lateral mass screws connected to C2 pedicle or pars screws by rods, has since emerged as the workhorse technique.15–17 It allows for intraoperative reduction of malalignment, avoiding the most potentially dangerous transarticular trajectories, and has demonstrated excellent fusion rates with fewer vertebral artery complications.18 Although exposure can be technically demanding and average blood loss is somewhat higher compared with transarticular fixation, the safety margin and versatility of this approach have made it the preferred option in many centers worldwide.19,20
Alternative posterior fixation strategies in complex anatomy
Other posterior constructs retain important roles in select cases. On the one hand, the C2 laminar screw technique provides a safe alternative in patients with small pedicles or high-riding arteries, with biomechanical properties sufficient for reliable fusion when paired with C1 fixation.21,22 When C1 is destroyed or unsuitable for instrumentation, or when instability extends cranially, occipitocervical fusion remains the recommended option.23
On the other hand, for patients with acute, reducible type II odontoid fractures and good bone quality, anterior odontoid screw fixation remains a potential option, and is the only method preserving motion at the C1–2 segment.24,25 Unfortunately, this option is limited to younger patients with favorable anatomy, outcomes are poorer in older patients, diagnosis of osteoporosis, or with a chronic fracture nonunion.26,27
Decision-making framework for C1–2 surgical fixation
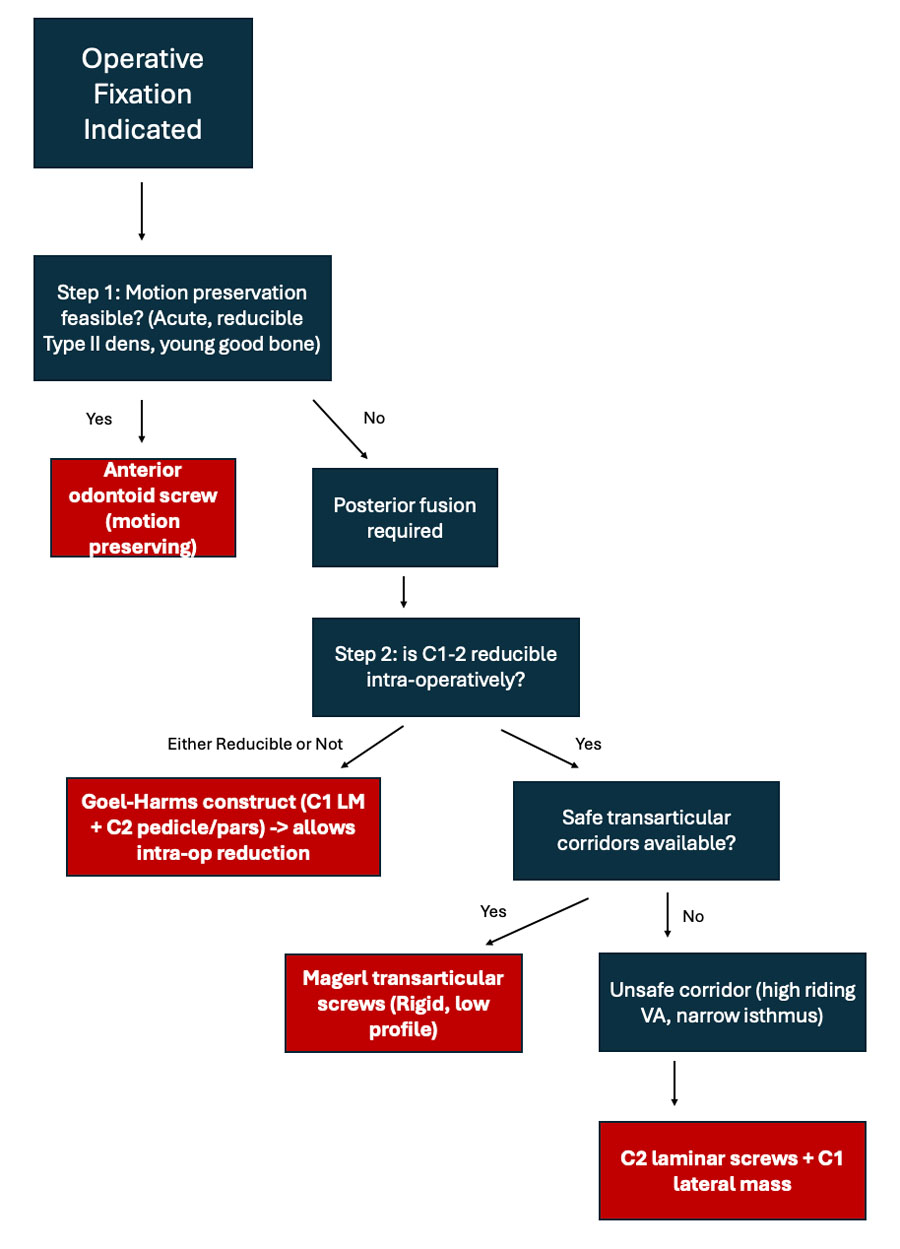
In practice, decision-making for C1–2 fixation follows a relatively consistent sequence. Surgeons must first determine whether motion preservation is possible, which is feasible only in the small subset of patients amenable to odontoid screw fixation.
In most cases, posterior fusion is required, and the choice between transarticular and Goel–Harms fixation depends on vertebral artery anatomy, reducibility of the joint, and surgeon preference.28 Once operative indication has been determined, listed below is one potential decision-making algorithm regarding surgical technique (Figure 2).
Author’s preferred surgical strategy: Goel–Harms fixation technique
In our practice, the Goel–Harms construct has become the standard method for addressing atlantoaxial instability.15,19,20 This configuration (C1 lateral mass screws connected with C2 pariscle (pars/pedicle) or laminar screws using short rods) provides excellent fixation and avoids potentially dangerous transarticular trajectory that carries a small risk of vertebral artery injury. Although in certain instances we consider use of transarticular screws with ideal anatomy and an easily-obtainable reduction, in our hands the Goel–Harms technique offers the safest most reliable solution for the vast majority of patients.
Preoperative planning: vertebral artery assessment and imaging
A preoperative CT angiogram or MRI is required to trace the course of the vertebral arteries (V3) and determine whether C2 can accommodate parsicle screws. Intraoperatively, the patient is positioned prone in a Mayfield head holder on a radiolucent Jackson table, maintaining the neck in neutral or slight extension. After midline incision from the subocciput to C3 spinous process, a subperiosteal exposure is carried caudal to the posterior arch of C1 and to lamina of C2, preserving soft-tissue attachments when possible.
C1 lateral mass screw placement: surgical technique
Starting point for C1 lateral mass is determined by palpating the medial border of the C1–2 joint with a key elevator and moving roughly two burr-widths lateral corresponding to the center of the lateral mass and aligning with the C2 screws below (see below).29 When considering visualization of C1 lateral masses, C2 nerve roots are identified and can be gently mobilized. Of note, if there is substantial bleeding from paravertebral/pararadicular venous complex, sacrificing C2 roots may improve visualization and access without long-term effects.
As mentioned, there should be preoperative knowledge of vertebral artery course, which typically travels laterally through the foramen transversarium before entering the sulcus arteriosus on the superior surface of the posterior arch. Thus, surgical dissection and the screw starting point must remain below the C1 posterior arch, with knowledge of potentially anomalous courses.
Bleeding from the paravertebral/pararadicular venous plexus is very common and is controlled with lateral suction while avoiding unnecessary exposure toward the laterally based vertebral artery. A Penfield #4 dissector can retract the C2 root medially during drilling and tapping.
Fluoroscopic guidance is always used throughout for cranial/caudal angulation. On the lateral view, the screw is aimed toward the anterior tubercle of C1, with trajectory angled 5-10 degrees medially toward midline. A 1.7 mm burr can be used to open the cortex/make starting point, advancing under fluoro, ball-tip probe to palpate walls/floor of pilot channel followed by a 3.0 mm conical tap under fluoroscopy and ball-tip probe again. Typically, a 3.5 mm × 30 mm screw (20 mm threaded, 10 mm smooth) is placed.
C2 parsicle screw fixation: hybrid strength and safety
Our preferred technique for C2 fixation is the parsicle screw, a combination of the pars and pedicle screw.30 We believe this hybrid construct combines the biomechanical strength of a pedicle screw with the safety (more medial starting) profile of a pars screw.
The starting point is located just cranial to the C2–3 facet joint and 4 mm inferior and medial to the traditional pedicle screw entry site. The cortex is breached with a 1.7 mm burr, and a Penfield 4 is placed medially to be aware of the location of the spinal canal. The trajectory is typically angled 15-20 degrees medially and 30-45 degrees cranially, always being sure to remain in the dorsolateral quadrant of the pedicle to maximize the distance from the vertebral artery.
The channel is tapped with a 3 mm tap, and walls are palpated with a ball-tip probe before inserting a 3.5-4.0 mm screw (20–26 mm length). Optimal purchase occurs after about 10 mm, when the screw crosses the lamina and engages the dorsal cortex of the pedicle.
The parsicle screw offers excellent cortical contact with overall biomechanical stability, while typically maintaining excellent alignment with the C1 screws above. To this end, it is especially valuable tool in cases of high-riding vertebral artery, narrow pedicle corridor, or revision surgery where standard pedicle screws may be unsafe.
Final C1–2 construct assembly and fusion strategy
After screw placement, short rods are contoured and secured to C1/C2 screws, allowing compression across the grafted joints to achieve reduction and firm bone contact. We then decorticate the C1 posterior arch and C2 lamina and apply additional bone graft along these surfaces. A rigid collar is worn postoperatively for comfort, but rigid internal fixation alone provides sufficient stability for fusion.
C1–2 transarticular screw (Magerl technique)
The Magerl transarticular screw remains an option for atlantoaxial fixation in anatomically suitable patients.31 Preoperative CT angiography is mandatory to exclude a high-riding vertebral artery. In addition, this approach is ideal when reduction is easily achievable preoperatively, otherwise a Goel–Harms construct is preferred. The typical starting point is located on the posterior aspect of the C2 inferior articular process, ~3–4 mm cranial to the C2–3 facet joint and 2–3 mm medial to its lateral border. The trajectory is angled 20-30 degrees cranial in the sagittal plane and 10–20 degrees medially, aiming toward the C1 anterior arch.
Under fluoroscopy, a hand drill is advanced from C2 bypassing the C1–2 joint (trans-articular) into the C1 lateral mass, ending just beneath the anterior cortex. The track is palpated with a ball-tip probe before tapping and screw insertion. Typical screw dimensions are 3.5–4.0 mm in diameter and 38–44 mm in length, depending on patient size. Bicortical fixation across the C1-2 joint provides immediate stability.
Conclusion: balancing stability, safety, and anatomy
Although the specific surgical technique chosen is ultimately subject to institutional culture and individual surgeon experience, the overall framework recommended is clear: balance the biomechanical requirements of stability with the anatomical risks posed by each trajectory. With careful patient selection, modern techniques have C1-2 fusion reliable and reproducible.
Despite advances in surgical technique, atlantoaxial instability terminology and treatment remains inconsistent. We encourage routine adoption of standardized classification systems (e.g. AO Spine Upper Cervical Injury Classification) to improve diagnostic clarity, enable meaningful outcome comparison, and facilitate consistent communication among providers and patients alike.
About the authors:
References and further reading:
- Charbonneau L, Watanabe K, Chaalala C, et al. Anatomy of the craniocervical junction — A review. Neurochirurgie 2024;70:101511.
- Bransford RJ, Alton TB, Patel AR, et al. Upper cervical spine trauma. Journal of the American Academy of Orthopaedic Surgeons 2014;22:718–29.
- Goel A. Indicators of atlantoaxial instability. J Craniovertebr Junction Spine 2021;12:103–6.
- Cho SK, Safir S, Lombardi JM, et al. Cervical Spine Deformity: Indications, Considerations, and Surgical Outcomes. Journal of the American Academy of Orthopaedic Surgeons 2019;27:E555–67.
- Bransford RJ, Alton TB, Patel AR, et al. Upper cervical spine trauma. Journal of the American Academy of Orthopaedic Surgeons 2014;22:718–29.<
- Jiang SH, Wang RK, Sadeh M, et al. In-hospital outcomes following surgery versus conservative therapy in elderly patients with C2 fractures: a propensity score–matched analysis. J Neurosurg Spine 2024;41:498–507.
- Hajek PD, Lipka J, Hartline P, et al. Biomechanical study of C1-C2 posterior arthrodesis techniques. Spine (Phila Pa 1976) 1993;18:173–7.
- Dickman CA, Crawford NR, Paramore CG. Biomechanical characteristics of C1–2 cable fixations. J Neurosurg 1996;85:316–22.
- Bahadur R, Goyal T, Dhatt SS, et al. Transarticular screw fixation for atlantoaxial instability - modified Magerl’s technique in 38 patients. J Orthop Surg Res 2010;5:87.
- Easton R. Atlantoaxial fixationwith transarticular screws—Magerl technique. Oper Tech Orthop 1998;8:13–5.
- Wang C, Yan M, Zhou H, et al. Atlantoaxial transarticular screw fixation with morselized autograft and without additional internal fixation: technical description and report of 57 cases. Spine (Phila Pa 1976) 2007;32:643–6.
- Madawi AA, Casey ATH, Solanki GA, et al. Radiological and anatomical evaluation of the atlantoaxial transarticular screw fixation technique. J Neurosurg 1997;86:961–8.
- Lee JH, Jahng TA, Chung CK. C1-2 transarticular screw fixation in high-riding vertebral artery: Suggestion of new trajectory. J Spinal Disord Tech 2007;20:499–504.
- Sonone S, Dahapute AA, Waghchoure C, et al. Anatomic Considerations of Anterior Transarticular Screw Fixation for Atlantoaxial Instability. Asian Spine J 2019;13:890.
- Lvov I, Grin A, Talypov A, et al. Efficacy and Safety of Goel-Harms Technique in Upper Cervical Spine Surgery: A Systematic Review and Meta-Analysis. World Neurosurg 2022;167:e1169–84.
- Goel A, Desai KI, Muzumdar DP. Atlantoaxial Fixation Using Plate and Screw Method: A Report of 160 Treated Patients. Neurosurgery 2002;51:1351–7.
- Harms J, Melcher RP. Posterior C1-C2 fusion with polyaxial screw and rod fixation. Spine (Phila Pa 1976) 2001;26:2467–71.
- Sharma JK, Kalidindi KKV, Sangondimath G, et al. Clinicoradiological outcomes of Goel and Harms fixation for atlantoaxial instability: An institutional experience. Surg Neurol Int 2020;11:189.
- Gelinne A, Piazza M, Bhowmick DA. Minimally invasive modification of the Goel-Harms atlantoaxial fusion technique: a case series and illustrative guide. Neurosurg Focus 2023;54:E14.
- Jain AK, Tawari M, Rathore L, et al. An experience with Goel-Harms C1-C2 fixation for type II odontoid fractures. J Craniovertebr Junction Spine 2022;13:175.
- Reddy C, Ingalhalikar A V., Channon S, et al. In vitro biomechanical comparison of transpedicular versus translaminar C-2 screw fixation in C2-3 instrumentation. J Neurosurg Spine 2007;7:414–8.
- Clifton W, Garcia JO, Damon A, et al. Freehand C2 Laminar Screw Placement: Technical Note and Operative Video. Cureus 2019;11:e5549.
- Joaquim AF, Osorio JA, Riew KD. Occipitocervical Fixation: General Considerations and Surgical Technique. Global Spine J 2019;10:647.
- Tyagi G, Patel KR, Singh GJ, et al. Anterior Odontoid Screw Fixation for C2 Fractures: Surgical Nuances, Complications, and Factors Affecting Fracture Union. World Neurosurg 2021;152:e279–88.
- Joaquim AF, Patel AA. Surgical treatment of Type II odontoid fractures: anterior odontoid screw fixation or posterior cervical instrumented fusion? Neurosurg Focus 2015;38:E11.
- White AP, Hashimoto R, Norvell DC, et al. Morbidity and mortality related to odontoid fracture surgery in the elderly population. Spine (Phila Pa 1976);35. Epub ahead of print April 2010. DOI: 10.1097/BRS.0B013E3181D830A4.
- Harrop JS, Przybylski GJ, Vaccaro AR, et al. Efficacy of anterior odontoid screw fixation in elderly patients with Type II odontoid fractures. Neurosurg Focus 2000;8:1–4.
- Bourdillon P, Perrin G, Lucas F, et al. C1-C2 stabilization by harms arthrodesis: Indications, technique, complications and outcomes in a prospective 26-case series. Orthopaedics & Traumatology: Surgery & Research 2014;100:225–31.
- Lin JM, Hipp JA, Reitman CA. C1 lateral mass screw placement via the posterior arch: a technique comparison and anatomic analysis. The Spine Journal 2013;13:1549–55.
- Kepler CC, Fang T, Bronson WH, et al. The C2 “Parsicle” Screw. Clin Spine Surg 2020;33:146–9.
- Bahadur R, Goyal T, Dhatt SS, et al. Transarticular screw fixation for atlantoaxial instability - modified Magerl’s technique in 38 patients. Journal of Orthopaedic Surgery and Research 2010 5:1 2010;5:1–8.
You might also be interested in...
AO Spine Classification Systems
AO Faculty have developed detailed classification systems for spine injuries, osteoporosis, tumors, infections, and deformity.
AO Surgery Reference
Check out the Spine Trama module on this detailed resource for the management of fractures, based on current clinical principles, practices and available evidence.
AO Spine Trauma Curriculum Courses
Globally respected educational programs, developed and taught by leading experts, and grounded in the latest evidence.
Knowledge Forum Trauma and Infection
Leading the globe in generating the knowledge that improves patient care after suffering from spine trauma and infection.