Recognizing the role of preoperative spinopelvic parameter assessment in hip stability
Preview
With the increasing number of patients undergoing total hip arthroplasty (THA) and the significant economic burden associated with revision surgery, improving implant stability has become a major focus in orthopedic surgery. Over the past decade, recognizing the impact of spinopelvic parameters on hip stability has revolutionized our preoperative assessment. As evidenced by recent clinical and biomechanical studies, these strategies can significantly reduce THA dislocation rates.
In Part 2 of our three-part series, Jonathan M Vigdorchik from the Hospital for Special Surgery in New York, United States, guides us through the latest advances in spinopelvic biomechanics. Together, we explore how these findings are reshaping our understanding of hip arthroplasty and why a personalized preoperative strategy is essential to optimize patient outcomes.

Jonathan M Vigdorchik
Hospital for Special Surgery, New York, New York, United States
Beyond the Lewinnek “safe zone”: the importance of spinometric parameters in optimizing THA stability
Total hip arthroplasty (THA) is one of the most successful procedures in orthopedic and trauma surgery [1]. However, despite advances in surgical techniques and implants, postoperative complications remain a challenge for both patients and surgeons. Dislocation is currently the leading cause of revision surgery in the United States, with rates ranging from 0.2% to 10% [2, 3].
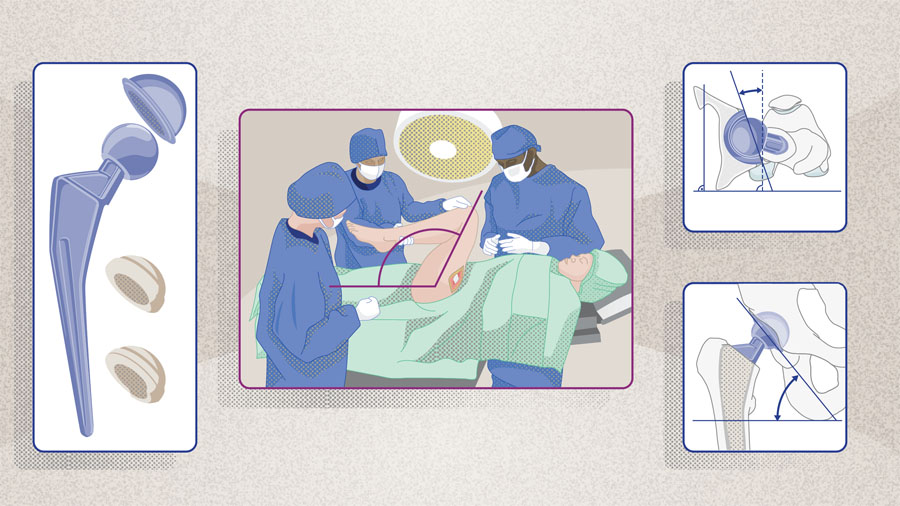
Although the incidence of dislocation has decreased, the number of primary THA patients is increasing and may account for an overall increase in postoperative instability. It is estimated that revision THA cases will rise between 78–182% between 2014 and 2030, potentially reaching up to 572,000 cases annually in the United States by 2040 [4]. Acetabular cup orientation is a key factor in THA success, with suboptimal positioning being a major contributor to dislocation. In a review of 380 revision THAs, Novikov et al [5] found that 51% were potentially preventable, with nearly half of these linked to suboptimal acetabular component positioning.
To minimize the risk of dislocation after primary THA, Lewinnek et al [6] proposed a “safe zone” for acetabular cup orientation of 40° ± 10° inclination and 15° ± 10° anteversion. These guidelines became widely adopted; however, numerous authors have challenged the validity of the Lewinnek safe zone as a universal standard for component orientation. Studies have shown that up to 60% of dislocations occur despite cup orientations falling within the radiographic inclination/anteversion boundaries described by Lewinnek [7–9]. So why do acetabular cups that appear to be within the safe zone still dislocate? Clearly, additional factors are at play.
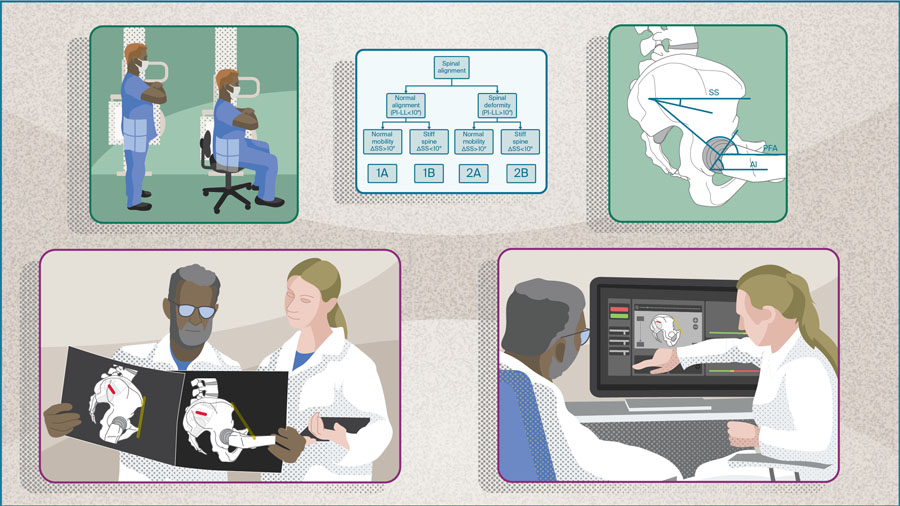
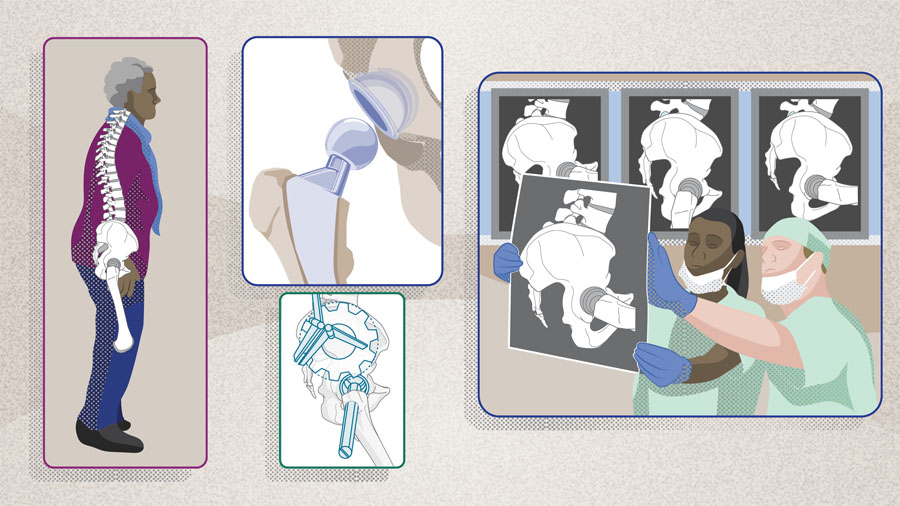
Hip arthroplasty surgeons are increasingly recognizing the dynamic interplay between the hip, spine, and pelvis and its impact on prosthesis stability, wear, and overall function. It is now well established that these structures move in coordination, with the orientation of the acetabulum shifting between positions such as standing and sitting. Patients with concomitant hip and spinopelvic pathology experience higher rates of postoperative complications [10–12]. For instance, DelSole et al [13], in a study evaluating 139 THAs in 107 patients with spinal deformity, found that this cohort had a dislocation rate of 8%, compared to just 1.5% in the control group.
Vigdorchik notes, “recognizing the interplay between the hip and spine is essential for improving clinical assessment, surgical planning, and postoperative outcomes. The current body of work addresses this oversight by highlighting the influence of spinopelvic alignment on hip stability and the need for a more personalized preoperative approach. We now understand that certain patients are at higher risk of complications, but by adjusting the surgical plan, we can reduce that risk; therefore, we need to identify those at-risk patients and tailor the surgical approach to decrease that risk”.
Read the full article with your AO login
- Preoperative spinopelvic assessment matters
- Beyond Lewinnek’s “safe zone”
- Spinopelvic parameter standardization
- Hip-Spine Classification
- Preoperative functional imaging
- Confirming clinical outcomes
- Conclusion
AO Recon resources
Contributing experts

George Grammatopoulos
The Ottawa Hospital, University of Ottawa, Ottawa, Ontario, Canada

Nathanael D Heckmann
Keck Medical Centre, University of Southern California, Los Angeles, California, United States

Jonathan M Vigdorchik
Hospital for Special Surgery, New York, New York, United States
This article was written by Chiara Cianciolo, AO Innovation Translation Center, Clinical Evidence, Switzerland.
References
-
Learmonth ID, Young C, Rorabeck C. The operation of the century: total hip replacement. The Lancet. 2007;370(9597):1508–1519.
-
Gwam CU, Mistry JB, Mohamed NS, et al. Current Epidemiology of Revision Total Hip Arthroplasty in the United States: National Inpatient Sample 2009 to 2013. J Arthroplasty. 2017 Jul;32(7):2088–2092.
-
Bozic KJ, Kurtz SM, Lau E, et al. The Epidemiology of Revision Total Hip Arthroplasty in the United States. JBJS. 2009;91(1):128–133.
-
Bains SS, Dubin JA, Salib CG, et al. The Epidemiology of the Revision Total Hip Arthroplasty in the United States From 2016 to 2022. Arthroplast Today. 2024 Oct 29:30:101517.
-
Novikov D, Mercuri JJ, Schwarzkopf R, et al. Can some early revision total hip arthroplasties be avoided? Bone Joint J. 2019 Jun;101-b(6_Supple_B):97–103.
-
Lewinnek GE, Lewis JL, Tarr R, et al. Dislocations after total hip-replacement arthroplasties. J Bone Joint Surg Am. 1978 Mar;60(2):217–220.
-
Esposito CI, Gladnick BP, Lee YY, et al. Cup position alone does not predict risk of dislocation after hip arthroplasty. J Arthroplasty. 2015 Jan;30(1):109–113.
-
Abdel MP, von Roth P, Jennings MT, et al. What Safe Zone? The Vast Majority of Dislocated THAs Are Within the Lewinnek Safe Zone for Acetabular Component Position. Clin Orthop Relat Res. 2016 Feb;474(2):386–391.
-
Dorr LD, Callaghan JJ. Death of the Lewinnek "Safe Zone". J Arthroplasty. 2019;34(1):1–2.
-
Vigdorchik JM, Sharma AK, Buckland AJ, et al. 2021 Otto Aufranc Award: A simple Hip-Spine Classification for total hip arthroplasty : validation and a large multicentre series. Bone Joint J. 2021 Jul;103-b(7 Supple B):17–24.
-
Sharma AK, Vigdorchik JM. The Hip-Spine Relationship in Total Hip Arthroplasty: How to Execute the Plan. J Arthroplasty. 2021 Jul;36(7s):S111–s120.
-
Luthringer TA, Vigdorchik JM. A Preoperative Workup of a "Hip-Spine" Total Hip Arthroplasty Patient: A Simplified Approach to a Complex Problem. J Arthroplasty. 2019 Jul;34(7s):S57–s70.
-
DelSole EM, Vigdorchik JM, Schwarzkopf R, et al. Total Hip Arthroplasty in the Spinal Deformity Population: Does Degree of Sagittal Deformity Affect Rates of Safe Zone Placement, Instability, or Revision? J Arthroplasty. 2017 Jun;32(6):1910–1917.
-
Vigdorchik J, Eftekhary N, Elbuluk A, et al. Evaluation of the spine is critical in the workup of recurrent instability after total hip arthroplasty. Bone Joint J. 2019 Jul;101-b(7):817–823.
-
Legaye J, Duval-Beaupère G, Hecquet J, Marty C. Pelvic incidence: a fundamental pelvic parameter for three-dimensional regulation of spinal sagittal curves. Eur Spine J. 1998;7(2):99–103.
-
Zagra L, Benazzo F, Dallari D, et al. Current concepts in hip–spine relationships: making them practical for total hip arthroplasty. EFORT Open Reviews. 2022 11 Jan. 2022;7(1):59–69.
-
Au J, Perriman DM, Neeman TM, Smith PN. Standing or Supine X-Rays after Total Hip Replacement – When is the Safe Zone Not Safe? HIP International. 2014;24(6):616–623.
-
Shon WY, Gupta S, Biswal S, et al. Validation of a simple radiographic method to determine variations in pelvic and acetabular cup sagittal plane alignment after total hip arthroplasty. Skeletal Radiol. 2008 Dec;37(12):1119–1127.
-
Ala Eddine T, Migaud H, Chantelot C, et al. Variations of pelvic anteversion in the lying and standing positions analysis of 24 control subjects and implications for CT measurement of position of a prosthetic cup. Surg Radiol Anat. 2001; 23(2):105–110.
-
Pierrepont J, Hawdon G, Miles BP, et al. Variation in functional pelvic tilt in patients undergoing total hip arthroplasty. Bone Joint J. 2017;99-B(2):184–191.
-
Sharma AK, Grammatopoulos G, Pierrepont JW, et al. Sacral Slope Change From Standing to Relaxed-Seated Grossly Overpredicts the Presence of a Stiff Spine. J Arthroplasty. 2023 Apr;38(4):713–718.e711.
-
Behery OA, Vasquez-Montes D, Cizmic Z, et al. Can Flexed-Seated and Single-Leg Standing Radiographs Be Useful in Preoperative Evaluation of Lumbar Mobility in Total Hip Arthroplasty? J Arthroplasty. 2020 Aug;35(8):2124–2130.
-
Pour AE, Green JH, Christensen TH, et al. Is It Necessary to Obtain Lateral Pelvic Radiographs in Flexed Seated Position for Preoperative Total Hip Arthroplasty Planning? Arthroplast Today. 2023 May 17:21:101133.
-
Karasavvidis T, Pagan CA, Sharma AK, et al. Decreased Instability in High-Risk (Hip-Spine 2B) Patients After Modifications of Surgical Planning and Technique. J Arthroplasty. 2024 Sep;39(9s1):S138–s144.
-
Ramkumar PN, Pang M, Vigdorchik JM, et al. Patient-Specific Safe Zones for Acetabular Component Positioning in Total Hip Arthroplasty: Mathematically Accounting for Spinopelvic Biomechanics. J Arthroplasty. 2023 Sep;38(9):1779–1786.
-
Novikov D, Mercuri JJ, Schwarzkopf R, et al. Can some early revision total hip arthroplasties be avoided? Bone Joint J. 2019 Jun;101-B(6_Supple_B):97–103.
-
Abdel MP, Carender CN, Berry DJ. Practice Norms in Primary Hip and Knee Arthroplasty: What is Everyone Else Doing? J Arthroplasty. 2025 Apr 10:SO883–5403(25)00340-7.