Integrated angular stable locking in the novel Tibia Nail Advanced (TN-A) in combination with low-profile retaining locking screws improves fixation stability in a distal tibia fracture model
Introduction
Unstable distal tibial fractures are challenging injuries requiring surgical treatment. Intramedullary nails are one of the implant options; however, insufficient fixation of the distal fragment may lead to postoperative loss of reduction, delayed healing, malunion, or nonunion. Recently, a novel design for angular stable locking has been developed that maintains the basic principle of intramedullary nailing, ie, relative stability, but introduces improvements expected to reduce nail toggling, screw migration and secondary loss of reduction, without the requirement for additional intraoperative procedures.
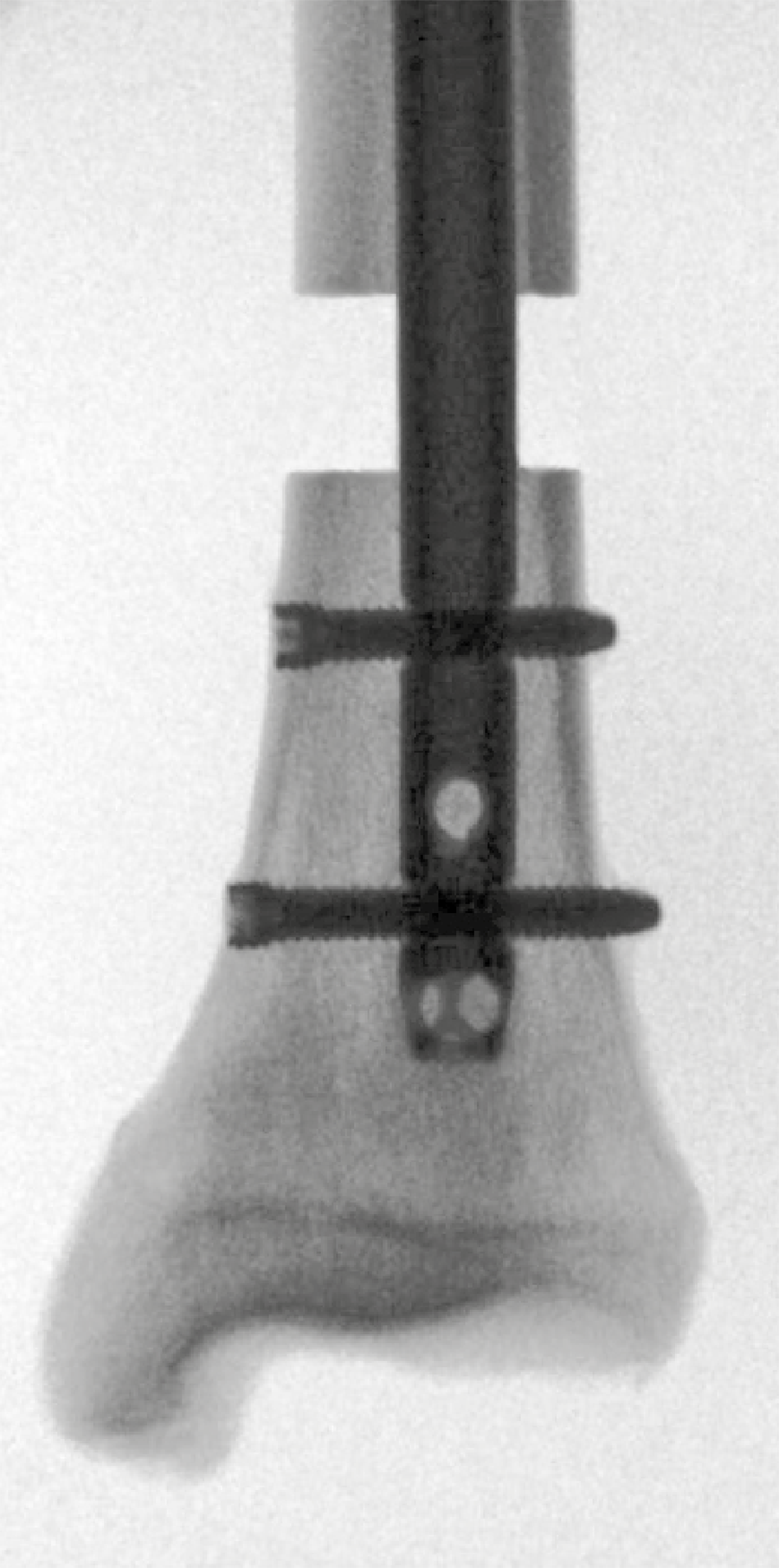
Core TN-A design features are polyether ether ketone (PEEK) inlays integrated in the proximal and distal canal portions of the nail for angular stable screw locking, and low-profile retaining locking screws with enhanced purchase in the near cortex (Fig 1 and Fig 2) (read detailed information about TN-A).
This project aimed to compare the biomechanical competence of the novel angular stable TN-A concept versus the conventional nonangular stable Expert Tibial Nail (ETN) fixation in a human anatomical model of an unstable distal tibial fracture under dynamic loading.
Materials and Methods
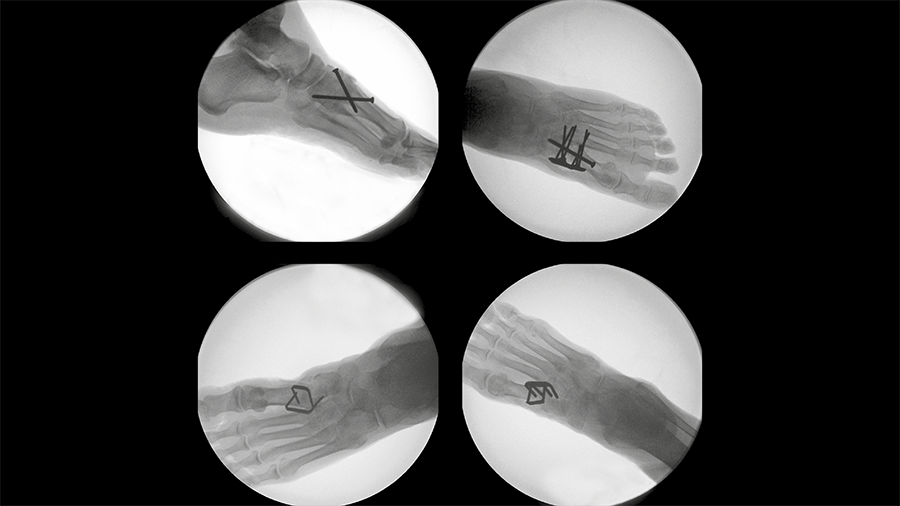
Ten pairs of fresh-frozen human anatomical tibiae with a simulated AO/OTA 42-A3.1 fracture were assigned to two groups for reamed intramedullary nailing using either a nonangular stable ETN with three distal screws or the novel TN-A with two distal angular stable low-profile retaining locking screws (Fig 2). Testing conditions included quasi-static and progressively increasing combined cyclic axial and torsional loading in internal rotation until failure of the bone-implant construct, with monitoring by means of motion tracking (Fig 3).
Results
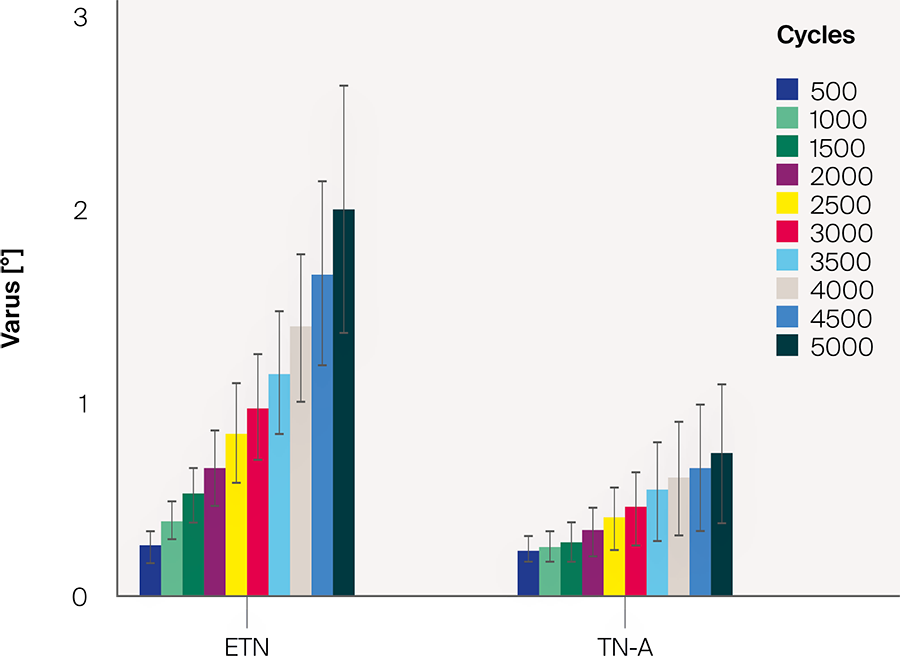
Initial axial construct stiffness did not differ significantly between the two nail systems (P = .29). In contrast, initial torsional construct stiffness was significantly higher for TN-A compared with ETN (P = .04). Initial nail toggling of the distal tibial fragment in varus and flexion was lower for TN-A compared with ETN, being significant in flexion (P = .91 and P = .03). After 5’000 cycles, interfragmentary varus, flexion, internal rotation, axial displacement and shear displacement movements at the fracture site were at least 54% lower on average for TN-A compared with ETN, with flexion and shear displacement being significant (P = .14, P = .04, P = .25, P = .11 and P =.04; Fig 4). Cycles to failure until interfragmentary 5° varus and 5° flexion were at least 16% higher on average for TN-A compared with ETN and were significantly different (P = .04).
Discussion
From a biomechanical perspective, the novel angular stable TN-A concept incorporating two improvements, namely (1) PEEK inlays and (2) low-profile retaining locking screws:
-
Provides increased relative construct stability and maintains it over time while reducing the number of required locking screws without impeding the flexibility of the nail itself
-
Reduces the tilting of the distal fragment in any direction by up to 72%
-
Resists better toward loss of reduction.
You might also be interested in
Combined nail and plate fixation
The treatment of osteoporotic comminuted distal femoral fractures shows a positive response to this new approach.
Peri-implant fractures
Short vs long cephalomedullary nails following pertrochanteric fracture consolidation.
Rib fracture plating comparison
Intrathoracic plate fixation demonstrates significantly higher stiffness versus extrathoracic plating.
Tarsometatarsal joint fusion
Nitinol stables might demonstrate comparable performance to established techniques for fusion of the first TMT joint.