Robotic-assisted total knee arthroplasty: a game changer in alignment strategies
Preview
Although the ideal alignment philosophy in the settings of total knee arthroplasty (TKA) is still debatable today, the value of an accurately positioned implant in the clinical outcome of joint reconstruction is undeniable. Thus, it is not surprising that the use of robots in the operating room is rising worldwide [1]. Through the dynamic intraoperative assessment of joint gaps and ligaments, robotic-assisted surgery platforms enable the surgeon to execute accurate bony cuts while preserving the soft-tissue envelope [2, 3]. Despite the high costs associated with robotic-assisted TKA (raTKA) [3], this technique is gaining popularity among the surgeons, especially those aiming to restore the most "normal" knee kinematics in a patient [4]. In this article, Sébastien Lustig, Professor in the Arthritis and Joint Replacement Department of Lyon North University Hospital, reviews the promises and limitations offered by raTKA for functional alignment.

Sébastien Lustig
Lyon North University Hospital
Lyon, France
Robotic-assisted total knee arthroplasty: the advent of semiactive and fully active systems
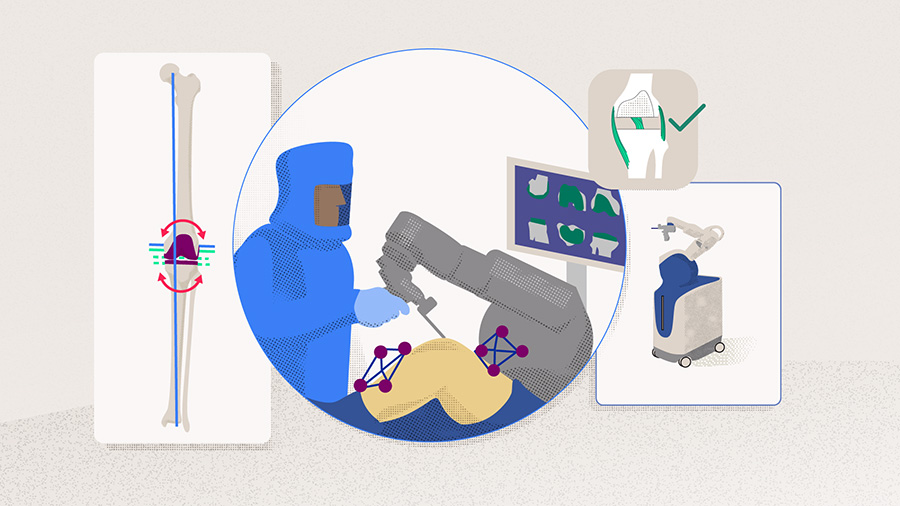
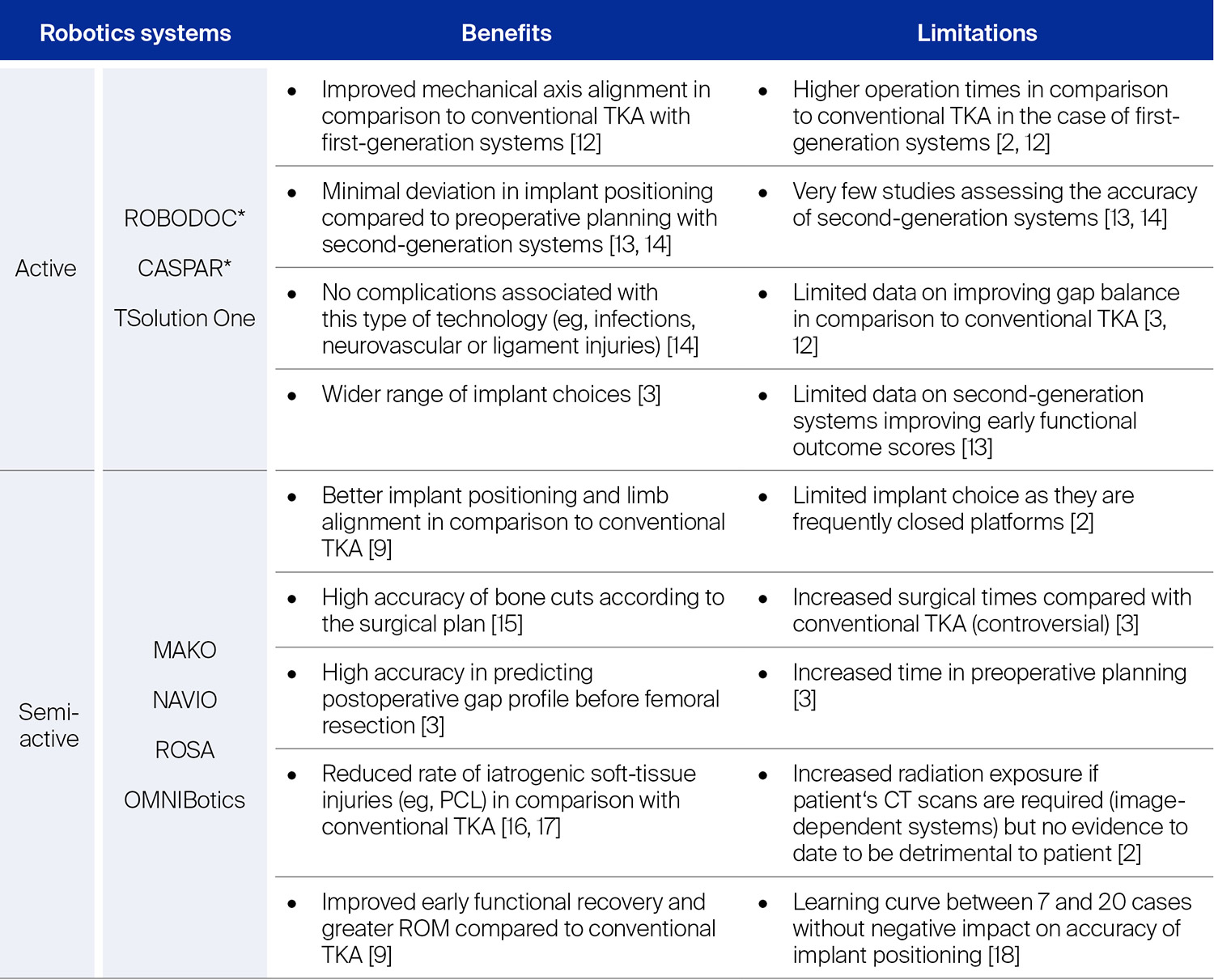
The term "robot" was initially coined in 1920 by the Czech science-fiction writer Karel Capek, who described artificially humanoids repeatedly performing labor tasks [2]. In the operating room, robots were initially designed to minimize human error while maximizing operative accuracy [3]. Since the first reported robotic-assisted total knee arthroplasty (raTKA) in the early 2000s [5], the surgical tasks performed by robotic-assisted surgery platforms have rapidly evolved. Currently, all robotic technologies use dynamic referencing to assess intraoperative knee stability, alignment, and range of motion (ROM) while adjusting bone resection, ligament balance, and position of the prothesis [2, 6]. Based on how bone resections are conducted, robotic-assisted surgery platforms can be either classified as "fully active" (ie, a robotic arm performs autonomously preprogrammed bone resections on the patient) or "semiactive" (ie, the surgeon performs bone resection within a predefined zone that has been set in the preoperative plan while receiving intraoperative feedback) [1, 3, 7]. Such systems normally include a haptic interface by which the surgeon receives information about the forces and stress exerted on articular surfaces and can adjust his/her movements intraoperatively. Preoperative computed tomography (CT) scans or magnetic resonance imaging (MRI) enables the surgeon to generate a virtual three-dimensional (3D) model of the patient-specific bony anatomy. The 3D virtual model is employed to preplan bone cuts, implant size, as well as positioning, and is subsequently mapped intraoperatively to the patient's bone anatomy using navigational trackers, in a process known as registration [8, 9]. Another type of semiactive systems are handheld robotic burrs, which are manually controlled by the surgeon. Instead of a haptic interface, the robot follows the navigation field's burring tool trajectory, controlling the speed and exposure of the device to protect against iatrogenic ligament injuries [3, 10]. Contrary to haptic systems, this type of semiactive system is imageless (ie, it is not based on CT/MRI scans) and compatible with a wide range of prosthetic implants and brands [2, 10, 11]. Each robotic device is associated with several benefits and limitations (Table 1). While semiactive systems are the most frequently used today, the appearance of second-generation fully active systems might change the orthopedic landscape in the near future.
Read the full article with your AO login
- Clinical and functional outcomes of robotic-assisted TKA
- Is raTKA a cost-effective technique?
- Robotic-assisted TKA and functional alignment philosophy: an intertwined road
- Personalized preoperative planning
- Registration, ligament balancing, and bone resection
- The promising clinical outcomes of functionally aligned total knee arthroplasty
- Conclusions and future perspectives
Additional AO resources
Access videos, tools, and other assets.
- Videos
- Upcoming events: AO Recon Course finder
Contributing experts
This series of articles was created with the support of the following specialists (in alphabetical order):

Michel Bonnin
Centre Orthopédique Santy
Lyon, France

Sébastien Lustig
Lyon North University Hospital
Lyon, France

Charles Rivière
Clinique du Sport Bordeaux-Mérignac
Mérignac, France
This issue was written by Antia Rodriguez-Villalon and Laura Kehoe, AO Innovation Translation Center, Clinical Science, Switzerland.
References
- Shah SM. After 25 years of computer-navigated total knee arthroplasty, where do we stand today? Arthroplasty. 2021 Nov 4;3(1):41.
- Saber AY, Marappa-Ganeshan R, Mabrouk A. Robotic Assisted Total Knee Arthroplasty. Treasure Island (FL): StatPearls Publishing; 2022.
- St Mart JP, Goh EL. The current state of robotics in total knee arthroplasty. EFORT Open Rev. 2021 Apr;6(4):270–279.
- Shatrov J, Battelier C, Sappey-Marinier E, et al. Functional Alignment Philosophy in Total Knee Arthroplasty - Rationale and technique for the varus morphotype using a CT based robotic platform and individualized planning. Sicot j. 2022;8:11.
- Jakopec M, Harris SJ, Rodriguez y Baena F, et al. The first clinical application of a "hands-on" robotic knee surgery system. Comput Aided Surg. 2001;6(6):329–339.
- Siebert W, Mai S, Kober R, et al. Technique and first clinical results of robot-assisted total knee replacement. Knee. 2002 Sep;9(3):173–180.
- Sultan AA, Piuzzi N, Khlopas A, et al. Utilization of robotic-arm assisted total knee arthroplasty for soft tissue protection. Expert Rev Med Devices. 2017 Dec;14(12):925–927.
- La Palombara PF, Fadda M, Martelli S, et al. Minimally invasive 3D data registration in computer and robot assisted total knee arthroplasty. Med Biol Eng Comput. 1997 Nov;35(6):600–610.
- Batailler C, Fernandez A, Swan J, et al. MAKO CT-based robotic arm-assisted system is a reliable procedure for total knee arthroplasty: a systematic review. Knee Surg Sports Traumatol Arthrosc. 2021 Nov;29(11):3585–3598.
- Casper M, Mitra R, Khare R, et al. Accuracy assessment of a novel image-free handheld robot for Total Knee Arthroplasty in a cadaveric study. Comput Assist Surg (Abingdon). 2018 Dec;23(1):14–20.
- van der List JP, Chawla H, Joskowicz L, et al. Current state of computer navigation and robotics in unicompartmental and total knee arthroplasty: a systematic review with meta-analysis. Knee Surg Sports Traumatol Arthrosc. 2016 Nov;24(11):3482–3495.
- Song EK, Seon JK, Yim JH, et al. Robotic-assisted TKA reduces postoperative alignment outliers and improves gap balance compared to conventional TKA. Clin Orthop Relat Res. 2013 Jan;471(1):118–126.
- Sicat CS, Chow JC, Kaper B, et al. Component placement accuracy in two generations of handheld robotics-assisted knee arthroplasty. Arch Orthop Trauma Surg. 2021 Dec;141(12):2059–2067.
- A. BO, B. S, S. K, et al. COMPONENT POSITION ACCURACY IN ACTIVE ROBOTIC TOTAL KNEE ARTHROPLASTY. Orthopaedic Proceedings. 2018;100-B(SUPP_12):24–24.
- Sires JD, Craik JD, Wilson CJ. Accuracy of Bone Resection in MAKO Total Knee Robotic-Assisted Surgery. J Knee Surg. 2021 Jun;34(7):745–748.
- Kayani B, Konan S, Pietrzak JRT, et al. Iatrogenic Bone and Soft Tissue Trauma in Robotic-Arm Assisted Total Knee Arthroplasty Compared With Conventional Jig-Based Total Knee Arthroplasty: A Prospective Cohort Study and Validation of a New Classification System. J Arthroplasty. 2018 Aug;33(8):2496–2501.
- Hampp EL, Sodhi N, Scholl L, et al. Less iatrogenic soft-tissue damage utilizing robotic-assisted total knee arthroplasty when compared with a manual approach: A blinded assessment. Bone Joint Res. 2019 Oct;8(10):495–501.
- Kayani B, Konan S, Huq SS, et al. Robotic-arm assisted total knee arthroplasty has a learning curve of seven cases for integration into the surgical workflow but no learning curve effect for accuracy of implant positioning. Knee Surg Sports Traumatol Arthrosc. 2019 Apr;27(4):1132–1141.
- Agarwal N, To K, McDonnell S, et al. Clinical and Radiological Outcomes in Robotic-Assisted Total Knee Arthroplasty: A Systematic Review and Meta-Analysis. J Arthroplasty. 2020 Nov;35(11):3393-3409.e3392.
- Chin BZ, Tan SSH, Chua KCX, et al. Robot-Assisted versus Conventional Total and Unicompartmental Knee Arthroplasty: A Meta-analysis of Radiological and Functional Outcomes. J Knee Surg. 2021 Aug;34(10):1064–1075.
- Lustig S, Sappey-Marinier E, Fary C, et al. Personalized alignment in total knee arthroplasty: current concepts. Sicot j. 2021;7:19.
- Kayani B, Konan S, Tahmassebi J, et al. Robotic-arm assisted total knee arthroplasty is associated with improved early functional recovery and reduced time to hospital discharge compared with conventional jig-based total knee arthroplasty: a prospective cohort study. Bone Joint J. 2018 Jul;100-b(7):930–937.
- Bhimani SJ, Bhimani R, Smith A, et al. Robotic-assisted total knee arthroplasty demonstrates decreased postoperative pain and opioid usage compared to conventional total knee arthroplasty. Bone Jt Open. 2020 Feb;1(2):8–12.
- Marchand RC, Sodhi N, Anis HK, et al. One-Year Patient Outcomes for Robotic-Arm-Assisted versus Manual Total Knee Arthroplasty. J Knee Surg. 2019 Nov;32(11):1063–1068.
- Zhang J, Ndou WS, Ng N, et al. Robotic-arm assisted total knee arthroplasty is associated with improved accuracy and patient reported outcomes: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc. 2022 Aug;30(8):2677–2695.
- Chen KK, Kim KY, Vigdorchik JM, et al. Cost-Effectiveness Analysis of Robotic Arthroplasty. In: Lonner JH, eds. Robotics in Knee and Hip Arthroplasty: Current Concepts, Techniques and Emerging Uses. Cham: Springer International Publishing; 2019. 67–74.
- Pierce J, Needham K, Adams C, et al. Robotic arm-assisted knee surgery: an economic analysis. Am J Manag Care. 2020 Jul 1;26(7):e205–e210.
- O'Callaghan WB, Gouk C, Wilkinson MPR, et al. Computer-Aided Surgery-Navigated, Functional Alignment Total Knee Arthroplasty: A Surgical Technique. Arthroplast Today. 2022 Apr;14:121–127.
- MacDessi SJ, Griffiths-Jones W, Harris IA, et al. Coronal Plane Alignment of the Knee (CPAK) classification. Bone Joint J. 2021 Feb;103-b(2):329–337.
- Kayani B, Konan S, Tahmassebi J, et al. A prospective double-blinded randomised control trial comparing robotic arm-assisted functionally aligned total knee arthroplasty versus robotic arm-assisted mechanically aligned total knee arthroplasty. Trials. 2020 Feb 18;21(1):194.
- Shatrov J, Coulin B, Batailler C, et al. Alignment philosophy influences trochlea recreation in total knee arthroplasty: a comparative study using image-based robotic technology. Int Orthop. 2022 Sep 16.
- Clark GW, Esposito CI, Wood D. Individualized Functional Knee Alignment in Total Knee Arthroplasty: A Robotic-assisted Technique. Techniques in Orthopaedics. 2022;37(3):185–191.