FIBULINK Syndesmosis Repair System
Michael Swords, Tim Schepers, Matthew Tomlinson, Christina Kabbash
Adequate treatment of syndesmotic injuries is important to restore ankle function and prevent poor clinical outcomes. Accuracy and maintenance of syndesmosis reduction are considered key factors for a successful treatment. The most common operative treatment method is syndesmotic screw fixation. Syndesmotic screws provide rigid fixation but inhibit the natural tibiofibular movement. Screw breakages are frequently observed. Suture button devices have been developed for “dynamic” syndesmosis fixation with the claimed benefits of allowing physiological motion of the distal tibiofibular joint.
The FIBULINK™ Syndesmosis Repair System combines the benefits of fixation of a screw and the flexibility of a suture. It is the first adjustable syndesmotic repair system to enable precise, anatomical syndesmotic fixation. The fixation concept addresses limitations of suture button constructs including lack of tension control and medial soft-tissue disruption.
The FIBULINK Syndesmosis Repair System is available in stainless steel and titanium. It can be used in combination with a fibula plate.
The system is compatible with the following DePuy Synthes plate holes:
- 1/3 tubular plate holes (LCP and non-locking)
- Non-threaded portion of a combi hole in a 2.7 mm/3.5 mm LCP Distal Fibula Plate
- Syndesmotic slots of a 2.7 mm VA-LCP Lateral Distal Fibula Plate
Additionally, the FIBULINK Implant is compatible with any distal fibula plate hole which accepts a 4 mm non-locking cortex screw.
Clinical problem
The ligaments around the syndesmosis maintain the proper relationship between the distal fibula and tibia. As such, they provide strong stabilization and dynamic support to the ankle mortise. Syndesmotic injuries occur in 1–18% of all ankle sprains, and 13–50% of all ankle fractures [1]. Based on data obtained from eight US states in 2009, Vosseler et al [2] reported an incidence rate of 2.09 syndesmotic injuries per 100,000 person-years. This incidence would correlate to about 7000 such injuries in the US in 2020. Syndesmotic injuries tend to occur in younger patients (between 18 and 34 years), which adds to the burden of disease because of the potential of productive years of life lost secondary to disability from this injury [2].
Proactive recognition and adequate treatment of syndesmotic injuries are important to restore ankle function and prevent poor clinical outcomes including degenerative ankle disease. Unstable syndesmotic injuries typically require surgical stabilization [3, 4]. Accuracy and maintenance of syndesmosis reduction are considered key factors for a successful treatment. If an associated fracture is present, the length, alignment, and the rotation of the fibula must be restored before syndesmotic reduction and fixation.
Historically, the most common operative treatment method is syndesmotic screw fixation. Syndesmotic screws provide rigid fixation but inhibit the natural physiological tibiofibular movement. Screw breakages are frequently observed [5, 6]. A second operation might be required for screw removal which is associated with substantial costs [7]. Lalli et al [8] stated that their institution billed a total of $188,271 for elective syndesmosis hardware removal in 56 patients. In 2012 a national survey [9] including 86 hospitals in the Netherlands revealed that syndesmotic screw removal was routinely done by 87% of the surgeons. There has been disagreement in the literature whether syndesmotic screws should be retained or removed. Timing of removal is also debated [4]. An argument in favor of screw removal is the restoration of the physiological syndesmosis function and the normal load transfer in the ankle joint.
Suture button devices have been developed for “dynamic” syndesmosis fixation with the claimed benefits of allowing physiological motion of the distal tibiofibular joint, reducing the implant breakage rate observed in rigid screw fixation and avoiding routine implant removal. Their use has become increasingly popular due to these appealing device features. Sanders et al [10] in a randomized controlled study compared two 3.5 mm 3-cortex screws with a frequently used suture button device (Syndesmosis TightRope®, Arthrex, Naples, Fla) for syndesmosis fixation. The reoperation rate was significantly higher in the group with screws (30%) than in the TightRope group (4%), largely due to elective removal of screw fixation [10]. Additionally, malreduction rate (2 mm translation or 10° rotation threshold) was 39% in the group with screws compared with 15% in the TightRope group [10]. A randomized trial [11] compared suture button fixation (48 patients) and fixation with a single quadricortical syndesmotic screw (49 patients) for syndesmosis injury. At 2 years, the median American Orthopedic Foot and Ankle Society (AOFAS) score was higher in the suture button group than in the syndesmotic screw group (96 vs 86), as was the median Olerud-Molander Ankle score (100 vs 90) [11]. In a randomized controlled trial Ræder et al [12] found no differences in the AOFAS score at 2 years (median AOFAS score was 97 in both groups) after treatment with single tricortical 3.5 mm syndesmotic screw fixation (n = 47) and suture button fixation (n = 48). A systematic review [13] of the treatment for acute syndesmotic injuries found that the implant removal rate of TightRope was lower compared with that of syndesmotic screws, but still amounted to 10% (in 220 patients).
Several drawbacks have been reported for TightRope fixation: superficial wound infection, chronic osteomyelitis, irritation from the suture knots, and creeping button migration/bony subsidence [4]. A study from Pirozzi et al [14] showed that there is a considerable risk of entrapment of superficial medial neurovascular structures. The authors advised that a medial incision should be used to ensure that these structures are not entrapped. LaMothe et al [15] concluded that in simulated highly unstable injuries a single suture button placed from the lateral fibula to the anterior medial malleolus allowed significantly more posterior motion of the fibula (and sagittal plane instability) than a syndesmotic screw. Additionally, TightRope devices are not indicated as sole fixation in length unstable patterns as they do not reliably prevent shortening from occurring [16]. A technical drawback of suture button instrumentation is the limited capability to reverse or fine tune the amount of tensioning in the system which may cause inadequate syndesmosis reconstruction.
The Foot and Ankle Expert Group (FAEG) and DePuy Synthes (DPS) investigated alternative concepts for syndesmosis repair to address the issues of syndesmotic screw and suture button fixation for treatment of syndesmotic injuries.
Solution
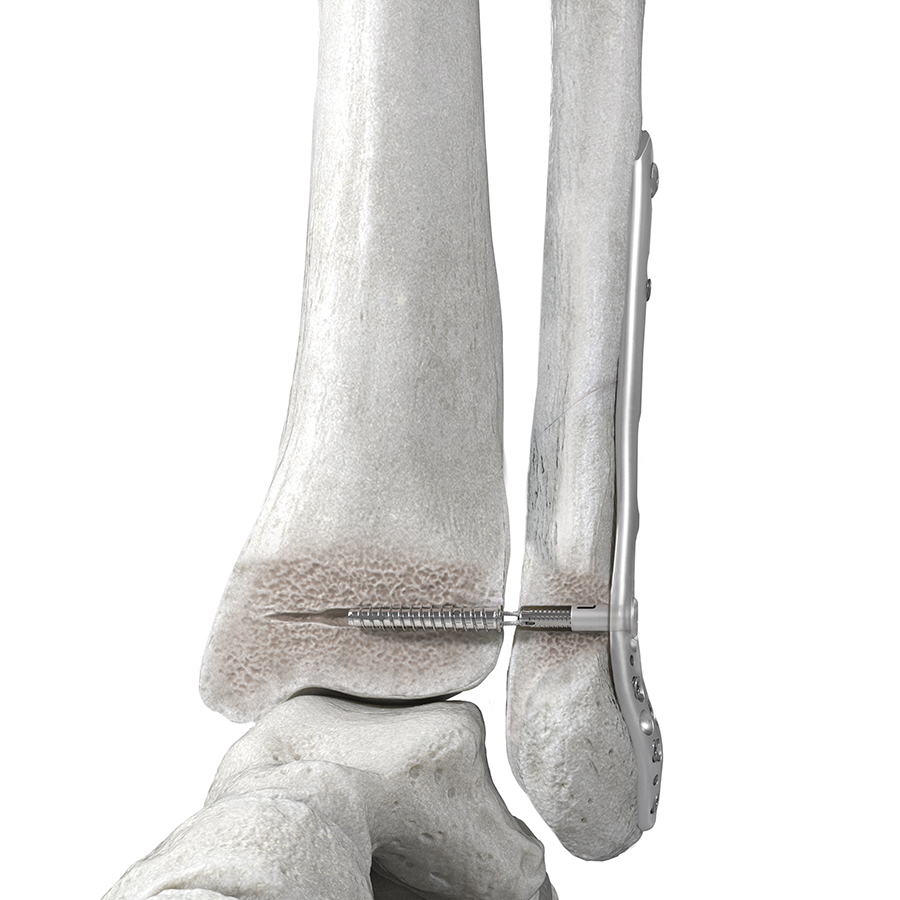
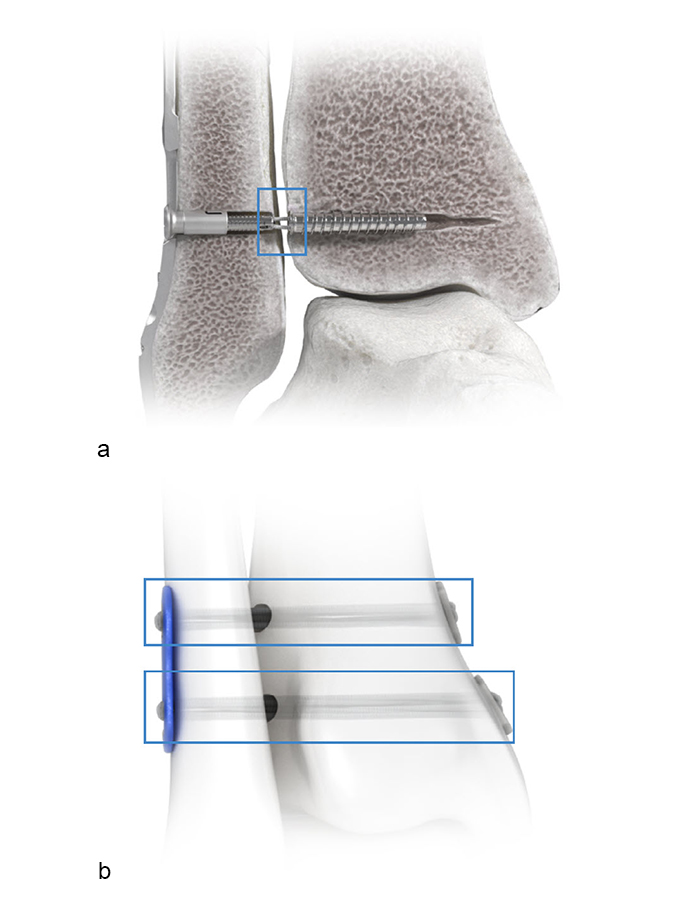
The FIBULINK™ Syndesmosis Repair System (Fig 1) combines the benefits of fixation of a screw and the flexibility of a suture. A short, high-strength suture bridge helps to restore the physiologic ankle motion.
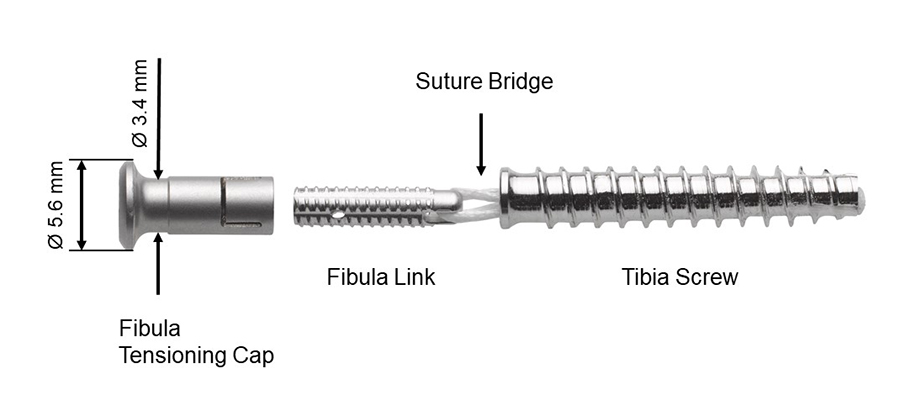
The implant is a multicomponent anchor system consisting of four main components (Fig 1):
- Fibula Tensioning Cap: interfaces with the Fibula Link. A rotation of the Tensioning Cap applies tension to the construct.
- Fibula Link: transfers the tension applied by the Fibula Tensioning Cap to the Suture Bridge. As such, it functions as an interface in the primary tension mechanism.
- Suture Bridge: applies compression between the fibula and the tibia via transferring the tension between the Fibula Link and the Tibia Screw. The 4 mm long Suture Bridge consists of four strands of #1 Ultra High Molecular Weight Polyethylene.
- Tibia Screw: functions as an anchor in the tibia.
Fibulink Syndesmosis Repair System components
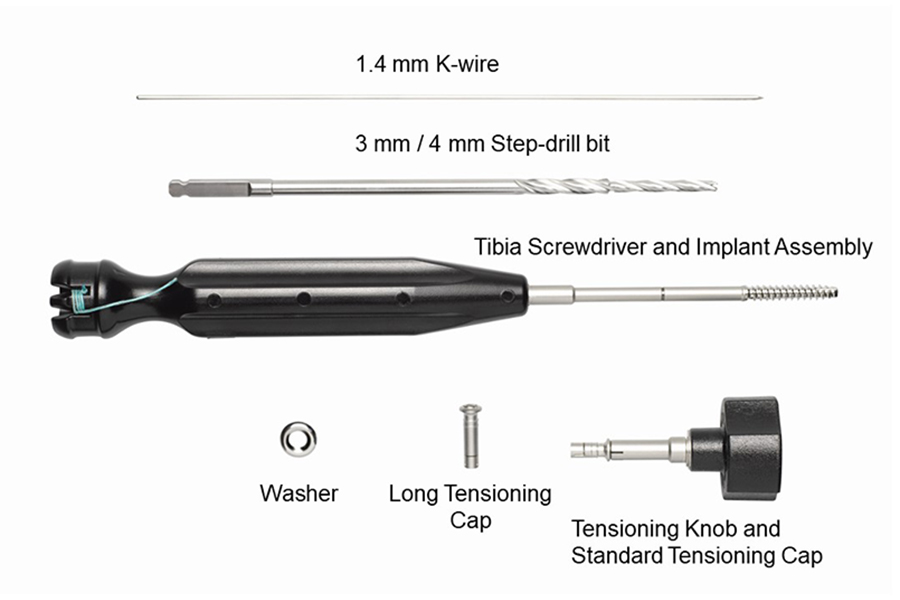
The implant components and instruments are provided in sterile, single-use kits (Fig 2). The standard Fibula Tensioning Cap is preattached to the Tensioning Knob. The self-tapping Tibia Screw is preloaded to the Tibia Screwdriver.
Key points of insertion
The 1.4 mm K-wire must be placed in appropriate position. Either in the center of the fibula and directed slightly anterior into the tibia, or - if used with a plate - through the center of the plate hole to allow free passage of the device. The step-drill bit should be advanced with caution to avoid penetration into the tibia. The tibia screw must be inserted until just flush with the lateral cortex of the tibia. Internal and external oblique imaging with the C-arm may be necessary to confirm appropriate depth of insertion.
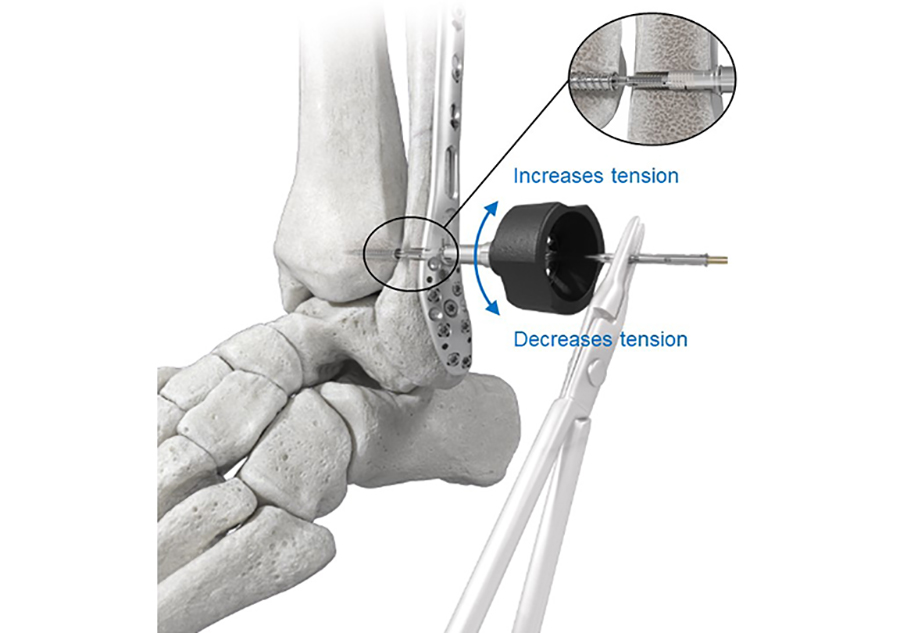
The Tensioning Knob is used to fine tune and readjust the tension in the Suture Bridge intraoperatively (Fig 3). Clockwise or counterclockwise rotation of the Tensioning Knob will advance or reverse the Fibula Tensioning Cap, thereby adjusting the tension in the suture bridge in a two-way tension control to achieve the desired level of correction.
The FIBULINK fixation concept does not require medial soft-tissue disruption and helps improve procedural efficiency by delivering fixation through a single lateral incision. Since it does not rely on hardware placement on the medial tibia it eliminates medial side complications, such as damage to neurovascular structures and soft-tissue entrapment associated with suture button constructs. It also limits interference with the placement of additional hardware on the medial side (eg, medial malleolar screws), which might be required because of the injury (eg, high-energy injury).
The short, high-strength suture bridge (Fig 4) enables physiological motion by spanning the distance between the medial side of the fibula and the lateral side of the tibia. Suture button constructs typically rely on long suture bridges between the lateral side of the fibula and the medial side of the tibia. The long suture distance can lead to suture toggling and tunnel widening compromising the fixation stability and changing the syndesmosis gap.
Biomechanical testing
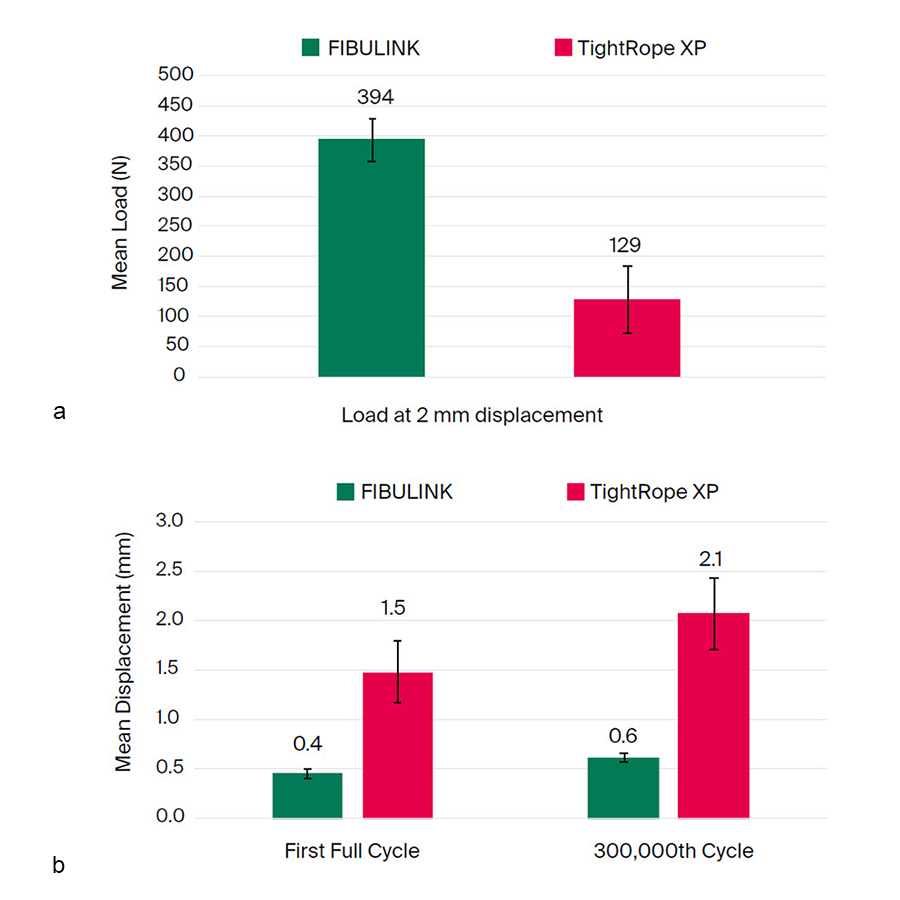
Bench testing was performed in a poor-quality bone model to compare the fixation strength provided by the FIBULINK Syndesmosis Repair System and Arthrex Syndesmosis TightRope® XP Implant System. Eight samples in each group were cyclically loaded in the direction of the fixation from 20 N to 113 N for 300,000 cycles. Displacements in load direction (elongation of the device) were recorded. After cyclic loading, a static load to failure test was executed. The load at 2 mm displacement was determined as measure for the fixation strength because the fibula displacement difference of 2 mm or more medial to lateral is pathological [17–21].
The FIBULINK Syndesmosis Repair System provided three times higher fixation strength (load at 2 mm displacement) than TightRope XP (Fig 5a). The elongation of the TightRope XP at 300,000 cycles was 3.5 times higher compared with the one of the FIBULINK Syndesmosis Repair System (Fig 5b).
Indications
The FIBULINK Syndesmosis Repair System is currently only available in the US with the following indication statement:
The FIBULINK Syndesmosis Repair System is intended as an adjunct in fracture repair involving metaphyseal and periarticular small bone fragments where screws are not indicated and as an adjunct to fixation systems involving plates, with fracture braces and casting. Specifically, the FIBULINK Syndesmosis Repair System is intended to provide fixation during the healing process following a syndesmotic trauma, such as fixation of syndesmosis (syndesmosis disruptions) in connection with Weber B and C ankle fractures.
References
1. Desai S. Syndesmotic injuries treated with an aperture fixation device. Techniques Foot Ankle Surg. 2020;19(2):96–103.
2. Vosseller JT, Karl JW, Greisberg JK. Incidence of syndesmotic injury. Orthopedics. 2014 Mar;37(3):e226–229.
3. Corte-Real N, Caetano J. Ankle and syndesmosis instability: consensus and controversies. EFORT Open Rev. 2021 Jun 28;6(6):420–431.
4. Vopat ML, Vopat BG, Lubberts B, et al. Current trends in the diagnosis and management of syndesmotic injury. Curr Rev Musculoskelet Med. 2017 Mar;10(1):94–103.
5. Behery OA, Mandel J, Solasz SJ, et al. Patterns and implications of early syndesmotic screw failure in rotational ankle fractures. Foot Ankle Int. 2020 Sep;41(9):1065–1072.
6. Lehtola R, Leskelä HV, Flinkkilä T, et al. Suture button versus syndesmosis screw fixation in pronation-external rotation ankle fractures: a minimum 6-year follow-up of a randomised controlled trial. Injury. 2021 Jul 2;S0020–1383(21):00588-X.
7. Neary KC, Mormino MA, Wang H. Suture button fixation versus syndesmotic screws in supination-external rotation type 4 injuries: a cost-effectiveness analysis. Am J Sports Med. 2017 Jan;45(1):210–217.
8. Lalli TA, Matthews LJ, Hanselman AE, et al. Economic impact of syndesmosis hardware removal. Foot (Edinb). 2015 Sep;25(3):131–133.
9. Schepers T, van Zuuren WJ, van den Bekerom MP, et al. The management of acute distal tibio-fibular syndesmotic injuries: results of a nationwide survey. Injury. 2012 Oct;43(10):1718–1723.
10. Sanders D, Schneider P, Taylor M, et al. Improved reduction of the tibiofibular syndesmosis with tight rope compared with screw fixation: results of a randomized controlled study. J Orthop Trauma. 2019 Nov;33(11):531–537.
11. Andersen MR, Frihagen F, Hellund JC, et al. Randomized trial comparing suture button with single syndesmotic screw for syndesmosis. J Bone Joint Surg Am. 2018 Jan;100(1):2–12.
12. Ræder BW, Stake IK, Madsen JE, et al. Randomized trial comparing suture button with single 3.5 mm syndesmotic screw for ankle syndesmosis injury: similar results at 2 years. Acta Orthop. 2020 Dec;91(6):770–775.
13. Schepers T. Acute distal tibiofibular syndesmosis injury: a systematic review of suture-button versus syndesmotic screw repair. Int Orthop. 2012 Jun;36(6):1199–1206.
14. Pirozzi KM, Creech CL, Meyr AJ. Assessment of anatomic risk during syndesmotic stabilization with the suture button technique. J Foot Ankle Surg. 2015 Sep-Oct;54(5):917–919.
15. LaMothe JM, Baxter JR, Murphy C, et al. Three-dimensional analysis of fibular motion after fixation of syndesmotic injuries with a screw or suture-button construct. Foot Ankle Int. 2016 Dec;37(12):1350–1356.
16. Riedel MD, Miller CP, Kwon JY. Augmenting suture-button fixation for Maisonneuve injuries with fibular shortening: technique tip. Foot Ankle Int. 2017 Oct;38(10):1146–1151.
17. Hunt KJ. Syndesmosis injuries. Curr Rev Musculoskelet Med. 2013 Dec;6(4):304–312.
18. Ramsey PL, Hamilton W. Changes in tibiotalar area of contact caused by lateral talar shift. J Bone Joint Surg Am. 1976 Apr;58(3):356–357.
19. Wilson FC Jr, Skilbred LA. Long-term results in the treatment of displaced bimalleolar fractures. J Bone Joint Surg Am. 1966 Sep;48(6):1065–1078.
20. Brodie IA, Denham RA. The treatment of unstable ankle fractures. J Bone Joint Surg Br. 1974 May;56(2):256–262.
21. Joy G, Patzakis MJ, Harvey JP. Precise evaluation of the reduction of severe ankle fractures: technique and correlation with end results. J Bone Joint Surg Am. 1974 Jul;56(5):979–993.
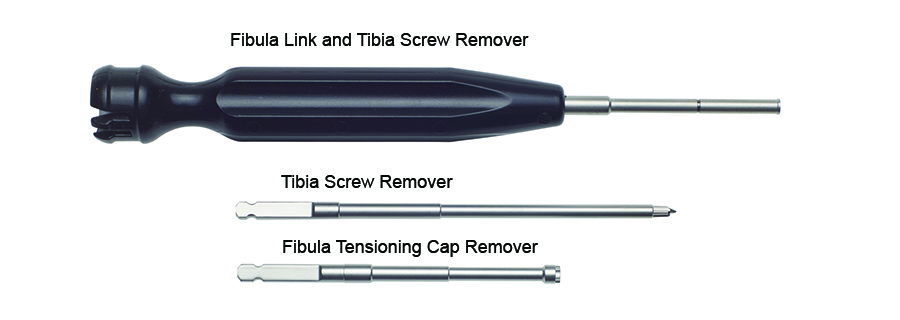
Removal
There is a dedicated removal kit available for implant removal (Fig 1). Removal of the implant is completed by reversing the installation steps.
Clinical case series
In a case series of 14 patients (mean age: 48 years; age range: 26–77 years; eight men and six women) the FIBULINK Implant was used to treat nine supination external rotation; two pronation external rotation; one Maisonneuve; and two isolated syndesmotic injuries [1]. The mean AOFAS score at follow-up (average: 9.5 months) was 94. It varied slightly by type of injury, gender, and age (range: 87–100 years). Isolated syndesmosis and Maisonneuve injuries had the highest AOFAS scores. There were no instances of loss of reduction, hardware removal, repeat surgeries, wound issues, or other complications.
Reference
1. Desai S. Syndesmotic injuries treated with an aperture fixation device. Techniques Foot Ankle Surg. 2020;19(2):96–103.
Clinical cases from Michael Swords (Michigan Orthopedic Center, Lansing, Mich, US)
Case 1
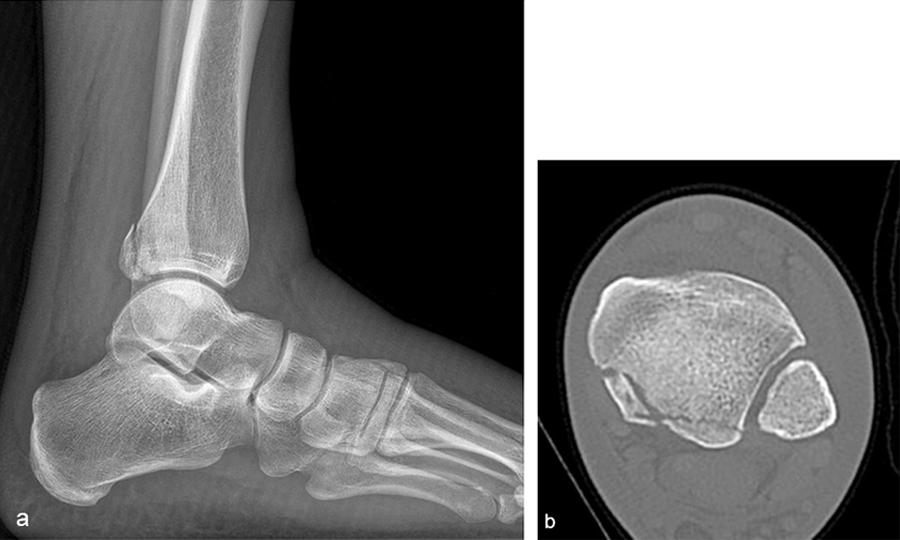
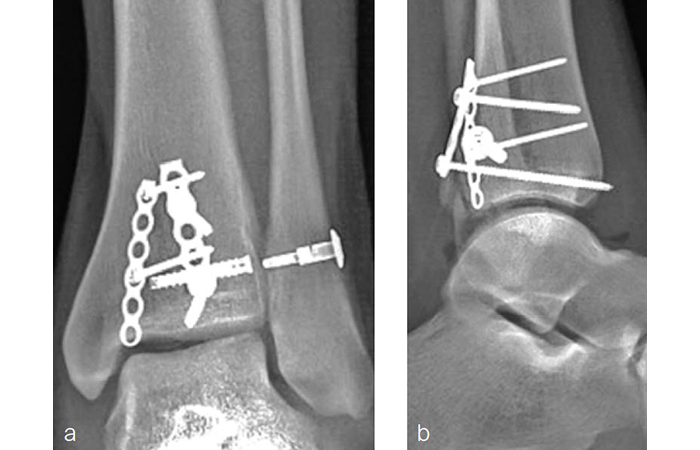
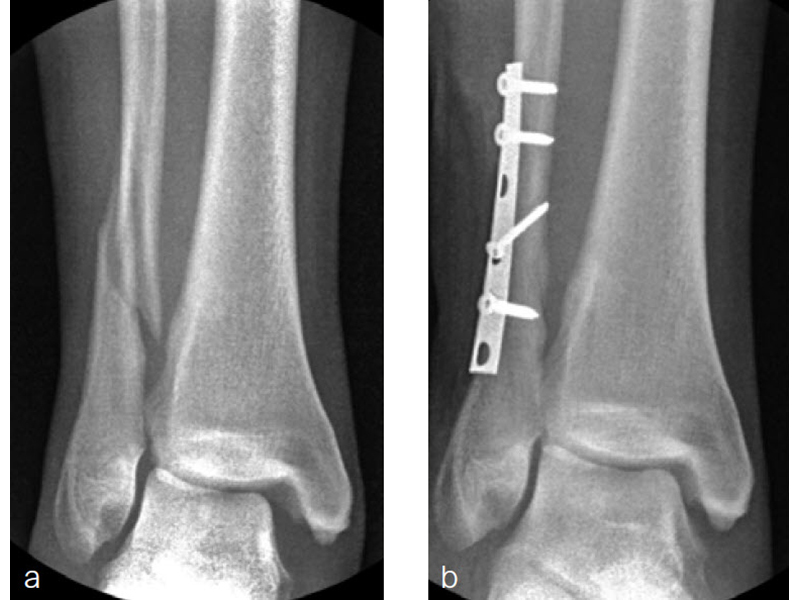
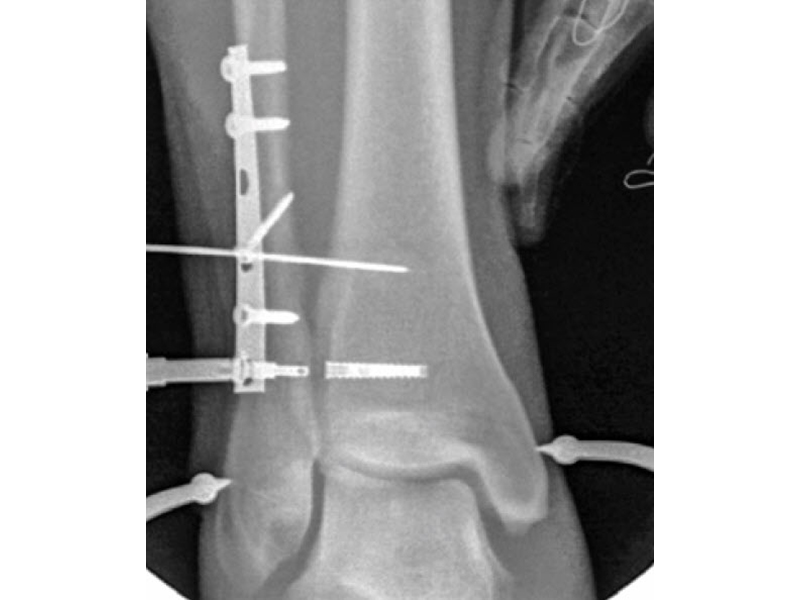
A 27-year-old man fell from a ladder sustaining a proximal fibula fracture (Fig 1) with a multipart posterior malleolar fracture (Fig 2). The patient was treated operatively with direct reduction and plate fixation of the posterior malleolar components. Intraoperative testing demonstrated continued syndesmotic instability requiring fixation (Fig 3). The syndesmosis was reduced in direct fashion and stabilized with a provisional K-wire and clamp before insertion of a FIBULINK Implant (Fig 4).
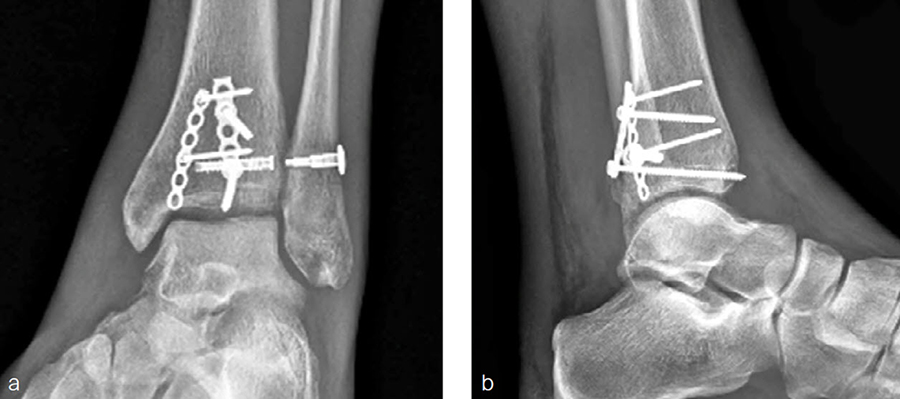
The patient healed (Fig 5) and returned to preoperative function.
Case 2
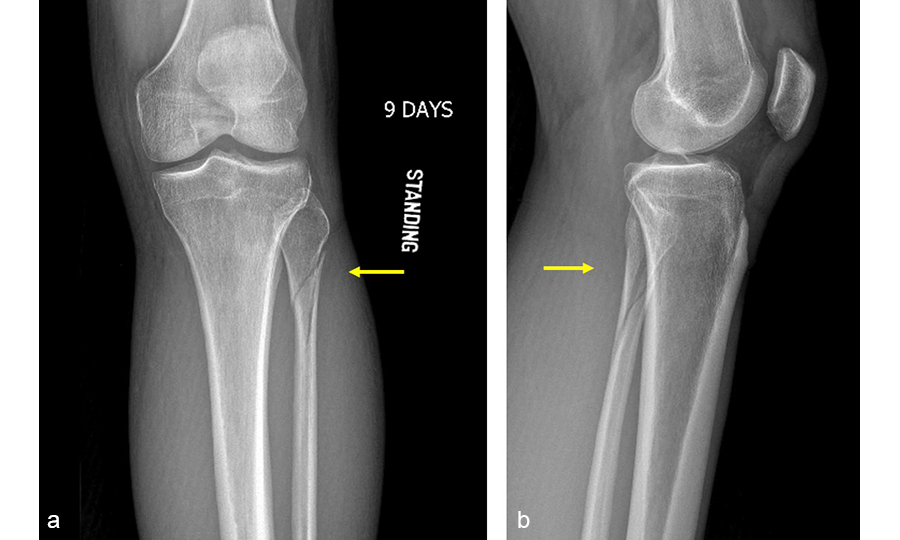
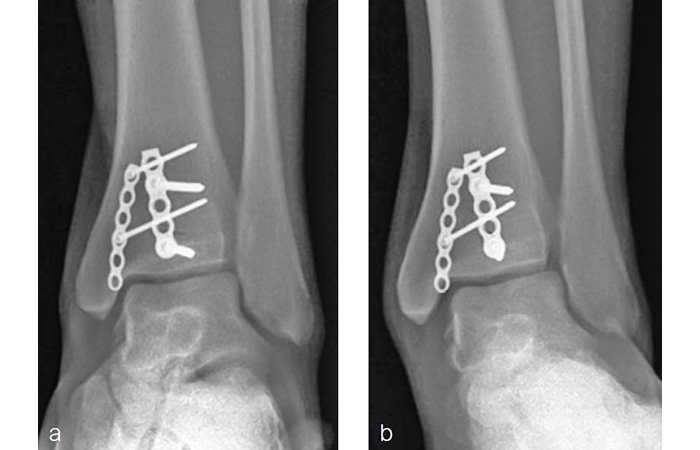
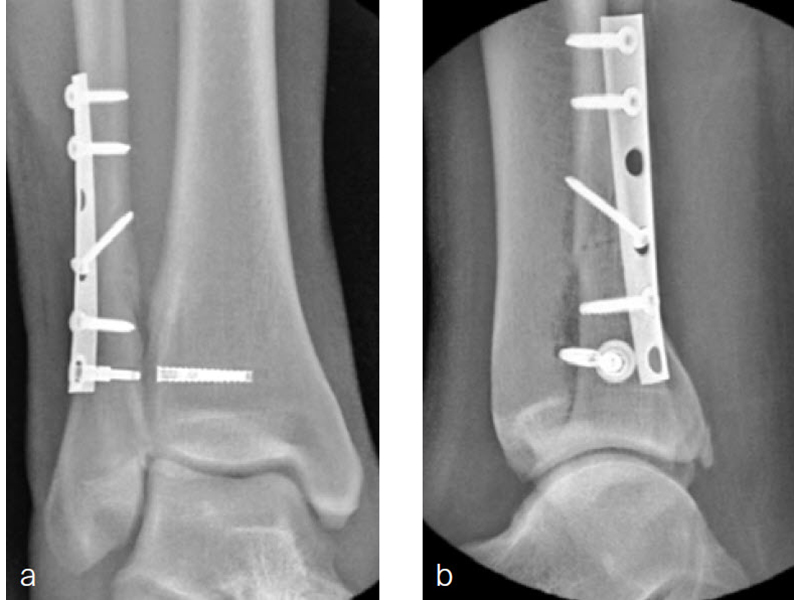
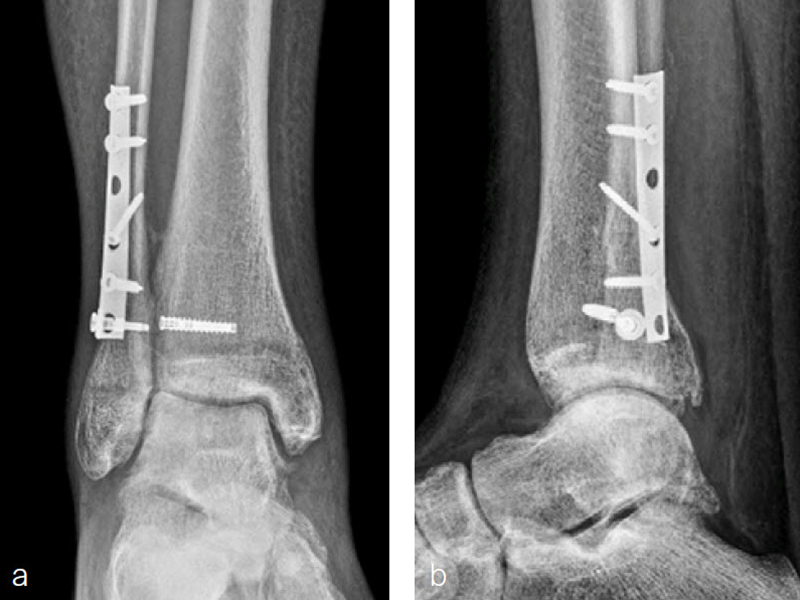
A 34-year-old woman was injured while riding a motor scooter sustaining an ankle fracture with associated syndesmotic injury (Fig 6a). The fibula was reduced anatomically and stabilized with a 1/3 tubular plate (Fig 6b). The unstable syndesmosis was reduced and provisionally stabilized with a K-wire and clamp (Fig 7) before FIBULINK Implant System implantation (Fig 8). The patient had an uneventful recovery (Fig 9).
Innovations in treatment of syndesmotic injuries
Hazards and labeling
Due to varying countries’ legal and regulatory approval requirements, consult the appropriate local product labeling for approved intended use of the products described on this website. All devices on this website are approved by the AO Technical Commission. For logistical reasons, these devices may not be available in all countries worldwide at the date of publication.
Legal restrictions
This work was produced by AO Foundation, Switzerland. All rights reserved by AO Foundation. This publication, including all parts thereof, is legally protected by copyright.
Any use, exploitation or commercialization outside the narrow limits set forth by copyright legislation and the restrictions on use laid out below, without the publisher‘s consent, is illegal and liable to prosecution. This applies in particular to photostat reproduction, copying, scanning or duplication of any kind, translation, preparation of microfilms, electronic data processing, and storage such as making this publication available on Intranet or Internet.
Some of the products, names, instruments, treatments, logos, designs, etc referred to in this publication are also protected by patents, trademarks or by other intellectual property protection laws (eg, “AO” and the AO logo are subject to trademark applications/registrations) even though specific reference to this fact is not always made in the text. Therefore, the appearance of a name, instrument, etc without designation as proprietary is not to be construed as a representation by the publisher that it is in the public domain.
Restrictions on use: The rightful owner of an authorized copy of this work may use it for educational and research purposes only. Single images or illustrations may be copied for research or educational purposes only. The images or illustrations may not be altered in any way and need to carry the following statement of origin “Copyright by AO Foundation, Switzerland”.
Check www.aofoundation.org/disclaimer for more information.
If you have any comments or questions on the articles or the new devices, please do not hesitate to contact us.
“approved by AO Technical Commission” and “approved by AO”
The brands and labels “approved by AO Technical Commission” and “approved by AO”, particularly "AO" and the AO logo, are AO Foundation's intellectual property and subject to trademark applications and registrations, respectively. The use of these brands and labels is regulated by licensing agreements between AO Foundation and the producers of innovation products obliged to use such labels to declare the products as AO Technical Commission or AO Foundation approved solutions. Any unauthorized or inadequate use of these trademarks may be subject to legal action.
AO ITC Innovations Magazine
Find all issues of the AO ITC Innovations Magazine for download here.
Innovation Awards
Recognizing outstanding achievements in development and fostering excellence in surgical innovation.