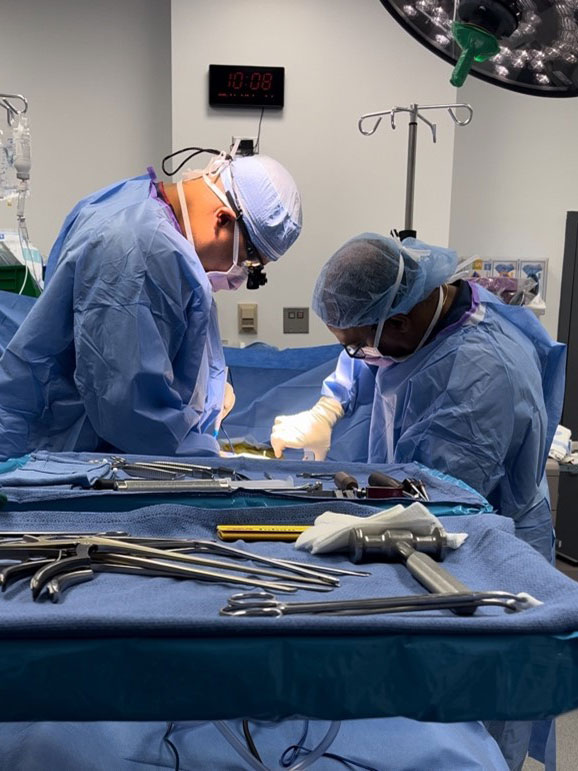
Awake Spinal Fusion—introducing the Rapid Recovery Spine Surgery protocol
BY DR ALOK SHARAN
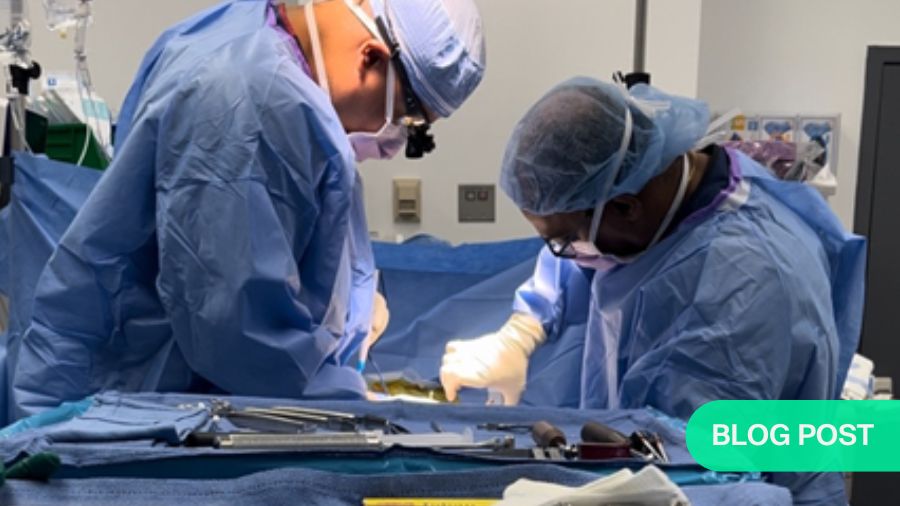
There have been tremendous advancements in the field of spine surgery over the past few decades. The advent of newer types of instrumentation along with techniques for placing instrumentation has increased the capabilities of what can be performed in spine surgery. Less invasive techniques, along with robotics and navigation systems, have made the placement of this instrumentation safer. And finally, there has been a tremendous concentration of research on factors outside of the operating room, including the use of Enhanced Recovery After Surgery (ERAS) protocols, that have led to improved outcomes and changed the paradigm for recovery. Awake Spinal Fusion represents the next major advancement in the evolution of spine surgery.
Disclaimer: The article represents the opinion of individual authors exclusively and not necessarily the opinion of AO or its clinical specialties.
Awake Spinal Fusion is a protocol that uses newer techniques of regional anesthesia to perform lumbar spine surgeries. By avoiding general anesthesia and using newer regional blocks, patients are able to recover safer, better, and faster after spine surgery.
The transition to using regional anesthesia vs general anesthesia has occurred in many other surgical specialties. It is very common for our hand colleagues to perform surgery with the patient wide awake. Knee replacements are routinely performed under spinal anesthesia, allowing the patients to mobilize quickly after surgery.
It has taken the spine surgery community a longer period to adopt the principles of regional anesthesia. In 1959 a publication from the Henry Ford Hospital demonstrated the efficacy of spinal anesthesia for lumbar spine surgery. (1) Since then, there have been many publications demonstrating the efficacy of axial blockade for lumbar surgeries. (2)
From lumbar laminectomy to lumbar fusion
For me the use of regional anesthesia in lumbar fusions started as a personal journey. I had been performing lumbar laminectomies using spinal anesthesia for many years when a patient with an L4–5 spondylolisthesis presented to my office. She was a widow and had been suffering from significant pain in her back down her legs. Having failed a course of non-operative treatment she knew that she needed surgery but was hesitant to proceed because of the side effects from general anesthesia. She had undergone a shoulder surgery in the past but had developed delirium for a few days after that surgery. This was consistent with the results of many studies that have demonstrated the higher incidence of post-operative delirium in elderly individuals after general anesthesia vs regional anesthesia. (3,4)
When I transitioned my practice to using spinal anesthesia for lumbar laminectomies, I had noticed that my patients had been experiencing a tremendous recovery. They were experiencing less pain after surgery, required less narcotics, and were able to leave the hospital faster. It was clear that the avoidance of general anesthesia allowed patients to recover faster.
I discussed this protocol with our patient, and she enthusiastically signed up for surgery. Using spinal anesthesia along with sedation we were able to perform a minimally invasive lumbar fusion on her. She tolerated the procedure well and was safely able to go home the next day. As we continued to transition our patients to the use of regional anesthesia, we were seeing tremendous outcomes in our patients after spinal fusion surgery.
Improved outcomes with Thoracolumbar Interfascial Plane Block
The next advancement in our protocol came after a publication by Dr Hand et al in 2015 describing the thoracolumbar interfascial plane block (TLIP) block (5). This was a novel regional anesthetic technique that blocks the branches of the dorsal rami nerve, the branches that innervate the paraspinal muscles. As part of our Awake Spinal Fusion protocol, we began to perform the TLIP block prior to surgery. There was clearly a difference in patients who had received the TLIP block—so much so that many of our patients began to ask for same day discharge after surgery. For patients who had received spinal anesthesia along with a TLIP block we noticed decreased narcotic usage along with faster mobilization after surgery.
By avoiding general anesthesia patients were less confused after surgery, they experienced less nausea and vomiting, and had less delirium. Together we noticed that patients were recovering faster after surgery and had improved outcomes. The convalescence period we typically observe for our patients after spinal fusion was shortened – which led to a faster recovery and faster discharge.
Recently we have integrated the addition of pre-operative and post-operative IV infusions of amino acids into our protocol. It is common for patients to be nutritionally deficient prior to surgery. There has been tremendous literature demonstrating that patients who are nutritionally optimized prior to surgery have better healing rates. Recent publications in the total joint replacement literature have also demonstrated that an infusion of certain amino acids can help improve muscle mass, improve quadriceps size and strength, and ultimately lead to a quicker recovery. (6) This ultimately leads to faster mobilization and recovery after a total knee replacement.
Using that information we have incorporated the administration of IV amino acid infusions prior to surgery. This is leading to reduced inflammation, faster mobilization, and less need for pain meds.
At this point, for many of our patients who undergo a minimally invasive lumbar fusion, we are able to routinely discharge them home within a few hours. As part of the protocol, we minimize how much narcotics they use and instead encourage the use of OTC pain meds. There have been instances now where patients take minimal to no narcotics after spinal fusion surgery. By doing so patients are developing less side effects from surgery including nausea, vomiting, and confusion.
Currently our Rapid Recovery protocol for Spinal Fusion consists of:
- IV Infusion of Amino Acids
- Spinal Anesthesia using isobaric Marcaine
- TLIP Block
- Minimally Invasive Lumbar Fusion
- Minimal Narcotics – Encourage OTC Meds
- IV Infusion post-op
Using this protocol the majority of our spinal fusion surgeries are performed on an outpatient basis. Many patients are discharged within 4 hours after surgery. We typically give pain meds for 48 hours only and encourage patients to use OTC meds for pain control. Walking is encouraged soon after with the initiation of physical therapy within two weeks after surgery.
The use of regional anesthesia has transformed many surgical procedures within orthopedics and other surgical specialties. This has allowed surgery to be safer and allow for faster recovery. For me, personally, our Awake Spinal Fusion protocol is leading to improved patient satisfaction, faster mobilization, and an overall better patient experience after spinal fusion surgery.
Awake spinal fusion represents a protocol that incorporates the use of regional anesthesia for lumbar spine procedures. By avoiding general anesthesia and using regional blocks patients who need a spinal fusion are safely able to go home the same day and minimize the use of narcotics after surgery.
About the author:
Dr Alok Sharan, MD, MHCDS, is an Orthopedic Spine Surgeon who is a pioneer of the Awake Spinal Fusion procedure, the latest advancement in minimally invasive spine surgery. He is a leading authority both nationally and internationally on the Awake Spinal Fusion procedure, having been invited to give presentations throughout the United States and many countries around the world. He is the President and Founder of the Spine and Performance Institute, a practice devoted to providing personalized and holistic care for individuals who suffer from spinal disorders. Dr Sharan has received numerous academic distinctions for his research with over 100 publications, abstracts, and book chapters. He has co-edited a textbook entitled Basic Science of Spinal Diseases.
References and further reading:
- Ditzler J, Dumke P, Harrington J, DeWitt F. Should spinal anesthesia be used in surgery for herniated intervertebral disk? Anesthesia & Analgesia 38(2):p 118-124, March 1959.
- McLain RF, Kalfas I, Bell GR, Tetzlaff JE, Yoon HJ, Rana M. Comparison of spinal and general anesthesia in lumbar laminectomy surgery: a case-controlled analysis of 400 patients. J Neurosurg Spine. 2005 Jan;2(1):17-22.
- Postoperative delirium in older adults: best practice statement from the American Geriatrics Society. J Am Coll Surg. Feb 2015;220(2):136-48.e1.
- Tow A, Holtzer R, Wang C, Sharan A, Kim SJ, Gladstein A, Blum Y, Verghese J. Cognitive Reserve and Postoperative Delirium in Older Adults. J Am Geriatr Soc 64:1341–1346, 2016.
- Hand William R, Taylor Jason M, Harvey Norman R, Epperson Thomas I, Gunselman Ryan J, Bolin Eric D, Whiteley Joseph. Thoracolumbar interfascial plane (TLIP) block: a pilot study in volunteers. Can J Anaesth. 2015 Nov;62(11):1196-200
- Ueyama H, Kanemoto N, Minoda Y, Taniguchi Y, Nakamura H. 2020 Chitranjan S. Ranawat Award: Perioperative essential amino acid supplementation suppresses rectus femoris muscle atrophy and accelerates early functional recovery following total knee arthroplasty. JBJS Br VOL. 102-B, No. 6 Supple A, June 2020.
You might also be interested in:
AO Spine Guest Blog
Find more innovative approaches to spine surgery directly from the AO Spine community and highlight your own work.
The AO Spine Knowledge Forums
Get to know the engines of AO Spine clinical research and find the latest knowledge to make your patients and practice flourish.
AO Spine sponsored Focus Issues
Collections of treatment recommendations, hot topics, and current controversies in spine care produced by AO Spine and the Knowledge Forums.
Global Spine Journal
AO Spine’s official scientific journal, the first truly fully Open Access journal in the field of spine surgery with an Impact Factor.