Harnessing modifiable intraoperative factors—what decisions should surgeons make to improve postoperative stability?
Preview
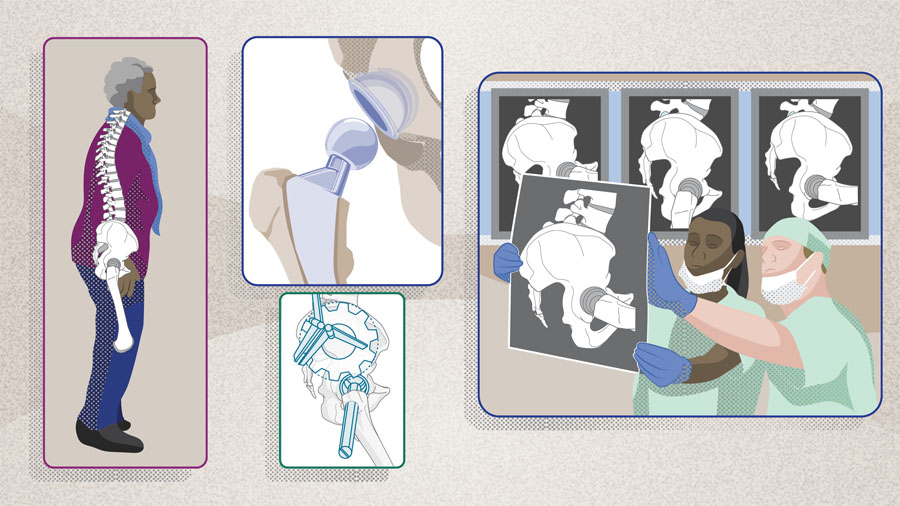
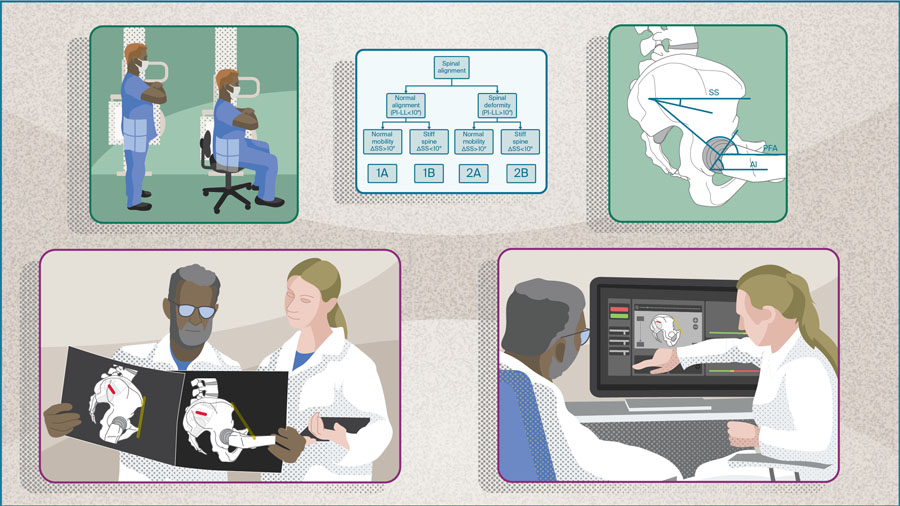
The risk of instability, impingement, and dislocation is multifaceted in total hip arthroplasty (THA). In Part 1 of the series, we discussed the nonmodifiable patient risk factors that come into play, including demographics, THA indications, and associated pathologies like lumbar spine diseases, that may affect the hip-spine relationship. Following the critical consideration of these characteristics, Part 2 of the series guides us through the preoperative planning stage, when spinopelvic parameters should be considered via radiographic imaging of the patient in different positions, ie, standing and sitting, to better template the orientation of the implant.
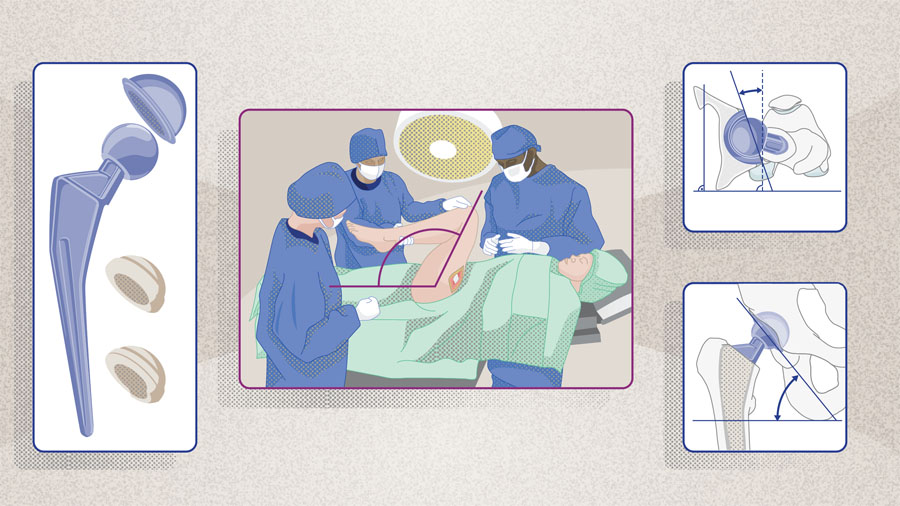
In Part 3 of our three-part series, George Grammatopoulos from The Ottawa Hospital emphasizes the need for a holistic approach encompassing all parameters that may influence clinical outcomes. He is a pioneering advocate in the importance of attention to detail intraoperatively and provides us with his list of key surgical decisions and safety checks to perform during the THA procedure. Understanding the surgical factors that influence clinical safety and performance outcomes, along with the role of spinopelvic parameters, will help heighten surgical acumen and minimize the risk of postoperative instability.

George Grammatopoulos
The Ottawa Hospital, University of Ottawa, Ottawa, Ontario, Canada
An emphasis on the problem—instability remains
In Part 1 and Part 2 of this series on spinopelvic parameters in total hip arthroplasty (THA), we discuss the prevalence and incidence of postoperative instability and how it is still a common complication despite many applied strategies for improvement. Besides the obvious risks of revision surgery due to instability, the postoperative quality of life of the patient can be dramatically influenced by the related complications. Impingement is undoubtedly painful and uncomfortable for the patient, and the constant concern that a dislocation could happen at any time is not easy to manage. Patient-reported outcomes from over 1,000 patients with dislocation were analyzed in a 2022 cross-sectional study in the Danish Hip Arthroplasty Register and matched 1:2 to control patients without dislocation. Applying the established EQ-5D and HOOS patient questionnaires, the study revealed that patients who experienced dislocation consistently reported reduced health and hip-related quality-of-life indicators compared to the controls, even 5 years after the latest dislocation. Twenty percent of the patients with dislocation said they would not undergo the hip replacement surgery again compared to only 7% of controls [1]. This is too high a degree of dissatisfaction and lack of confidence in THA from patients who sustained a dislocation.
Another recent 2022 analysis from the UK Clinical Practice Research Datalink database had similar findings on the quality of life and burden of THA dislocation, with the EQ-5D and Oxford Hip Scores reported as being worse in patients with dislocation. Additionally, the economic burden was shown to be immense. Dislocation led to increased healthcare costs and use of resources, with patients often requiring multiple surgeries. Direct medical costs at 2 years were around 150% higher for patients with dislocation, and these costs increased to around 450% for patients with multiple closed reductions and a revision surgery [2]. Collectively these studies underscore the long-term impact of dislocation on patient well-being, as well as the never-ending balance in maintaining excellence in patient care while decreasing economic burden.
Read the full article with your AO login
- Highlighting the remaining instability
- Improved disclocation rates?
- Intraoperative strategies during THA surgery
- Towards anterior approach adoption
- Patient-specific spinopelvic evaluation
- Bearing size impact on dislocation rate
- Hip reconstruction and trial liners use
- Big data and future technology
- Conclusions
AO Recon resources
Contributing experts

George Grammatopoulos
The Ottawa Hospital, University of Ottawa, Ottawa, Ontario, Canada

Nathanael D Heckmann
Keck Medical Centre, University of Southern California, Los Angeles, California, United States

Jonathan M Vigdorchik
Hospital for Special Surgery, New York, New York, United States
This article was written by Greta Thompson-Steckel, AO Innovation Translation Center, Clinical Evidence, Switzerland.
References
-
Hermansen LL, Viberg B, Overgaard S. Patient-reported outcome after dislocation of primary total hip arthroplasties: a cross-sectional study derived from the Danish Hip Arthroplasty Register. Acta Orthop. 2022 Jan 3;93:29-36.
-
Galvain T, Mantel J, Kakade O, et al. Treatment patterns and clinical and economic burden of hip dislocation following primary total hip arthroplasty in England. Bone Joint J. 2022 Jul;104-B(7):811-819.
-
van Erp JHJ, Husken MFT, Filipe MD, et al. Did the dislocation risk after primary total hip arthroplasty decrease over time? A meta-analysis across six decades. Arch Orthop Trauma Surg. 2023 Jul;143(7):4491-4500.
-
Haynes JA, Hopper RH, Jr., Ho H, et al. Direct Anterior Approach for Primary Total Hip Arthroplasty Lowers the Risk of Dislocation Compared to the Posterior Approach: A Single Institution Experience. J Arthroplasty. 2022 Mar;37(3):495-500.
-
Christensen TH, Egol A, Pope C, et al. How Does Surgical Approach Affect Characteristics of Dislocation After Primary Total Hip Arthroplasty? J Arthroplasty. 2023 Jul;38(7 Suppl 2):S300-S305.
-
Grammatopoulos G, Innmann M, Phan P, et al. Spinopelvic challenges in primary total hip arthroplasty. EFORT Open Rev. 2023 May 9;8(5):298-312.
-
Kahn TL, Kellam PJ, Anderson LA, et al. Can Dislocation Rates Be Decreased Using the Anterior Approach in Patients With Lumbar Spondylosis or Lumbar Instrumented Fusion? J Arthroplasty. 2021 Jan;36(1):217-221.
-
Vigdorchik JM, Sharma AK, Madurawe CS, et al. Does Prosthetic or Bony Impingement Occur More Often in Total Hip Arthroplasty: A Dynamic Preoperative Analysis. J Arthroplasty. 2020 Sep;35(9):2501-2506.
-
Sharma AK, Cizmic Z, Dennis DA, et al. Low dislocation rates with the use of patient specific "Safe zones" in total hip arthroplasty. J Orthop. 2021 Sep-Oct;27:41-48.
-
Vigdorchik JM, Sharma AK, Buckland AJ, et al. 2021 Otto Aufranc Award: A simple Hip-Spine Classification for total hip arthroplasty : validation and a large multicentre series. Bone Joint J. 2021 Jul;103-B(7 Supple B):17-24.
-
Verhaegen JCF, Innmann M, Vorimore C, et al. Achieving cup target as per spinopelvic assessment is associated with improved THA outcome: a prospective, multicentre study. Hip Int. 2025 Mar;35(2):130-141.
-
Karasavvidis T, Pagan CA, Sharma AK, et al. Decreased Instability in High-Risk (Hip-Spine 2B) Patients After Modifications of Surgical Planning and Technique. J Arthroplasty. 2024 Sep;39(9S1):S138-S144.
-
Murray DW. The definition and measurement of acetabular orientation. J Bone Joint Surg Br. 1993 Mar;75(2):228-232.
-
Meermans G, Grammatopoulos G, Innmann M, et al. Cup placement in primary total hip arthroplasty: how to get it right without navigation or robotics. EFORT Open Rev. 2022 May 31;7(6):365-374.
-
Beverland DE, O'Neill CK, Rutherford M, et al. Placement of the acetabular component. Bone Joint J. 2016 Jan;98-B(1 Suppl A):37-43.
-
Merle C, Grammatopoulos G, Waldstein W, et al. Comparison of native anatomy with recommended safe component orientation in total hip arthroplasty for primary osteoarthritis. J Bone Joint Surg Am. 2013 Nov 20;95(22):e172
-
Sevick J, Plaskos C, Speirs A, et al. Does Replication of Native Acetabular Anatomy Satisfy Recommended Hip-Spine Targets for Cup Orientation? JB JS Open Access. 2025 Apr-Jun;10(2).
-
Hoskins W, Rainbird S, Holder C, et al. A Comparison of Revision Rates and Dislocation After Primary Total Hip Arthroplasty with 28, 32, and 36-mm Femoral Heads and Different Cup Sizes: An Analysis of 188,591 Primary Total Hip Arthroplasties. J Bone Joint Surg Am. 2022 Aug 17;104(16):1462-1474.
-
Wyatt MC, Whitehouse MR, Kieser DC, et al. Are Lipped Polyethylene Liners Associated with Increased Revision Rates in Patients with Uncemented Acetabular Components? An Observational Cohort Study. Clin Orthop Relat Res. 2020 Mar;478(3):581-589.
-
Hussein Y, Iljazi A, Sorensen MS, et al. The risk of dislocation in dual-mobility versus 36 mm heads in primary total hip arthroplasty for osteoarthritis. Bone Joint J. 2025 Jan 1;107-B(1):50-57.
-
Merle C, Innmann MM, Waldstein W, et al. High Variability of Acetabular Offset in Primary Hip Osteoarthritis Influences Acetabular Reaming-A Computed Tomography-Based Anatomic Study. J Arthroplasty. 2019 Aug;34(8):1808-1814.
-
Heckmann ND, Chung BC, Wier JR, et al. The Effect of Hip Offset and Spinopelvic Abnormalities on the Risk of Dislocation Following Total Hip Arthroplasty. J Arthroplasty. 2022 Jul;37(7S):S546-S551.
-
Konishi T, Hamai S, Kawahara S, et al. Impact of CT-based navigation, large femoral head, and dual-mobility liner on achieving the required range of motion in total hip arthroplasty. Bone Jt Open. 2025 Feb 8;6(2):155-163.
-
Wyles CC, Maradit-Kremers H, Larson DR, et al. Creation of a Total Hip Arthroplasty Patient-Specific Dislocation Risk Calculator. J Bone Joint Surg Am. 2022 Jun 15;104(12):1068-1080.
-
Khosravi B, Rouzrokh P, Maradit Kremers H, et al. Patient-specific Hip Arthroplasty Dislocation Risk Calculator: An Explainable Multimodal Machine Learning-based Approach. Radiol Artif Intell. 2022 Nov;4(6):e220067.