Understanding the physeal spike complex in equine athletes
BY DR BARNY FRASER

The physeal spike complex represents an intriguing but impactful source of lameness in performance horses, most commonly involving the distal radius. Although relatively uncommon, these osteochondromata and exostoses can produce significant clinical signs by impinging on soft tissues within the adjacent tendon sheath. Their diagnosis and management require careful interpretation of imaging, a detailed understanding of regional anatomy, and a thoughtful, minimally invasive surgical approach. Given their importance in racehorses and other high‑performance equine athletes, it is essential that clinicians recognize the presentation, interpret diagnostic findings accurately, and apply effective treatment strategies to optimize outcomes.
-
Read the quick summary:
- Dr Barny Fraser explains the physeal spike complex and its role as a source of lameness in performance horses, especially at the distal radius.
- Spikes and osteochondromata can damage the deep digital flexor tendon, create inflammation, and cause secondary tenosynovitis leading to significant clinical signs.
- Equine clinicians benefit from recognizing clinical presentation, using appropriate imaging, and applying minimally invasive tenoscopic treatment to improve outcomes.
- CT is definitive but diagnosis can be made with ultrasound and radiography.
- Ongoing focus includes refining diagnostic accuracy, managing intra‑operative challenges, and optimizing prognosis across different long bones affected by similar lesions.
Disclaimer: The article represents the opinion of individual authors exclusively and not necessarily the opinion of AO or its clinical specialties.
The physeal spike complex
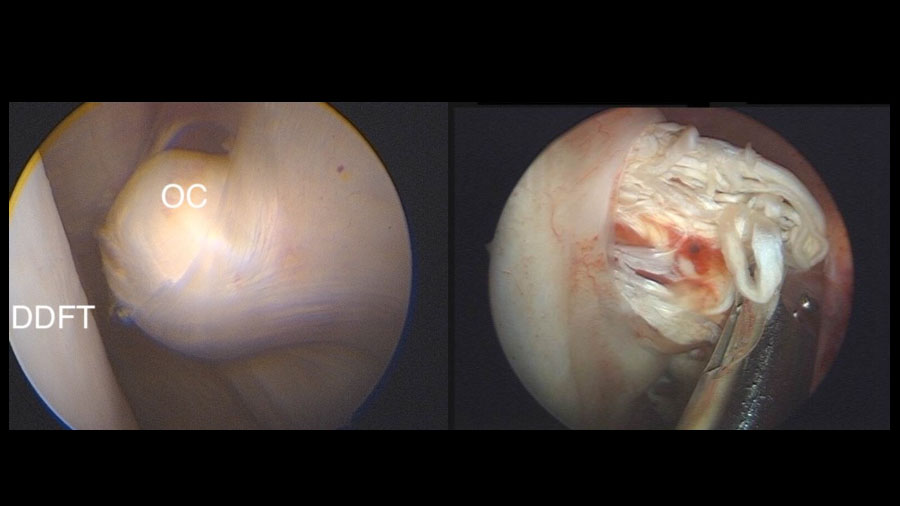
Osteochondromata and exostoses arising from the caudal physeal region, often referred to as “spikes”, most commonly occur at the distal radius, with the tibia and the third metacarpal or metatarsal bones involved less frequently. Their clinical significance lies not only in their presence but in their relationship to the deep digital flexor tendon (DDFT) as it glides across the caudal aspect of the distal limb. Even seemingly small protrusions can cause considerable tendon irritation or tearing, particularly during high‑speed work, when flexion–extension cycles are rapid and forceful.
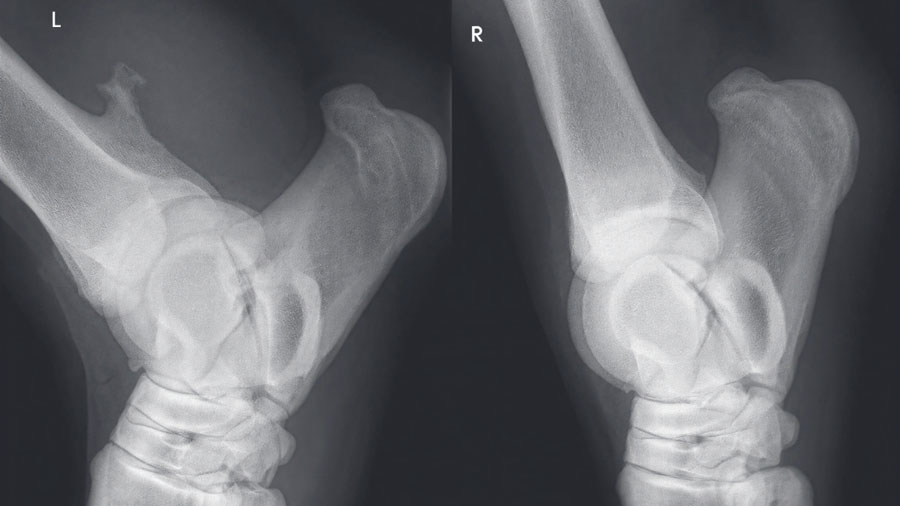
Two distinct categories exist, with osteochondroma usually much larger and presenting distinctly more proximal to the physis, compared to the much smaller physeal spikes which usually occur at the level of the distal radial physeal scar. This positional difference affects how the lesions appear on imaging but does not affect the damage to the overlying tendon. Perhaps the most important difference is that osteochondroma usually affect one leg whereas physeal spikes are invariably bilateral.
Clinical presentation and pathophysiology
Lameness in affected horses is usually attributed to three interrelated mechanisms:
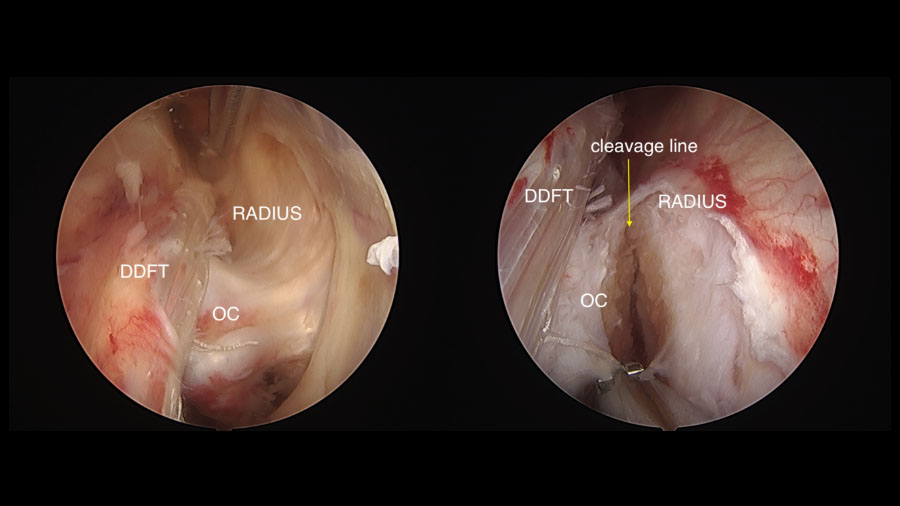
- Direct tendon trauma, often manifesting as linear tears on the dorsal surface of the DDFT as it moves across the spike
- Inflammatory response generated when torn tendon fibers are exposed within the tendon sheath, causing secondary tenosynovitis and synovial distension
- In acute cases, intra-synovial haemorrhage (haemosynovium) and subsequent distension can cause severe lameness.
In practice it is most likely all three that contribute to lameness, and all three need addressing to adequately treat the condition.
Clinically, horses often present with acute lameness following high‑speed exercise, accompanied by marked effusion within the carpal sheath. Aseptic synoviocentesis commonly yields sanguineous synovial fluid due to hemorrhage from the torn DDFT. If frank blood is obtained, surgery should be delayed to allow further diagnostics and importantly haemostasis, as continued bleeding within the sheath significantly increases surgical difficulty and risks.
Meanwhile, haemosynovium of the carpal sheath can result from a number of conditions including accessory carpal bone fracture, capsular tearing, rupture of the radial head of the DDFT and the above-mentioned laceration of the DDFT by a bony spike.
Imaging challenges and diagnostic pitfalls
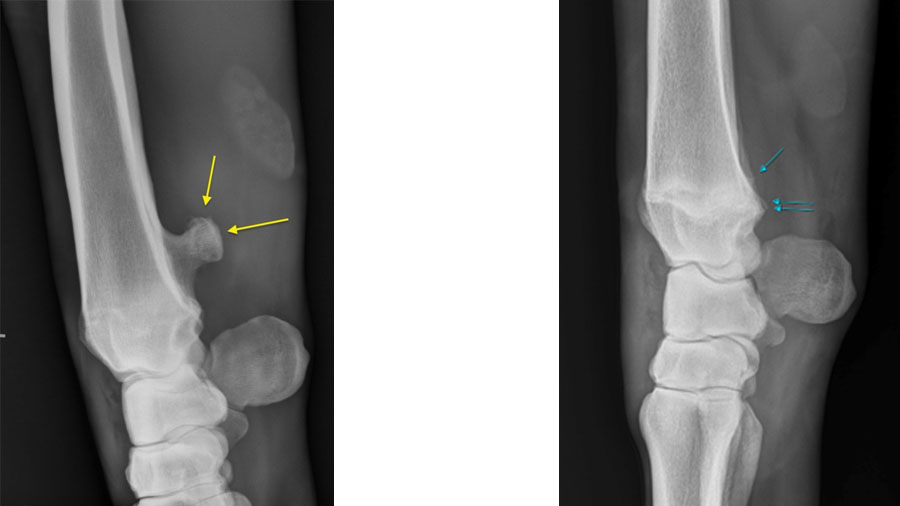
Radiography and ultrasonography are often used for primary investigation but can be easily misinterpreted.
Due to the concave aspect of the caudal radius at the level of the distal physis, axial spikes can be hidden by the more prominent medial and lateral extent of the physis, making them difficult to appreciate on standard projections. Equally, the medial and lateral physeal “scars” can be misinterpreted as spikes.
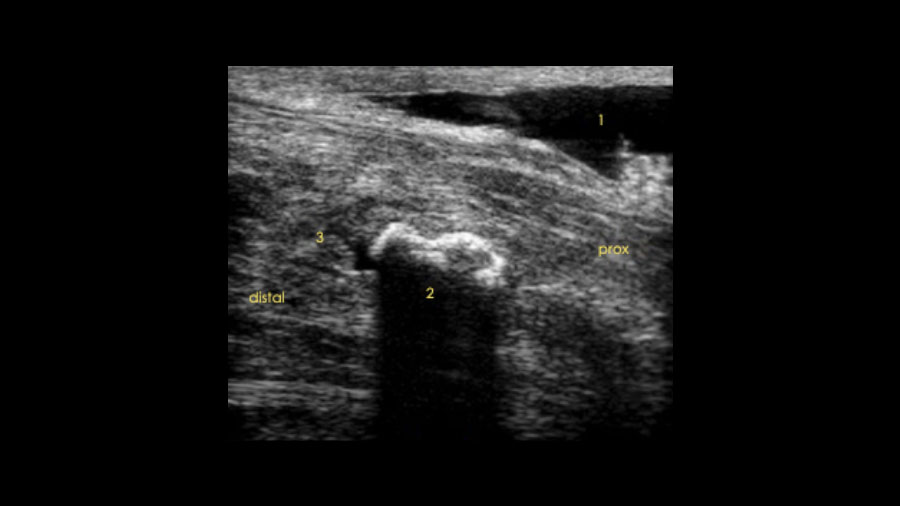
Ultrasound
Ultrasound can be useful to document the position of the spike and its location relevant to the DDFT, with more medial and lateral bony protuberances causing no impingement on tendons as they pass over the caudal radius. Trauma to the dorsal aspect of the DDFT in the presence of a spike is definitive.
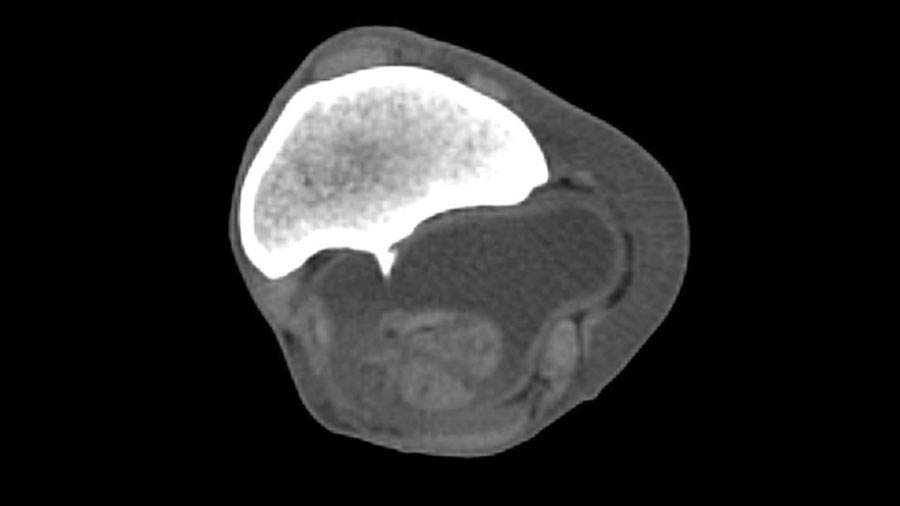
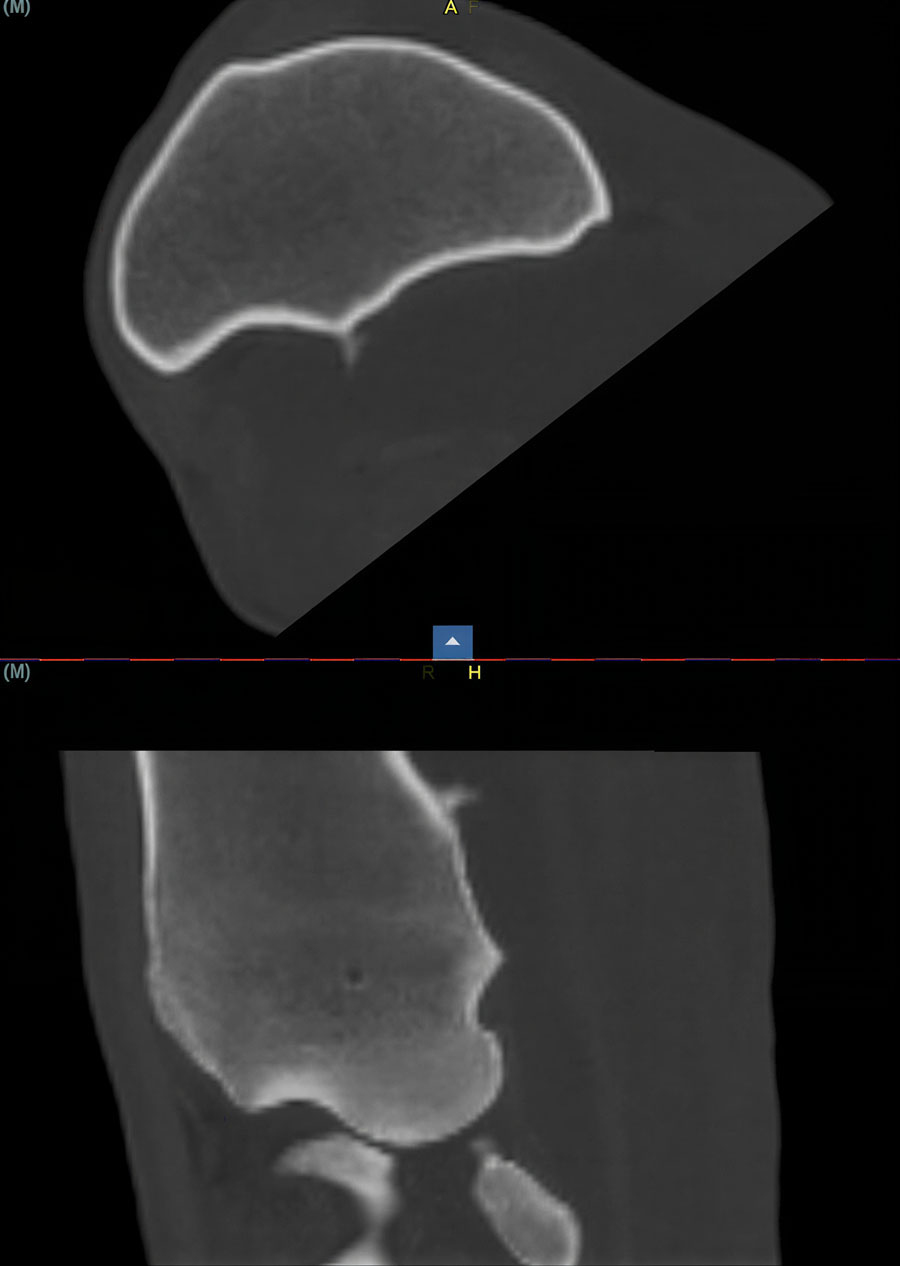
Computed tomography
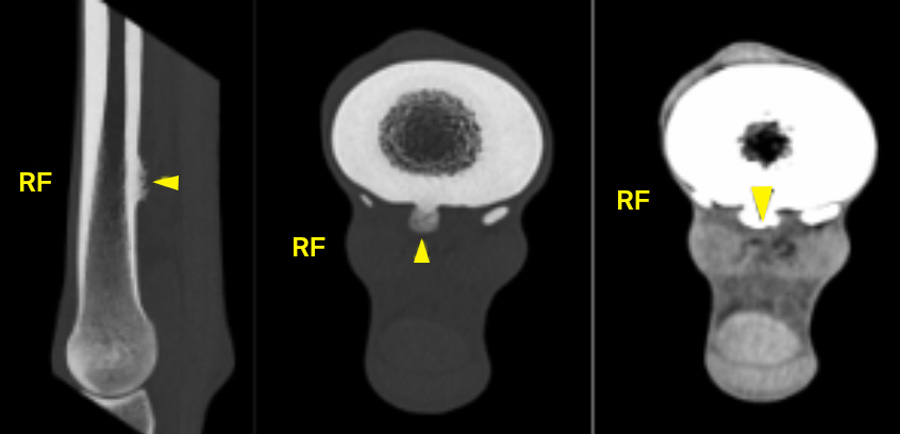
Computed tomography (CT) provides the greatest diagnostic accuracy. CT reconstruction clearly demonstrates the position of the spike, the presence of synovial effusion, and any associated tendon damage. Flexed, non‑weightbearing images may allow tears in the epitenon to open when not under tension, while seeing the spike protruding into the body of the DDFT on a weightbearing image is diagnostic.
In many cases, CT also helps clarify the extent of tendon involvement, especially when conventional imaging has been inconclusive.
If available, CT with intra-thecal contrast, will provide the most accurate diagnostic information, helping guide surgical planning as well as predicting prognosis in the presence of concurrent injury to the region.
Surgical management
Treatment involves both removing the bony protrusion to prevent impingement on the tendon and simultaneous debridement of the tendon lesion to prevent ongoing tenosynovitis and persistent lameness.
Extrapolating from DDFT linear tears (a common cause of lameness seen in the digital flexor tendon sheath of horses) and carpal sheath effusion resulting from tears of the radial head of the DDFT (unrelated to spike trauma) we know that damaged tendon fibres prolapsed from a linear tear must be removed and the defect debrided in order to resolve lameness.
The preferred technique with these cases is minimally invasive surgery (tenoscopy) to remove the bony spike and debride the torn tendon fibrils, at the same time allowing assessment of the contents of the carpal sheath. Reports suggest a higher incidence of post-operative infection with carpal sheath surgery compared to other synovial structures, so an open approach is best avoided if possible.
However, tenoscopic removal is not without challenges.
Intra‑operative considerations
Haemorrhage is the arthroscopist’s worst nightmare, reducing visibility and making completion of surgery challenging. Both removal of the impinging bone spike and debridement of the tendon lesion result in bleeding.
To combat this, horses are operated in dorsal recumbency and ingress fluid pressure is increased, watching for extravasation of fluid via the portal which itself can limit instrument access.
Unfortunately, the use of a tourniquet often restricts tendon movement and reduces access in the carpal sheath, so these are not routinely used.
Technique overview
A standard lateral tenoscopic approach is made to the carpal sheath and an incision is made in the thickened synovium overlying the base of the bony spike. An osteotome is then seated parallel to the caudal radius and a mallet used to section the osteochondroma or spike in a lateral to medial direction. The bone is usually left attached by medial soft tissues and can be safely removed with rongeurs.
If large it can be sectioned using a mechanical burr or left in situ to be removed after tendon debridement via an enlarged portal. Enlarging a portal prior to completing tendon debridement with an oscillating mechanical resector results in loss of fluid pressure, extensive bleeding and an inability to complete the procedure.
The DDFT tear (and any damage to SDFT or RH-DDFT) is debrided with the resector and the sheath lavaged before routine skin closure and bandaging.
Postoperative care and prognosis
Affected horses are maintained in a bandage until aseptic suture removal at 10–14 days, followed by restricted activity for approximately four weeks. Most horses return to training at three months, with a good prognosis for racing. This is in contrast to the six months rest usually given for DFTS linear tears post-operatively, which have a much more guarded prognosis for return to work.
Representative clinical case
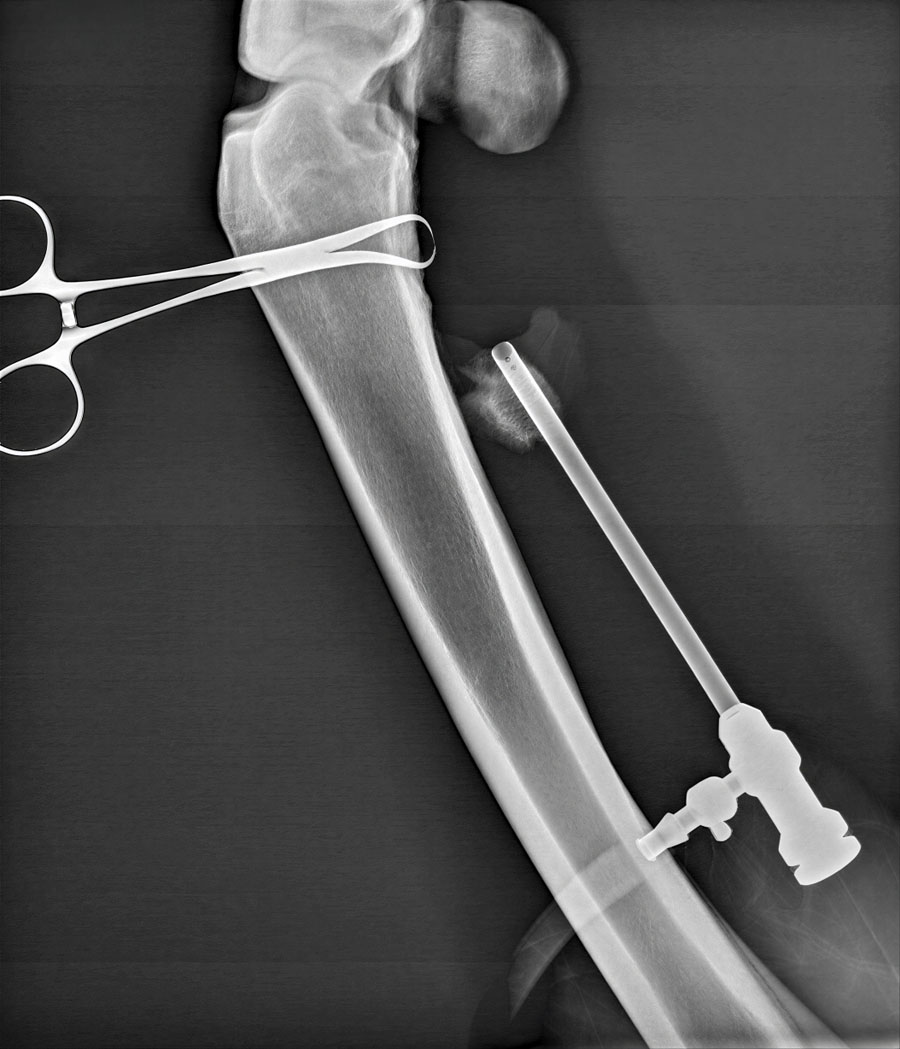
A recent case involved a 3‑year‑old Thoroughbred gelding with acute lameness and carpal sheath swelling, having successfully completed multiple races. Radiographs identified a large osteochondroma, and ultrasound confirmed marked disruption to the DDFT. Standard tenoscopic surgery was completed as above, identifying the osteochondroma extending deep into the DDFT. Removal was confirmed using radiography intra-operatively after debridement of the tendon lesion.
Spikes in other long bones
Similar lesions are occasionally seen in the caudal distal physes of other long bones:
Tibial osteochondromata
Although unusual, these are treated with the same principles: accurate imaging, removal of the impinging bone via tenoscopy of the tarsal sheath, and debridement of any soft‑tissue damage. Similar success has been reported.
Distal third metacarpal exostoses
These tend to occur proximal to the joint and digital flexor tendon sheath, impinging instead on the bifurcation of the suspensory ligament. Diagnosis is similar, but treatment is via an open surgical approach with the fetlock slightly flexed to access the spike on the caudal physeal region. As no synovial structure is involved, less debridement is required, though prolapsed fibers should be removed if present. Again, a good prognosis for return to exercise is expected.
The physeal spike complex in practice
Irrespective of the aetiology of the spike and anatomic location, the physeal spike complex presents an interesting diagnostic process, with the chance to combine arthroscopic surgery with hammers and chisels (every orthopod’s dream!) and a rewarding surgical outcome for patient and owner.
About the author:
Barny Fraser, BVSc MSc CertES(Orth) AFHEA DipECVS MRCVS, is an Associate Professor of Equine Surgery at Murdoch University in Western Australia and a Recognised Specialist since 2006 (ECVS, ABVS). He is primarily involved in clinical teaching of lameness and surgery in horses, with special interests in fracture repair and arthroscopic surgery. Research interests include the use of CT for pre-surgical diagnosis and planning as well as investigating longitudinal development of pre-fracture pathology using CT and MRI in young racehorses.
In addition to undergraduate, intern and resident training, his passion for clinical teaching led him to become initially AO VET Faculty and subsequently the Equine Representative on the Asia-Pacific Board of AO VET, where he hopes to help shape the future of post-graduate veterinary surgical education in the region.
You might also be interested in...
Fellowships
The AO VET Fellowship Program provides additional experience in AO techniques for young veterinary surgeons interested in orthopedics and musculoskeletal disorders.
Videos and webinars
Discover the full collection of educational videos with small and large animal practical exercises, recorded webinars and expert presentations by AO VET's world-renowned faculty.
Pastern Arthrodesis
This blog article examines technique selection, ongoing debates, and practical guidance for optimizing outcomes for Pastern Arthrodesis in the horse.