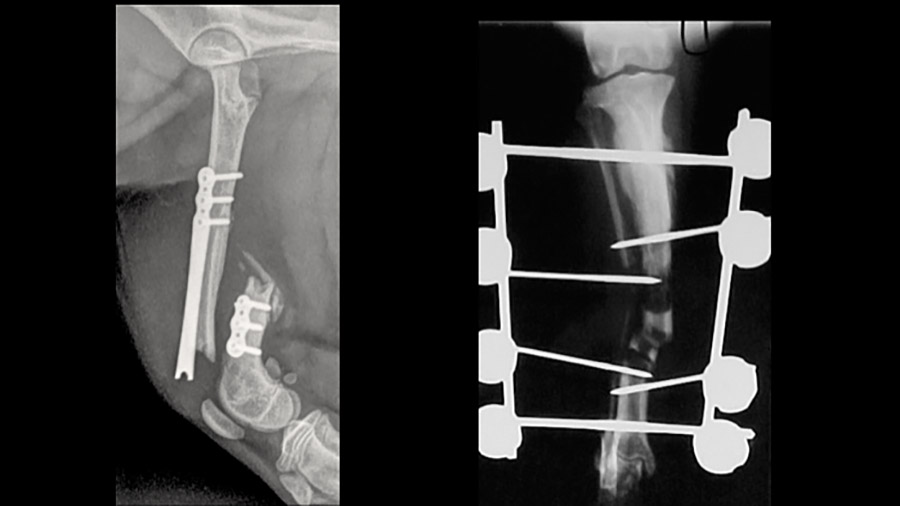
How to avoid and manage complications in veterinary surgery
WITH BRUNO PEIRONE

Learning—and practicing—under the guidance of experienced master veterinary orthopedic surgeons is key to gaining the necessary experience to avoid complications, says AO VET faculty member Bruno Peirone. In combination with state-of-the-art technique and good- quality implants, experience can drive complications down to an acceptable rate, he explains.
Peirone, who has practiced for 35 years, says one simple question is the foundation of managing complications.
“The most important thing to consider in managing complications is, ‘Why did it happen?’ This begins the analysis of the complication. What we are trying to teach is, number one, an understanding of why a complication occurred and, number two, what we have to do to solve it,” he says. “So, you look at mechanics, biology, and then a strategy for revision.”
The master veterinary orthopedic surgeon is quick to point out that 99 percent of complications are surgeon-related—a difficult pill for some surgeons to swallow but essential to driving down complication rates.
“The surgeon is mainly responsible for any complications. That’s not easy for surgeons to accept because it requires a retrospective analysis and admitting that they made a mistake but that’s the key to understanding why a complication occurred,” he says.
Improving patient outcomes
Over the course of his career, Peirone has seen the emergence of bone substitutes, more robust locking plate technology, and more effective antibiotics—all of which make important contributions to improved patient outcomes.
“Many things have changed during my career: We have many bone substitutes available that we didn’t have in the past, so if a complication results in bone loss, you can replace that with bone substitute,” he says. “We have better, more robust locking plates that add stability, and we have better antibiotics to fight infection. All of these add up to better patient outcomes.”
Peirone says less time on the operating time also reduces complications, and that’s where technologies like 3D printing can make a valuable difference.
“When you’re facing a complex bone deformity or complex fracture, you can send the patient to the computed tomography (CT) scan and from the CT scan you can produce a 3D-printed bone model that you can practice on—for example, bending the plate the day before the surgery,” he says.
“Then, when you come into surgery, you’re already prepared. In corrective osteotomy, 3D printing can be helpful not only in terms of generating a model of a crooked bone, but also in production of a cutting guide—and this saves a lot of time. We know that one of the most common causes of complication is the duration of the surgery—if it goes longer than two hours, the risk increases.”
Performing better surgical techniques also reduces complication rates, Peirone says.
“A complication may occur, but if the surgeon sticks to the principles, the complication rate becomes an acceptable 2–3 percent,” he said.
Experience counts
Young surgeons often don’t appreciate the important role that experience plays when attempting a veterinary orthopaedic surgery.
“A young surgeon may not be able to do that kind of surgery but is eager to do it and may not realize that the learning curve goes very slowly and you need mentoring,” Peirone explains, adding that when analyzing fractures, young surgeons need to be able to correctly assess the situation. “You need to be able to make a correct judgment of the fracture, ‘Am I able to fix it or not?’ If you can’t or if you’re unsure, it’s always better to refer the case to a more experienced surgeon.”
Second, he says, is the ability to judge whether a fracture is anatomically reducible.
“You can have to ask which kind of osteosynthesis—rigid and stable or more elastic—is most appropriate. If you correctly answer the first question—whether the fracture is anatomically reducible—then you will sort out the corrective technique,” says Peirone. “One of the most common mistakes is mixing the principles—applying the wrong technique to a given fracture.”
‘Cool down’ when facing complications
Moreover, when encountering a complication, maintaining a cool head is essential.
“The best way to react to a complication is to cool down. If you react suddenly and immediately, you can create another complication and create a domino effect,” he notes. “Cool down, ask what went wrong, and consider how to solve the problem. Don’t act instinctively or ignore the complication. For instance, when you’re putting in a prosthesis and reaming the femur, and you hear a crack—indicating a femural fissure—don’t ignore it just because you don’t want to think about the femoral fissure. That just creates an even worse complication.”
Canine total hip replacement is another procedure where remaining calm in the face of complication can make a huge difference.
“When you’re inserting the stem in the femur, if you have an issue and ignore it, the dog will have a full fracture,” says Peirone. “If you understand that there was a fissure, you often can resolve it intraoperatively. This is where developing skills over time, and with mentoring, is so very important.”
The value of a solid preoperative plan
Having a solid preoperative plan, including all instruments and implants that might be needed to deal with complications, is indispensable, Peirone says.
“If you don’t have everything you need, you can end up closing the surgical site without any success,” he explained.
Most postoperative complications involve implant failure, screw pullout, infections, delayed union or nonunion, Peirone adds, noting that the correct response depends on the complication itself.
“If the complication is infection, you do the surgery within one or two hours in a sterile operating room and a well-prepared surgeon and team,” he says. “For implant failure, the risk of complication is mainly related to the quality of the implant and how you apply it, and for the bone healing process, nonunion is typical if the surgical footprint is too severe on the soft tissue therefore limiting the vascular supply. The worst-case scenario is when you have to perform an amputation—but it’s very uncommon. Only after discussion with the owner do we go ahead with an amputation; it’s always bad, but our patients have four limbs, and a dog with three legs can have an acceptable quality of life.”
The myAO advantage
It isn’t always easy to openly discuss topics like complications and worst-case scenarios, but myAO— the AO’s proprietary digital network of trauma and orthopedic surgeons around the world—provides a secure place to exchange knowledge with peers and experts.
“On myAO, surgeons can discuss taboos, which are those cases that didn’t go well—a case with complications. These are the cases that you wouldn’t normally present in a big auditorium because it’s about your reputation,” Peirone says. “On myAO, we have an AO VET group about complications, with very specific case sharing.”
Peirone says that because myAO is a global community, it reduces the distance between members and provides greater accessibility to the resources—including expertise—that veterinary orthopedic surgeons need.
“Our clinical division is a benchmark for the others: Most of AO VET’s myAO users are younger than 40. They are digital natives who are used to using websites and apps to exchange knowledge,” says Peirone.
In addition to his legacy as an AO VET faculty member and his work as chairperson of the AO VET Community Development Commission (July 2021 to July 2023), Peirone has recently been involved in the design of new Synbone bone models that demonstrate complications.
“With Synbone in 2021, we created five spatial models mimicking the most common complications and these models were used during the AO VET Masters Course—How to Avoid, Recognize, and Manage Complications in Small Animal Fracture this year in Cremona, Italy,” says Peirone who chaired that 2022 course.
The ‘magic’ of the Cremona masters courses
The annual AO VET masters courses in Cremona hold a special place in Peirone’s heart: He has been involved in them from their inception 15 years ago and he has seen first-hand how they have evolved as an educational opportunity that today includes networking and leisure activities among participants and faculty.
“We always have two courses: one about limb alignment such as skeletal deformities and patellar luxation—and another course which this year was complications in veterinary orthopedic trauma. The Cremona courses were inspired by limb alignment courses by two United States surgeons, and I have been involved with the Cremona courses from the beginning,” he says.
Beyond Cremona’s easy-to-get-to location in northern Italy’s Lombardy region, the course venue—the historic Trecchi Palace—is part of the event’s allure, Peirone says.
“The magic of these courses is that we have a very nice venue that mimics an operating room and we can do practical exercises on models and cadaveric specimens,” he says. “Then we can take the postoperative radiographs of participants’ surgeries and have a general discussion, and that’s a big tool for education because participants can see what they did and we as faculty can critique. It really is a rare opportunity for participants. At the Cremona courses, we are filling the gap between what we teach and what the participants will practice after the courses. Of course, we as faculty always learn something by exchanging ideas with our colleagues, and the questions from participants are always useful.”
The annual Cremona courses are also memorable for the camaraderie that has developed among faculty members.
“We have one day off between the two courses and all of the speakers like to ride bicycles, so we take a bike tour of the city together,” he said. “It’s a nice way to spend some time together—not just teaching and practicing.”