Symphony Occipito-Cervico-Thoracic System
Frank Kandziora
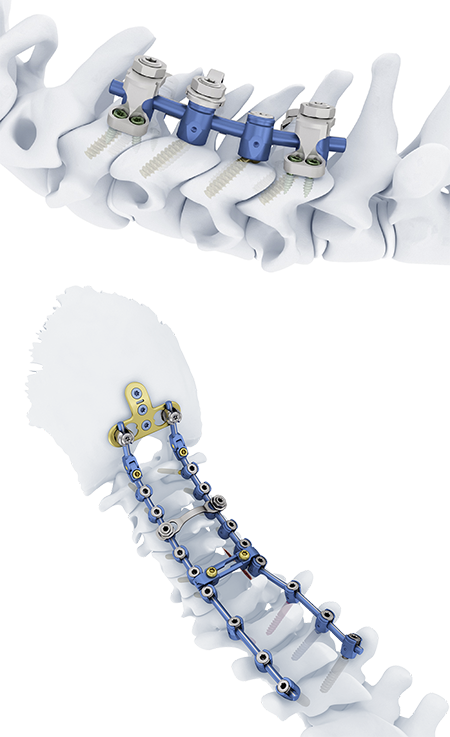
The Symphony Occipito-Cervico-Thoracic System (Fig 1) is an enhanced set of instruments and implants for posterior fixation of the upper (cervico-thoracic) spine. The Symphony System consists of polyaxial screws, 3.5 mm and 4.0 mm rods, compatible hooks, cross connectors, lateral offset connectors, and rod connectors designed for posterior stabilization of the upper spine (Figs 2a-d below). The implants provide the flexibility required to accommodate variations in patient anatomy.
Symphony is intended for use in Posterior Cervical Fusion (PCF) surgery for the treatment of various cervical spine diseases including myelopathy, kyphosis, radiculopathy, deformity cases, and spinal cord injury. Such spine diseases represent a major health concern and are associated with a substantial socioeconomic burden1. Whilst treatment options include fusion and non-fusion procedures, the total number of PCF procedures undertaken annually is increasing [1]. The complexity of patient cases treated with PCF is also higher: there is a growing need for longer constructs extending to the thoracic region and PCF is often paired with anterior fusion surgery. Symphony is designed to reduce the complexity of PCF procedures; to reduce the risk of surgical complications and to improve patient outcomes.
The Symphony system offers a solution for unmet clinical needs in fixation in poor bone quality, deformity correction and revision surgery, whilst retaining the best features of Mountaineer and Synapse.
Fixation
Poor bone quality is an increasing challenge for surgeons [1], as older patients are increasingly meeting the indications for PCF surgery. Screw failure is a common issue (~5.2/patient) in PCF, and patients with poor bone quality are likely to be at greater risk [2,3]. 95% of surgeons have observed lateral-mass screw loosening or pull out [2,3]. The anatomically specific screws and thread forms found within the Symphony system allow for stronger fixation in poor quality bone, and may reduce revisions and complications associated with screw loosening or pull out.
Alignment
In terms of patient outcomes, improvements in regional cervical alignment following deformity correction correlate with an improvement in health-related quality of life (HRQoL) postoperatively [4]. There is a clear need for advanced instrumentation and stronger rods/materials to achieve the desired alignment in the surgical treatment of deformity [4]. Symphony offers stronger and stiffer constructs in the form of 3.5 and 4.0 mm cobalt-chromium rods that are biomechanically superior to titanium equivalents. Furthermore, Symphony offers a single system to cross the cervical-thoracic junction, thereby reducing the complexity of the surgical procedure. Within the Symphony system, screws are available in diameters from 3.5 mm to 5.5 mm, allowing for more stable fixation.
Surgical Revision
The number of posterior cervical revision surgeries undertaken globally is increasing (2%-27% at 41.3 months) [5]. Surgical revisions, specifically the extension of previous posterior cervical constructs, are challenging and can be very invasive for the patient [5]. Use of the Symphony Universal Connectors allows the size of the surgical incision to be significantly reduced. Furthermore, the Universal Connectors accept multiple sizes of rods (3.5 - 6.35 mm) and are able to connect to existing systems. This feature allows existing hardware to be extended rather than removed and replaced, thereby reducing surgical complexity and the duration of the revision procedure. The reduced operating room time offers both improved patient outcomes and economic savings for the hospital system.
Symphony offers a variable and comprehensive set of instrumentation and implants with a sterile packed option. This allows surgeons to handle cases of increasing complexity whilst simplifying instrumentation handling by OR staff and reducing reprocessing costs [6].
Indications
The Symphony System is intended to provide immobilization and stabilization of spinal segments as an adjunct to fusion for acute and chronic instabilities of the cranio-cervical junction, the cervical spine (C1 to C7) and the upper thoracic spine (T1-T3).
Indications include traumatic spinal fractures and/or traumatic dislocations, instability or deformity, failed previous fusions (e.g. pseudarthrosis), tumors involving the cervical/thoracic spine, degenerative disease, including intractable radiculopathy and/or myelopathy, neck and/or arm pain of discogenic origin as confirmed by radiographic studies, and degenerative disease of the facets with instability.
The Symphony System is also intended to restore the integrity of the spinal column even in the absence of fusion for a limited time period in patients with advanced stage tumors involving the cervical spine, in whom life expectancy is of insufficient duration to permit achievement of fusion.
The Symphony System is compatible with occipital fusion components (plates, rods and clamps) from the Synapse Occipital-Cervical-Thoracic System and the Mountaineer Spinal System. Additionally, the Symphony System is compatible with Synapse System hooks and rods.
The Songer Wire/Cable System to be used with the Symphony System allows for wire/cable attachment to the posterior cervical spine.
The Symphony System may be connected to the Expedium Spine System and Viper System using connectors and tapered rods. Symphony can also be linked to the USS Spinal System and Matrix Spine System using connectors and tapered rods.
Contraindications
- Active systemic infection or an infection localized to the site of the proposed implantation.
- Severe osteoporosis may prevent adequate fixation of screws and thus preclude the use of this or any other spinal instrumentation system.
- Patients who have been shown to be safely and predictably treated without internal fixation.
- Open wounds.
Relative Contraindications
Relative contraindications include any entity or condition that totally precludes the possibility of fusion (e.g., kidney dialysis or osteopenia), obesity, certain degenerative diseases, and foreign body sensitivity.
References
- Salzmann SN, Derman PB, Lampe LP, et al. Cervical Spinal Fusion: 16-Year Trends in Epidemiology, Indications, and In-Hospital Outcomes by Surgical Approach. World Neurosurg. 2018;113:e280-e295.
- Coe JD, Vaccaro AR, Dailey AT, et al. Lateral mass screw fixation in the cervical spine: a systematic literature review. J Bone Joint Surg Am. 2013;95(23):2136-2143.
- Olsen Market Research - Cervical Spine. 2018.
- Iyer S, Nemani VM, Nguyen J, et al. Impact of Cervical Sagittal Alignment Parameters on Neck Disability. Spine. 2016;41(5):371-377.
- Koerner JD, Kepler CK, Albert TJ. Revision surgery for failed cervical spine reconstruction: review article. HSS J. 2015;11(1):2-8.
- J. Abrams MD, N. Chutkan. Maximizing operating room efficiency in spine surgery: a process of tray consolidation, instrument standardization and cost savings. In: 2017
Clinical case provided by Frank Kandziora, BG Unfallklinik Frankfurt, Germany.
Patient medical history
The patient was a 67-year-old internal medicine specialist who had six spine surgeries over the last 22 years. Beside her cervical spine problems, she was fit, healthy and slim. She first underwent cervical spine surgery in 1998 with a Frykholm procedure at C6/C7. Four years later she had another Frykholm procedure at C3/C4, followed shortly by an anterior cage stand-alone fusion procedure at C3/4. In 2015 she underwent a cage stand-alone anterior decompression and fusion at C5/C6 and C6/C7. Another 2 years later she had total disc prosthesis at C4/C5, and finally 16 months ago a posterior stabilization from C2 to C4.
Complaints
When the patient was seen for the first time in February 2020, she complained of significant load-dependent neck pain (Visual Analog Scale [VAS] score: 6 points) and an awful crepitation. She also reported bilateral arm pain (VAS score: 5 points), radiating to the ulnar side. She scored 30 points on the Neck Pain Disability Index. With neck flexion she experienced pain relief but also some tingling in her legs. The patient had tried to reduce her pain by conservative means including physiotherapy, massage, acupuncture, and multimodal pain treatment including continuous morphine therapy, but she did not improve substantially.
Clinical evaluation
Clinically, the patient had local pressure pain in the motion segments C4/5, C5/6, and especially C7/Th1 accompanied by a C8 radiculopathy on both sides. The slim neck and the muscle atrophy allowed an easy palpation of the posterior implants that was painful on the right side. Neurological and neurophysiological evaluation confirmed C8 root compression and residual myelopathic changes with prolonged Medianus-SEPs and MEPs. The ear, nose, and throat evaluation was within the reference range.
Radiographic evaluation
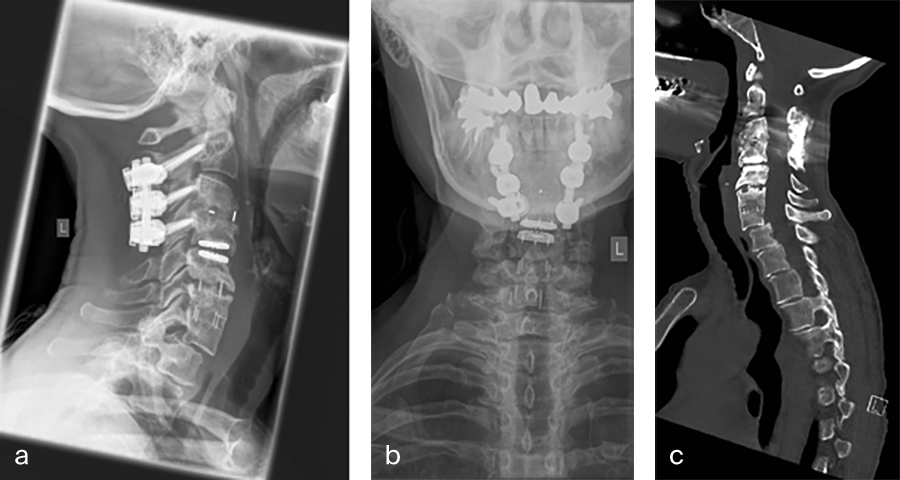
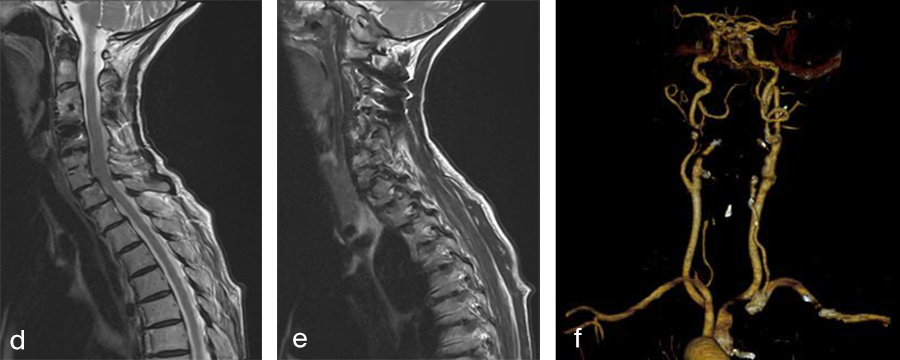
Her preoperative radiographic evaluation comprised x-rays, functional x-rays, computed tomographic, and magnetic resonance imaging scans (Fig 4) and demonstrated:
- A fusion of the motion segments C2/3/4 and C6/7
- A moderate implant loosening of the posterior C2 screw on the right side
- An afunctional disc prosthesis at the level C4/C5 with significant heterotopic ossifications (grade III) accompanied by a facet joint osteoarthritis in this motion segment
- A nonunion at the level C5/C6 with residual mobility in this motion segment
- A highly mobile degenerative spondylolisthesis at the level C7/Th1 with bilateral neuroforaminal stenosis
Preoperative imaging (Fig 4a-f), showing:
- C2-C4 posterior instrumentation and fusion.
- Anterior fusion after Anterior Cervical Decompression and Fusion (ACDF) C3/4 and C6/7.
- Status after total disc replacement of C4/5 with heterotopic ossifications.
- Nonunion C5/6 after ACDF C5/6.
- Spondylolisthesis C7/Th1 with neuroforaminal stenosis on both sides.
- A normal cervical angiogram (cave: artefacts).
Surgery
Based on the findings detailed above and the patient's excruciating pain, an anterioposterior revision surgery was performed in June 2020.
First, a C7/Th1 ACDF was performed via a left-sided approach. After decompression of the spinal canal and bilateral neuroforaminal decompression of the C8 nerve route, stabilization was achieved with a stand-alone Syncage-C (DPS) that already significantly reduced the spondylolisthesis.
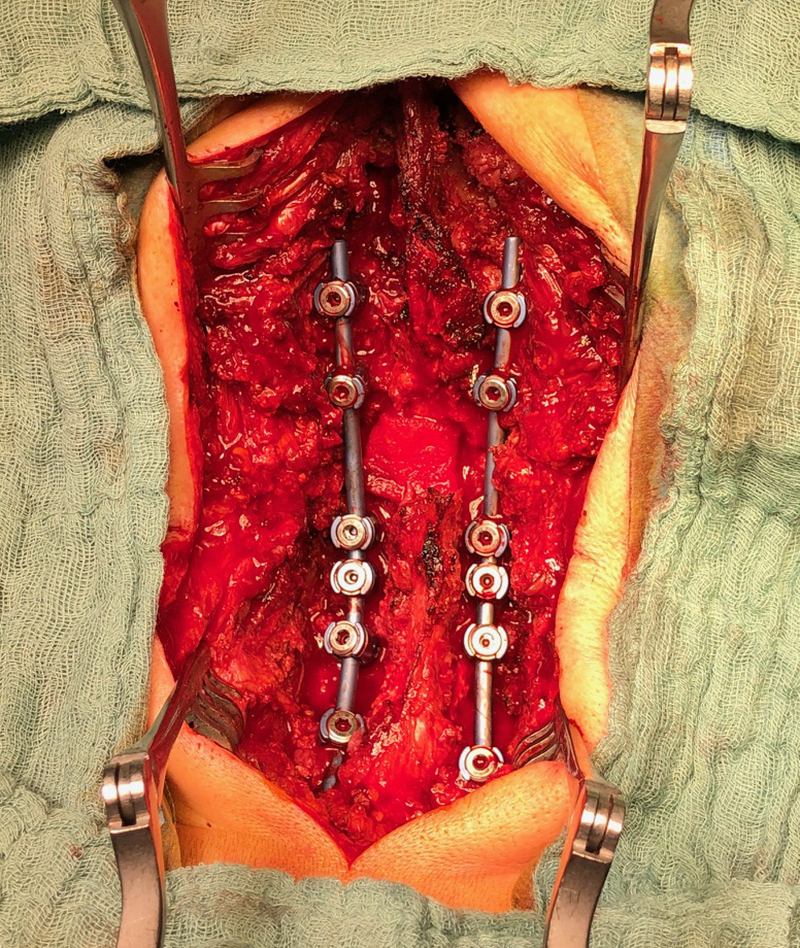
Second, a posterior revision surgery was performed including implant removal of the posterior instrumentation between C2 and C4 followed by a laminectomy of C7 with bilateral foraminotomy of the C8 nerve routes. Re-instrumentation with isthmic screws at the level C2, lateral mass screws at the level C4, C5, and C6, as well as bilateral pedicle screws at the level T2 and T3 was performed using the new Symphony system (DPS). The Symphony system offered the opportunity to place 4.0 mm screws in the previous loosened screw location at the level C2. The 3.5 mm screws were placed in C4, C5, and C6, and 5.5 and 5.0 mm screws at T2 and T3, respectively. The 4.0 mm rod allowed a good direct connection between the cervical spine isthmic and lateral mass screws and the thoracic pedicle screws, providing adequate stability and allowing excellent reduction. An intraoperative image is shown in Fig 5. Postoperative x-ray evaluations are displayed in Fig 6ae.
Postoperative course
The patient improved significantly postoperatively with regard to her C8 radiculopathy, which had already disappeared the day after surgery. Her neck pain also improved significantly and on the day of discharge from the hospital (day 5 after surgery) she only needed analgesic medication (administration of 600 mg ibuprofen three times daily).
At 6-week postoperative follow-up, the patient was taking 600 mg ibuprofen once daily for a good night's sleep and she was satisfied with the postoperative course (VAS neck pain score: 2; arm pain score: 0). Hence, her rehabilitation program was started.
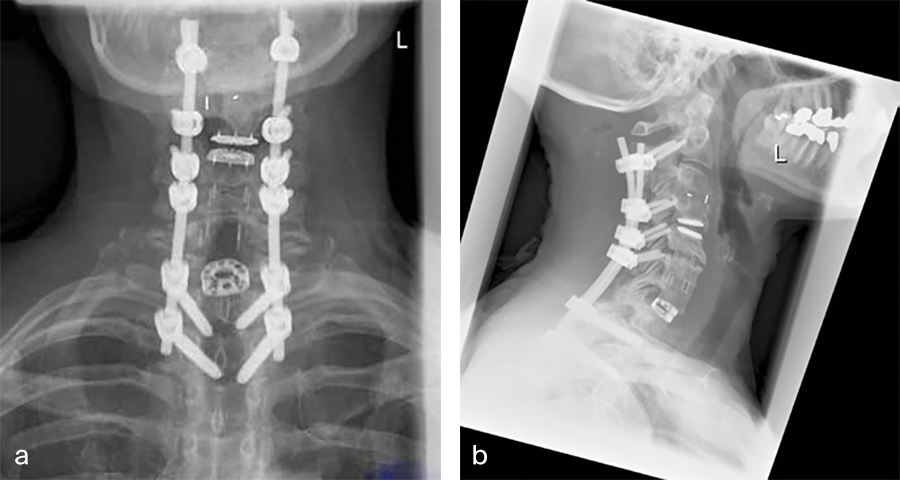
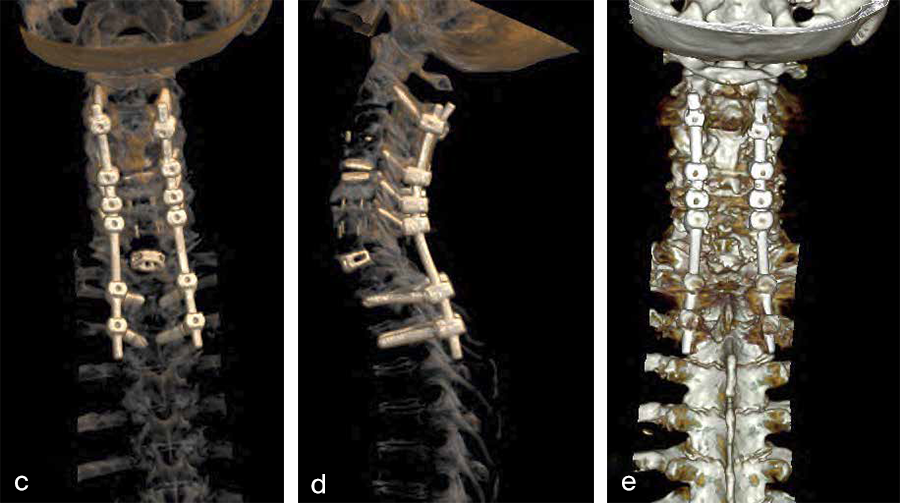
Postoperative imaging (Fig 6a-e), showing:
AC DF C7/Th1 (Syncage C) and posterior stabilization with Symphony of C2, C4, C5, C6, Th1, and Th2 using 3.5 (C4/5/6) 4.0 (C2), 5.0 (TH2) and 5.5 mm (Th1) screws and 4.0 rods.
Symphony—Occipito-Cervico-Thoracic System
Hazards and labeling
Due to varying countries’ legal and regulatory approval requirements, consult the appropriate local product labeling for approved intended use of the products described on this website. All devices on this website are approved by the AO Technical Commission. For logistical reasons, these devices may not be available in all countries worldwide at the date of publication.
Legal restrictions
This work was produced by AO Foundation, Switzerland. All rights reserved by AO Foundation. This publication, including all parts thereof, is legally protected by copyright.
Any use, exploitation or commercialization outside the narrow limits set forth by copyright legislation and the restrictions on use laid out below, without the publisher‘s consent, is illegal and liable to prosecution. This applies in particular to photostat reproduction, copying, scanning or duplication of any kind, translation, preparation of microfilms, electronic data processing, and storage such as making this publication available on Intranet or Internet.
Some of the products, names, instruments, treatments, logos, designs, etc referred to in this publication are also protected by patents, trademarks or by other intellectual property protection laws (eg, “AO” and the AO logo are subject to trademark applications/registrations) even though specific reference to this fact is not always made in the text. Therefore, the appearance of a name, instrument, etc without designation as proprietary is not to be construed as a representation by the publisher that it is in the public domain.
Restrictions on use: The rightful owner of an authorized copy of this work may use it for educational and research purposes only. Single images or illustrations may be copied for research or educational purposes only. The images or illustrations may not be altered in any way and need to carry the following statement of origin “Copyright by AO Foundation, Switzerland”.
Check www.aofoundation.org/disclaimer for more information.
If you have any comments or questions on the articles or the new devices, please do not hesitate to contact us.
“approved by AO Technical Commission” and “approved by AO”
The brands and labels “approved by AO Technical Commission” and “approved by AO”, particularly "AO" and the AO logo, are AO Foundation's intellectual property and subject to trademark applications and registrations, respectively. The use of these brands and labels is regulated by licensing agreements between AO Foundation and the producers of innovation products obliged to use such labels to declare the products as AO Technical Commission or AO Foundation approved solutions. Any unauthorized or inadequate use of these trademarks may be subject to legal action.
AO ITC Innovations Magazine
Find all issues of the AO ITC Innovations Magazine for download here.
Innovation Awards
Recognizing outstanding achievements in development and fostering excellence in surgical innovation.