Same-calendar-day discharge after hip and knee arthroplasty
Hot topic snapshot
Over the last decade there has been increasing institutional and societal pressure for cost savings and efficiency in both total knee arthroplasty (TKA) and total hip arthroplasty (THA). In the USA, the Centers for Medicare and Medicaid Services (CMS) removed TKA from the Inpatient-Only (IPO) List in 2018 and THA in 2020. Combined with cost containment, advancements in medical technology, arthroplasty techniques, and anesthesia and pain protocols, surgeons—particularly in the US—increasingly offer same-calendar-day discharge (SCDD) arthroplasty to select patients. A generalized reduction in length of stay has, however, been observed across multiple geographic regions, though regional differences remain.
Multiple studies have demonstrated the feasibility, safety, and efficacy of TKA and THA in the outpatient setting [1]. The benefits of same-day hip or knee arthroplasty include a lower risk of hospital-acquired infection, quicker return to normal activities, and a more comfortable recovery at home; good candidates include those patients who are motivated, in good general health, and who have a good support team at home. These efforts have led to the rise of ambulatory arthroplasty allowing carefully selected patients to be safely discharged on the day of surgery. Not only is SCDD THA or TKA safe, and affording similar outcomes to inpatient THA or TKA, it also potentially provides significant cost savings. The impetus of reducing healthcare costs has been an additional catalyst for this “paradigm shift” towards ambulatory arthroplasty.
In this article, we discuss the evolving trend toward same-calendar-day discharge with a pioneer in this field, Young-Min Kwon, and take a closer look at how this can be applied in other regions with Seung-Jae Lim.
Meet the experts

Young-Min Kwon
Harvard Medical School, Boston, USA
Young-Min Kwon MD, PhD is Professor of Orthopedic Surgery at Harvard Medical School and the Vice Chairman of the department of orthopedic surgery at Massachusetts General Hospital in Boston. Kwon is the director of the bioengineering laboratory. He is board-certified in orthopedic surgery by the American Board of Orthopaedic Surgery (ABOS), the Royal College of Surgeons of England (FRCS), and the Royal Australasian College of Surgeons (FRACS). He is a fellow of the American College of Surgeons (FACS) and the American Orthopaedic Association (AOA). He is an active member of The Hip Society and The Knee Society.

Seung-Jae Lim
Samsung Medical Center, South Korea
Seung-Jae Lim is a Professor of Orthopaedic Surgery at the Samsung Medical Center in Seoul, Korea. He has published more than 120 peer-reviewed papers, and his work has received more than 3,200 citations. He is a board member of the Arthroplasty Society in Asia, the Korean Hip Society, the Korean Fracture Society, and the Korean Society for Computer-Assisted Orthopaedic Surgery. He is also a member of the editorial board of the Journal of Arthroplasty and reviewer for several international orthopedic journals.
In the field
Over the past 30 years, the average length of stay for, specifically, THA has decreased dramatically from 2 weeks to a couple of days. This has been achieved through a combination of innovations in patient education and perioperative care pathways, surgical and anesthetic techniques, blood conservation, multimodal pain management, and accelerated recovery pathways. When questioning how we can perform SCDD after THA or TKA, it is crucial to understand that the outpatient program has to contain essential elements, as described in the American Association of Hip and Knee Surgeons (AAHKS) and American Academy of Orthopaedic Surgeons (AAOS) joint position statement (for further reading, see the AAHKS Position Statement on Outpatient Joint Replacement in 2024 [1] and Karam et al [2]). When considering patients, such an outpatient program must involve good patient selection, patient education and expectation management, and good social support. From the side of the healthcare center, evidence-based pathways and protocols for anesthesia and pain management [2], blood conservation, wound management, mobilization, and venous thromboembolism prophylaxis should be in place. The clinical and surgical team’s expertise and experience is crucial, as Kwon states, “Having everyone in the team being on the same page helps to achieve the optimal outcome”. The health facility environment needs to be conducive to optimizing surgical outcomes, and finally postdischarge communication needs to be considered and followed through.
Looking more closely at which patients to choose, Kwon notes that this is one of the biggest factors to consider. Patient selection requires thorough medical screening in conjunction with medical specialists when needed. Any medical comorbidities and modifiable risk factors should be optimized before surgery. Nevertheless, outpatient arthroplasty is contraindicated in some patients. This includes patients who have poor balance or cognitive impairment, as well as those who have major depression and generalized anxiety disorder, which are known to be independent risk factors for complications. Further, patients who lack a strong social support network are contraindicated. One tool to aid in patient selection is the Outpatient Arthroplasty Risks Assessment (OARA), which can be used to determine who can undergo SCDD. This tool stratifies the patients by nine comorbidity areas to generate a risk category. It has a positive predictive value (PPV) of 81.6% versus 56.4% from the American Society of Anesthesiologists Physical Status (ASA-PS) classification and 70.3% from the Charlson Comorbidity Index (CCI) scores alone. When patients have a low OARA score, ie, < 59, they are twice as likely to be discharged ‘early’. Furthermore, patients who were discharged home within 24 hours were more likely to be young, male, with an ASA score of < 2 and a body mass index (BMI) of < 40. Indeed, lower BMI and patients who had fewer allergies were predicted to be discharged the same day [3]. When selecting patients, it is important to identify risk factors such as congestive heart failure, chronic obstructive pulmonary disease, coronary artery disease, or cirrhosis, given that most major medical complications occur more than 24 hours postoperatively.
Kwon and Lim stress the importance of patient education. When considering transitioning to SCDD or aiming to shorten length of stay, one question that may arise is “what should we tell patients?”. Often inpatient joint replacement uses hospital staff and resources for patient optimization. However, successful SCDD programs will likely involve building and maintaining this infrastructure through an Ambulatory Surgery Center (ASC) or surgeon’s practice. Patient education for optimizing THA and TKA requires advice or an in-home visit to convey the ideal home environment for a safe recovery. Further, digital platforms for patient education, such as videos, websites, or apps, may be beneficial. Finally, it is important to communicate appropriate expectations regarding anticipated pain, mobility, and safety.
Key stats and trends
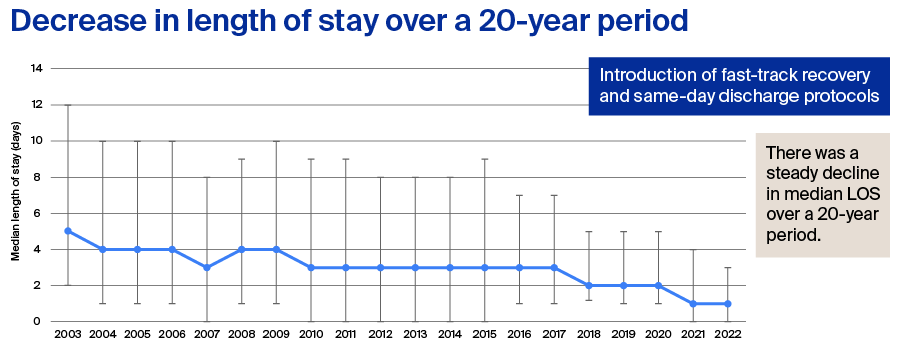
In general, length of stay for THA or TKA has been decreasing. A downward trend in length of stay for THA and TKA over 20 years (from 2003 to 2022) has been previously documented [4, 5]. Interestingly, the trend to a shorter length of stay had gained momentum also outside of the US [4], even before the US-specific 2018 removal of TKA from the Medicare IPO list and the global COVID-19 pandemic (Figure 1).
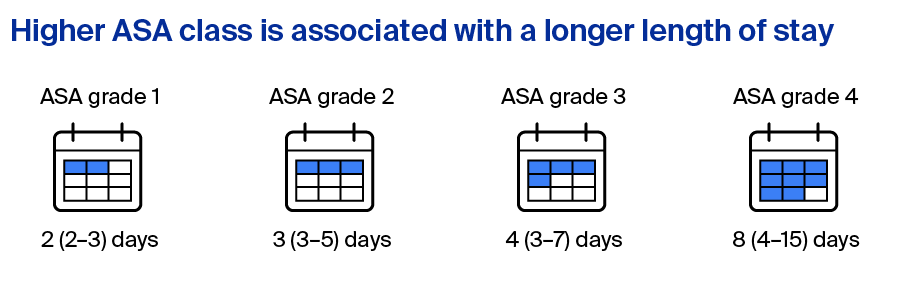
In one Canadian study, Sheridan et al [4] assessed risk factors for length of stay, identifying ASA class to be one of the main predictors of length of stay. In their study, for each increase in ASA class a stepwise increase in length of stay was shown (Figure 2) [4].
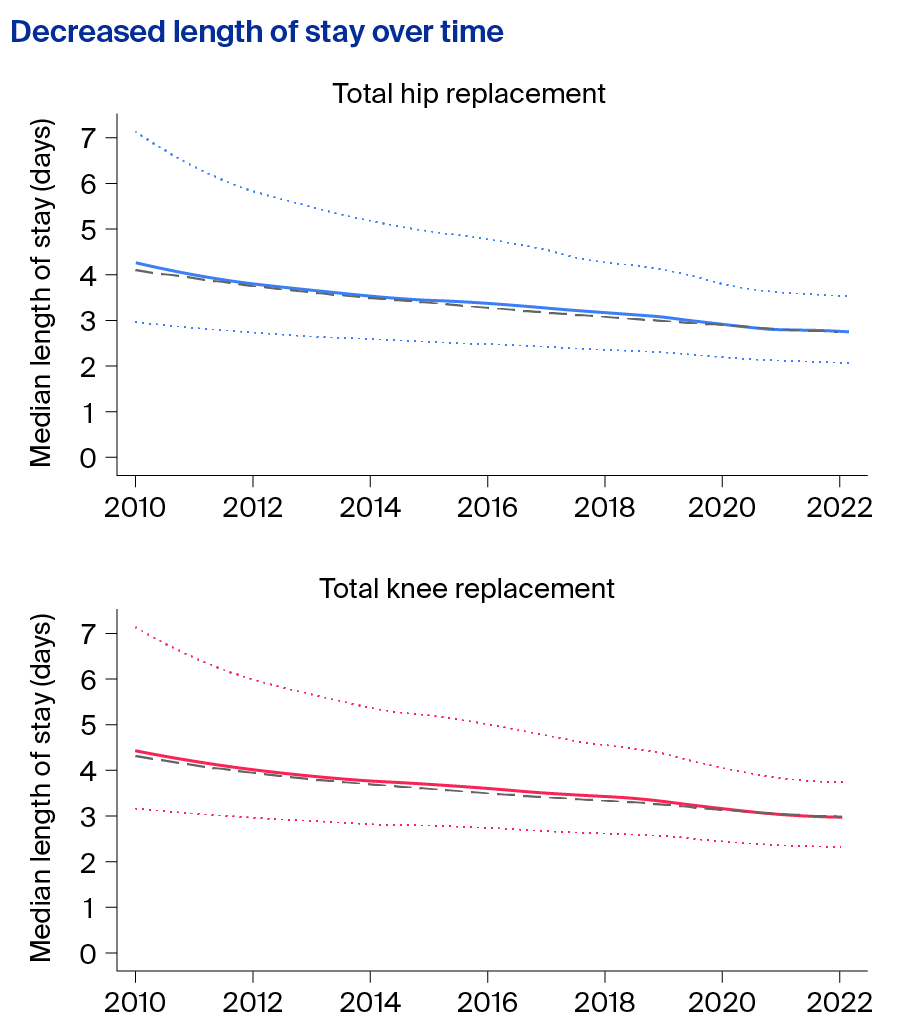
In the UK, length of stay has steadily decreased with the implementation of enhanced recovery protocols (Figure 3).
Certain risk factors for increased length of stay have been identified [3]. The ASA risk class 3 and 4 have been identified to be independent risk factors for readmission or complications together with increased age (> 80 years), smoking, or bleeding diatheses [3]. As noted before, patient selection for SCDD after THA or TKA is crucial. The only tool available to correctly assess patients suitable for same-day discharge is OARA. When compared to the CCI or ASA-PS, OARA has a positive predictive value (PPV) of 81.6% for same-day or next-day discharge, compared with 70.3% for the CCI score and 56.4% for the ASA-PS [3].
Within the United States, Richardson et al [6] observed a dramatic rise in the number of same-day TKA and THA procedures following removal of these surgeries from the Medicare IPO list, as well as during the COVID-19 pandemic. Using the Nationwide Ambulatory Surgery Sample and the National Inpatient sample from 2016 to 2020, they found an increase in the proportion of same-day TKA from 1.2% to 62.4% and same-day THA from 2.0% to 54.5% [6]. By the end of 2020, more than half of all the procedures were performed as same-day surgeries [6].
Similarly in Canada, Gleicher et al [7] reported on the major impact of the COVID-19 pandemic on the available inpatient resources at one local hospital, leading to a surgical backlog. As a response, they transitioned to outpatient arthroplasty through establishing an evidence-based, patient-centered outpatient pathway, including well-defined outpatient selection criteria, anesthetic modifications to allow for early ambulation, education materials aimed at outpatient recovery, and virtual postoperative follow-up [7]. The outpatient pathway was well-appreciated by patients, and by January 2021, more than 25% of patients primarily referred for total joint arthroplasty underwent surgery on an outpatient basis [7].
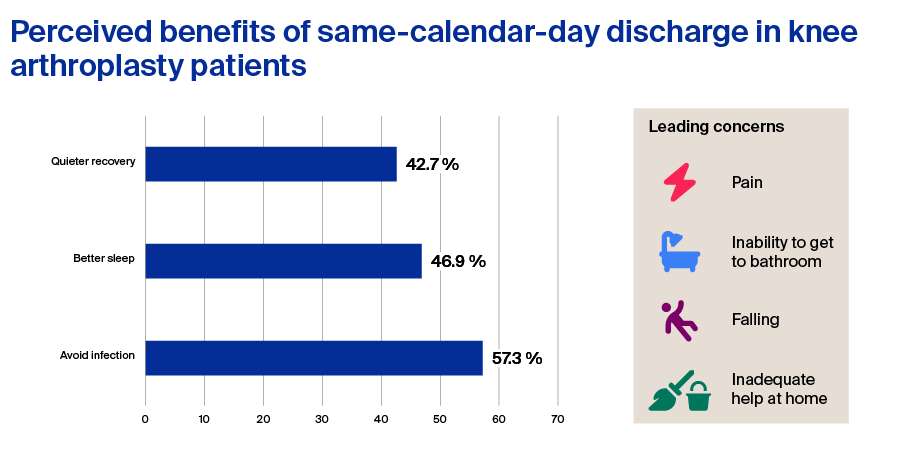
Although these statistics show dramatic increases in outpatient TKA and TKH, they do not provide any insights into the patients’ perspectives. One study by Adelani and Barrack (as cited in Scully et al [3]) surveyed 346 TKA patients, where few patients (3.2%) underwent outpatient TKA. When questioned about their perceptions, most patients felt that they would not have been able to have undergone surgery as an outpatient, whereas only 4.9% thought that they definitely would have been able to go home the same day. The patients reported perceived benefits to include avoiding infection, getting better sleep, and having a quieter recovery, but they were concerned about pain, not being able to get to the bathroom, falling, or not having enough help at home (see Figure 4).
For places where outpatient arthroplasty is established, for example in the US with the use of ASCs for such procedures, the essential elements of an outpatient program may already be in place or are currently being established or improved. But what does it take to become successful, to reduce length of stay, and to try to achieve SCDD?
The upcoming section features Kwon and Lim as they examine various methods, address key challenges, and share results. Lim also offers his insights on SCDD within the Asian context.
Research focus
As discussed earlier, optimizing anesthesia protocols and pain management is crucial for successful SCDD after THA or TKA, since same-day discharge requires the patient to be able to walk independently. We asked Kwon, “What is the role of the analgesia protocol?”, and he explained his established pain management and anesthesia protocols.
To start with, patient education has a high priority. Patients need to be educated in spinal and regional anesthesia techniques. They need to be aware of the level of expected postoperative pain, swelling and mobility, and particular techniques available for the management of pain. Kwon explained that there are multimodal protocols of pain management available. Firstly is “neuraxial anesthesia”, which has demonstrated lower rates of superficial infection, transfusion, thromboembolic and cardiac events, and decreased length of stay. When combined with regional or periarticular anesthesia, neuraxial anesthesia can lower immediate postoperative pain scores and short-term complications. It is, however, important to modulate the effects of neuraxial anesthesia to avoid delays in mobilization and discharge. In this sense, “short-acting” spinal anesthetics, eg, isobaric ropivacaine, bupivacaine, or mepivacaine, with no additives or narcotics, can be used. Secondly is “regional anesthesia”, which has been shown to reduce opioid consumption and need for deep sedation. This is advantageous as it limits nausea, urinary retention, and respiration depression. Both femoral and sciatic blocks, however, should be avoided, as patients cannot rapidly mobilize and have an increased fall risk. Instead, an adductor canal block can be used. This does not affect the quadriceps, allowing for better motor function with early physical activity. Thirdly is “periarticular injection”, which is an effective and more targeted approach to pain management. Periarticular injection avoids motor blockade and minimizes the risk of nerve damage. It also reduces cost and logistical issues associated with regional blocks. A periarticular injection is a “cocktail” of local anesthetic with opioid, ketorolac, epinephrine, or clonidine, and is given as numerous small injections into the pericapsular tissues. This targeted approach has been associated with significant reductions in postoperative pain and opioid consumption. Kwon also noted that over the years they have optimized the pain management and anesthesia protocol so that it has become standard for all patients, be it those aiming for same-day discharge or otherwise.
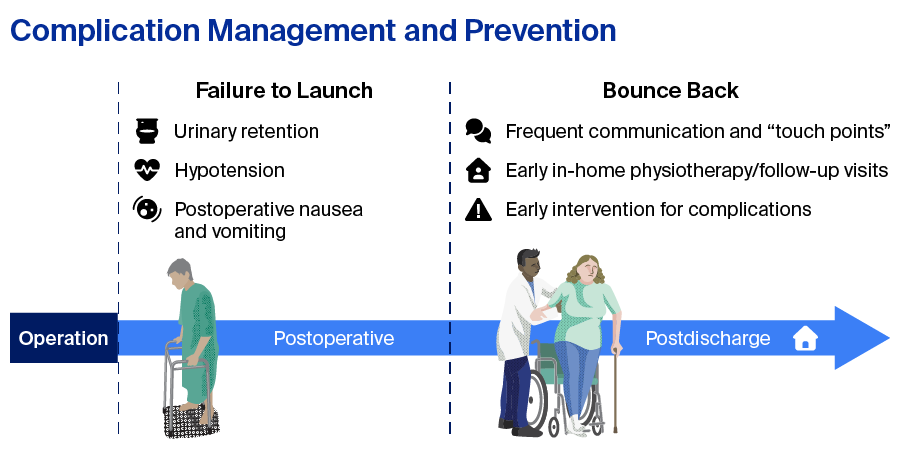
With regard SCDD following THA or TKA, one of the biggest questions raised is, “Does it always work?”. To address this, we must take a closer look at complication management and prevention. Kwon explained the concept of “Failure to Launch”, which includes the immediate postoperative complications that could happen (Figure 5). Postoperative urinary retention is one complication that could occur and ranges in frequency from 5% to 70%. However, this mainly affects patients of increasing age, men, those with spinal anesthesia, prostate pathology, intraoperative insertion of indwelling catheter or improper fluid management. In cases where a urinary catheter is needed, the catheter should be discontinued at the end of the procedure and not left in place postoperatively. What is key here is that prevention of urinary retention is linked to optimized postoperative protocols.
Another possible complication is hypotension, which should be anticipated and actively managed. Preventative strategies include limiting sedation and use of narcotics. Furthermore, by avoiding long-acting spinal anesthetics the duration of sympathectomy can be minimized. Patients should also undergo aggressive fluid resuscitation to maintain adequate intravascular volume, but this must be carefully balanced against the risk of postoperative hyponatremia. In addition, the perioperative use of tranexamic acid can be used to limit blood loss, thus helping to mitigate hypotension.
Postoperative nausea and vomiting must also be preempted. One method is by reducing narcotic consumption, which can be managed through the aforementioned pain management protocols. Alternatively, patients can be prophylactically given antiemetics in combination with glucocorticosteroids or given glucocorticosteroids alone, which can be used due to their antiemetic properties. One other option is to consider a transdermal scopolamine patch, which can be applied to prevent nausea and vomiting after anesthesia and surgery.
Kwon also explained the concept of “Bounce back”, this is when patients who initially were stable enough to be discharged the same day experience issues that require them to return back to their healthcare provider. These postdischarge complications can also be preempted and mitigated through careful postdischarge communication plans. In addition to anticipating and managing immediate postoperative complications, frequent postdischarge communication and eliminating barriers to communication are important. Scheduled phone calls or electronic communication, as well as early in-home physiotherapy or follow-up visits have multiple benefits. They maintain “patient touch points”, which improves satisfaction, and they allow for early intervention for complications, which in turn likely reduces readmission and emergency room visits. To achieve this may require workflow changes and additional infrastructure provided by an ASC or a surgeon’s practice. Nevertheless, these elements of postdischarge care should be considered in future studies which analyze cost and effort for the SCDD episode of care.
Another consideration is regarding safety, “Is same-day arthroplasty safe?”. Although same-day arthroplasty has gained traction, concerns about safety and postoperative complications may still be present. Kwon acknowledged that it is difficult to tease out results specifically for SCDD, as there is an inherent selection bias in nearly all published studies. This is because—as previously explained—outpatient joint replacement is reserved primarily for younger and healthier patients. Additionally, retrospective case series and case-control studies are often from high-volume centers where there is significant expertise in outpatient joint replacement. Nevertheless, the overall rate of complications for outpatients is low. This was shown in a retrospective review study on TKAs performed by a single surgeon [8]. In that study, 100 consecutive patients with SCDD were matched to a cohort of 300 patients with inpatient discharge [8]. Propensity-score matching was performed to adjust for baseline differences in preoperative patient demographics and medical comorbidities [8]. They found that patients with same-day discharge had similar clinical outcomes and superior functional outcomes when compared with patients that had a standard inpatient protocol [8]. The difference in scores for patient-reported outcome measures (PROMs) between patients with same-day discharge and those with inpatient discharge decreased from 3 months following TKA to 1 year after surgery [8]. They found that there was no difference in reoperation or readmission rates, or in healthcare provider visits, concluding that “same-day discharge following TKA may be a safe, viable option” in selected patients [8].
Beyond this, a key consideration for the transition to outpatient arthroplasty is “can it be done safely at a surgery center?” In the US, Ambulatory Surgery Centers (ASC) are healthcare facilities designed to accommodate same-day surgical care, including outpatient arthroplasty. A shift to ASCs offers potential benefits at different levels, eg, costs, efficiency, and patient satisfaction. Multiple initial studies have concluded that THA can be safely performed in both ASC and hospital outpatient settings. Kwon stressed that although successful outpatient arthroplasty has been reported in the ASC setting, it is important to place extra emphasis on preoperative planning. One aspect to consider is equipment because storage and sterilization capacity is often limited in ASCs. As such, careful forethought should be given to intraoperative complication management, so that the center is prepared for intraoperative complications such as fractures or contaminated instruments. The center should also have the ability to convert or change implants, should the need arise. Additionally, there should be a particular focus on team training. In the ASC, the teams should be trained so that they are able to handle standard intraoperative complications in a similar manner to a hospital surgical room. A “transfer safety net” should be set up in ASCs to handle perioperative medical complications, with a transfer agreement to a hospital or plan in place for these cases.
Another question that may be asked and which is a major driver for a shift towards SCDD arthroplasty, is, “is it cost saving?” Kwon emphasized that the evaluation of the financial differences between outpatient and inpatient total joint arthroplasty is complicated by multiple factors. There are inherent regional and healthcare system differences, population differences which include payer type and reimbursement rates, as well as individual provider preferences. In addition, the transition toward outpatient arthroplasty highlights the fact that costs and resources that were often embedded or absorbed by the hospital, such as patient education, medical clearance (preoperative assessment), patient navigators or communication platforms, are being shifted to surgeon practices and outpatient facilities, such as ASCs. Nevertheless, the potential economic benefit of outpatient arthroplasty has been repeatedly cited, with the average cost for outpatients being USD 4,000 less than for inpatients. Thus, for eligible patients, there is the potential for significantly reduced costs for arthroplasty in the outpatient setting.
Did you know?
Is outpatient total hip arthroplasty possible in Asia?
As explained, outpatient THA or SCDD THA is possible particularly in the US given the removal of THA (and TKA) from the Medicare IPO list, and the availability of ASCs. The overall trend towards shorter length of stay has gained momentum. Nevertheless, regional differences still exist. For example, in Canada and the United States, typical length of stay for uncomplicated THA is 0–1 days, whereas in Germany it has been reported as 8–10 days [9]. However, the payment per THA in the United States is far higher than that of other countries, despite the stay being shorter [9].
Lim provided us with his experiences in Japan and Asia. He commented that length of stay is much longer in Japan [10, 11] and in other Asian countries. In most Asian countries, it is around 2–5 days for THA rather than outpatient THA. This takes into consideration the public insurance systems, low admission cost, and diverse socioeconomic or cultural differences. However, the longest length of stay in Asia is in Japan. Here, the convalescent rehabilitation system was set up in 2000 to improve mobility and activities of daily living enabling patients to be discharged to home via rehabilitation care [10]. In a study by Kuwakado [10], patients who underwent TKA or THA remained in an acute care hospital for around 18 days, and in a convalescent hospital for an average of around 37 days. Lim noted that in Japan there is a better patient satisfaction rate without an increased infection rate. On the contrary, the best cost-saving model has been shown to be in China, which leverages the use of the National Volume-Based Procurement (NVBP) of implants [12]. In China, after implementation of the NVBP policy, a significant decrease in cost of implants and hospital stay was observed [12].
When asked whether outpatient THA is possible in Asia, Lim said, “Yes, we can do it, but it is not popular yet.” The regional differences in same-day surgery are evident; while the US is at one end of the spectrum, other regions could aim for reduced length of stay rather than “day-zero” discharge. Implementing the practical measures outlined here—including optimized patient selection, clearly defined anesthesia, and pain management protocols, as well as structured postdischarge communication and follow-up—may contribute to a reduction in length of stay.
Conclusion
The adoption of same-day or short-stay pathways necessitates a collaborative shift in culture among surgeons, anesthesiologists, physiotherapists, and nursing staff, and may require several years to become standard practice. As Kwon and Lim conclude, “Our focus is optimization rather than an absolute target of day-zero discharge”.
AO Recon resources
Contributing experts
This article was created with the support of the following specialists (in alphabetical order):

Young-Min Kwon
Harvard Medical School, Boston, USA

Seung-Jae Lim
Samsung Medical Center, South Korea
This article was written by Lyndsey Kostadinov, AO Innovation Translation Center, Clinical Science, Switzerland.
References
- American Association of Hip and Knee Surgeons. Position Statement on Outpatient Joint Replacement. Published 2018; updated 2024. Available at: AAHKS-Outpatient-Position-Statement-2024.pdf. Accessed April 10, 2026.
- Karam JA, Schwenk ES, Parvizi J. An Update on Multimodal Pain Management After Total Joint Arthroplasty. J Bone Joint Surg Am. 2021;103(17):1652–1662.
- Scully RD, Kappa JE, Melvin JS. "Outpatient"-Same-calendar-day Discharge Hip and Knee Arthroplasty. J Am Acad Orthop Surg. 2020;28(20):e900–e909.
- Sheridan GA, Howard LC, Neufeld ME, et al. Factors Associated With Length of Stay for Hip and Knee Arthroplasty: A 20-Year Single-Province Population-Based Analysis of Longitudinal Temporal Trends. Arthroplasty Today. 2023;24:101274.
- French JMR, Deere K, Sayers A, et al. Trends in hip and knee replacement length of stay and patient demographics in England: a population-based study of 1,455,842 primary procedures. BMC Medicine. 2025;23(1):561.
- Richardson MK, Wier J, Liu KC, et al. Same-Day Total Joint Arthroplasty in the United States From 2016 to 2020: The Impact of the Medicare Inpatient Only List and the COVID-19 Pandemic. J Arthroplasty. 2024;39(4):858–863.e852.
- Gleicher Y, Peacock S, Peer M, et al. Transitioning to outpatient arthroplasty during COVID-19: time to pivot. Cmaj. 2021;193(13):E455.
- Klemt C, Cohen-Levy WB, Pattavina MH, et al. The Same Day Discharges following Primary Total Knee Arthroplasty: A Single Surgeon, Propensity Score-Matched Cohort Analysis. J Knee Surg. 2023;36(13):1380–1385.
- Skopec L, Berenson RA, Simon B, et al. Variation in processes of care for total hip arthroplasty across high-income countries. Health Aff Sch. 2024;2(4):qxae043.
- Kuwakado S, Kawaguchi K, Sakugawa A, et al. Factors Affecting the Length of Convalescent Hospital Stay Following Total Hip and Knee Arthroplasty. Prog Rehabil Med. 2021;6:20210033.
- Tokunaga J, Imanaka Y. Influence of length of stay on patient satisfaction with hospital care in Japan. Int J Qual Health Care. 2002;14(6):493–502.
- Fan Y, Xu Q, Jin G, et al. The cost of total hip arthroplasty: compare the hospitalization costs of national centralized procurement and national volume-based procurement. Front Public Health. 2024;12:1383308.